Article Series: Understanding Physiology When Developing Medical Simulation
HealthySimulation.com writer, Dr. Kim Baily, guest authored a series of articles that discuss the importance of understanding physiology when developing medical simulation experiences. Although simulation in healthcare incorporates knowledge from many disciplines, perhaps the most pervasive information comes from physiology. Simulation team members may have a limited background in physiology or medicine. These articles provide a more thorough explanation of basic physiological concepts that can enable non medical simulationists to better understand medical simulation.
Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 1: Blood Pressure
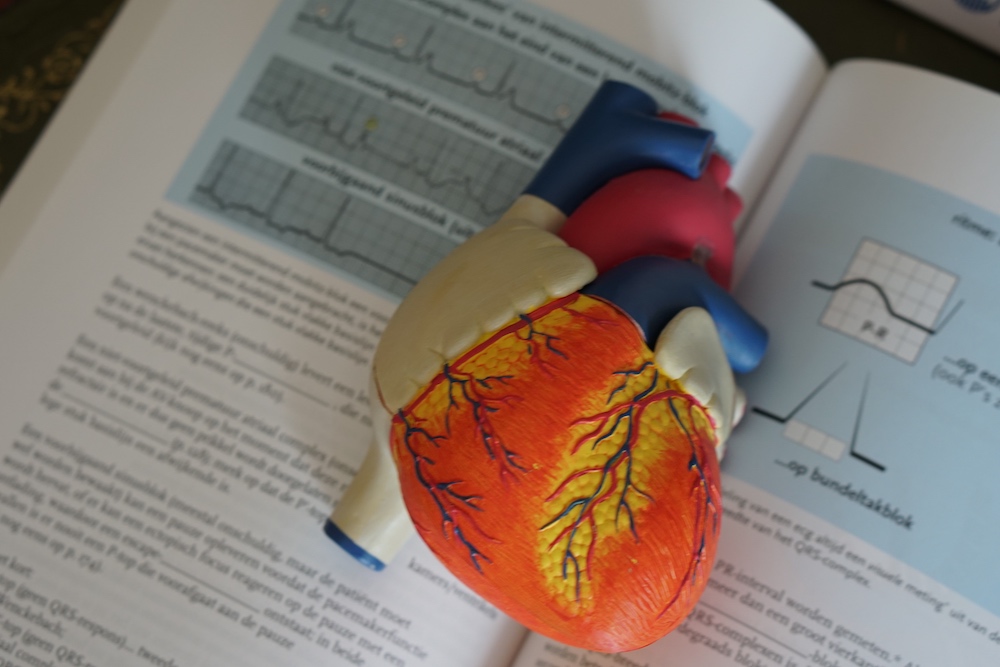
Some simulation team members may have a limited background in physiology or medicine. An understanding of basic physiological concepts can enable non medical simulationists to better understand medical simulation. Physiology is defined as the study of how the body works. Given that there are trillions of chemical reactions going on in the human body at any moment of time, beginning a discussion on physiology may seem an impossible task. There are, however, some general concepts that are helpful in understanding some of the basics.
Sponsored Content:
Some simulation team members may have a limited background in physiology or medicine. An understanding of basic physiological concepts can enable non medical simulationists to better understand medical simulation. This article is the second in a series of posts related to physiology, the force behind simulation. This post covers vital signs – heart rate (pulse), respiratory rate, and temperature.
Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 3: Pulse Oximetry
Although traditional vital sign measurement includes blood pressure, temperature, pulse (heart rate) and respirations, a fifth vital sign pulse oximetry (oxygen saturation) is now widely used to provide information on blood oxygen levels. As all body tissues need oxygen, measurement of oxygen levels can provide vital information about the oxygenation status of a patient. An arterial blood gas (ABG) can provide detailed information about oxygenation, ventilation, and acid-base levels; however, an ABG is an invasive procedure that provides a single snapshot of the patient’s condition. The advantage of pulse oximetry is that it can measure blood oxygen saturation non-invasively and continuously.
Sponsored Content:
Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 4: Diabetes
Diabetic patients are prone to fluctuating blood sugars which must be treated promptly to prevent serious consequences. Diabetes can be incorporated into any existing scenario thereby increasing the complexity of the scenario. Alternatively, a significant change in blood glucose levels can form the basis of a standalone scenario.
This article takes a closer look at Hypoglycemia and blood sugars. All diabetic patients in hospital should be covered by a hypoglycemic protocol. The adult treatment depends on the patients level of consciousness and IV access. The hypoglycemia template located within this article may be adapted to match any facility. Running a sim with a matching policy is desirable; however, if students from different clinical sites will run through the same sim, let learners review the policy before the simulation.
Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 4C: Insulin
Scenarios can be created for learners at different levels. For example, for novice learners, routine blood sugar testing before meals and at bedtime accompanied by appropriate insulin administration is a good place to start. This article discusses patient education and helping newly diagnosed patients face the onset of a chronic disease creates a challenging scenario for learners. Scenarios can incorporate children and teens as patients.
Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 5: Sepsis
As timely diagnosis and intervention of sepsis are key factors in preventing mortality, simulation provides a unique opportunity to prepare clinicians and students in the identification and treatment of sepsis. This article, which includes basic information about the definition, cause, risk factors, and pathophysiology of sepsis, is intended for simulation team members whose background is non-medical or for those who need a refresher.
The key to developing a realistic healthcare simulation experience is to understand how physiological functions change in response to various stimuli (stressors). Learners are more likely to focus on desired learning objectives when they participate in life-like scenarios and receive information which is consistent with the clinical situation being studied. This article discusses the physiological basics of Hypovolemia.
Learners are more likely to focus on desired learning objectives when they participate in life-like scenarios and receive information which is consistent with the healthcare situation being studied. This article also covers the physiological response, treatment and incorporation of hypovolemia into simulation. For example, cardiac output and blood pressure depend on circulating blood volume. As volume is lost, physiological mechanisms switch on to maintain blood pressure and ensure that tissues and organs are supplied with the oxygen they need. Clinicians must assess signs and symptoms to determine the severity of blood loss and the required treatment.
Healthcare simulation technical staff are often very knowledgeable about computer technology or film production, but may be less knowledgeable about the physiological principles which underlay medical simulation scenarios. This article highlights common IV fluids found in clinical practice and provides Excel templates for IV labels.
Understanding IV Site Access for Healthcare Simulation, with Assessment Template
Intravenous fluid (IV) and medication administration is often a necessary component of patient care even though there are potential hazards associated with this type of therapy. Healthcare Simulation scenarios involving IV fluids or medications should attempt to mimic real life situations as much as possible. When learners have to frequently “pretend” to perform tasks, they may spend unnecessary time wondering if the lack of fidelity is part of the simulation or a normal component of simulation learning.
Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 7C: PCA for Pain
Patient Controlled Analgesia (PCA) allows patients to manage their pain by self-administering small doses of intravenous analgesia within set limits. This article discusses PCA pain management buttons and how they can be used in medical simulation. The PCA mode of therapy minimizes the roller-coaster effects of peaks of sedation and valleys of pain that occur with the traditional method of PRN dosing.
Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 8: ABGs
The more closely healthcare simulation matches real life situations (aka fidelity), the more likely that learners will become involved in the learning experience and be less confused. In the clinical setting, healthcare practitioners review past labs or order new ones to help make decisions about appropriate patient care. Lab results should be included in healthcare simulation scenarios where appropriate. Adding lab results provides learners with potentially missing pieces of data that would normally be available. Medical Simulation technologists often come from technical backgrounds with limited knowledge of physiology. By increasing basic physiological knowledge, simulation technicians can add to their understanding of medicine and become more fully involved in simulation operations, research, and development.
As sepsis and septic shock with subsequent multi-organ failure are the leading causes of death in adult intensive care units (ICUs), most healthcare simulation programs should consider medical simulation scenarios that educate and train on the topic. This article takes a deeper dive into understanding Sepsis Labs.
Read the Entire Physiology: The “Force” Behind Healthcare Simulation HealthySimulation.com Article Series:
- Part 1: Blood Pressure
- Part 2: Heart & Respiratory Rate
- Part 3: Pulse Oximetry
- Part 4: Diabetes
- Part 4B: Hypoglycemia & Excel Template for Simulated EHR
- Part 4C: Insulin
- Part 5: Sepsis
- Part 6A: Hypovolemia (Intro)
- Part 6B: Hypovolemia (Treatment & Simulation Tips)
- Part 7A: IV Fluids & Bags
- Part 7B: IV Pumps & Site Access
- Part 7C: PCA for Pain
- Part 8: ABGs
- Part 9: Sepsis Labs
Watch HealthySimulation.com Webinar “Understanding Basic Physiology for Clinical Simulation”
Lance Baily, BA, EMT-B, is the Founder & CEO of HealthySimulation.com, which he started while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas back in 2010. Lance is also the Founder and acting Advisor to the Board of SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife Abigail Baily, PhD live in Las Vegas, Nevada with their two amazing daughters.
Sponsored Content: