Simulation Lab
A simulation lab is designed to provide immersive learning experiences for healthcare practitioners and students. A simulation center, which consists of a realistic clinical sim lab rooms, manikins and equipment, allow learners to practice and develop clinical expertise without any risk of patient harm. Also called a Sim Lab, learners utilize these spaces to apply their theoretical knowledge in carefully created hands-on scenarios that mimic various clinical situations inside these simulation laboratories. These scenarios range in complexity and/or skill level. For example, healthcare simulation may be used for undergraduate medical and nursing schools, internships, residencies and training programs for qualified practitioners. Some examples of healthcare simulation scenarios include asthma attacks in pediatric patients, GI bleed, labor and delivery complications, cardiac arrest and newborn hypoxia. In addition, medical simulation provides a unique opportunity for hospital staff and students to practice team communication, interdisciplinary care and patient safety.
Clinical Simulation Lab spaces may be divided into three main areas:
- Prebriefing space: Information is provided to the learners about a patient situation. A review of standards may be included.
- Simulation Lab space: Where a scenario case study with specific learning outcomes which can be reproduced with a high fidelity patient simulator, other medical simulators or Standardized Patient actors. Learners, who assume a variety of healthcare roles, must respond to the scenario as if they were with a real patient. Additional learners may watch and listen either through a one-way mirror or remotely via a live video transmission
- Debriefing space: Learners review and reflect on their actions in the scenario, identify what went well and not so well (aka practice gaps) and ways to improve future performance. Debriefing is a key component of simulation education where the learners themselves consider their own behaviors, learn from the experience, change future behaviors and become better healthcare practitioners.
The greater the realism (fidelity) of the clinical simulation scenario and environment within the simulation laboratory to real life, the more likely the learners will suspend disbelief and immerse themselves as if they are in a real life clinical case.
Sponsored Content:
Simulation labs are built to mimic various hospital locations such as emergency rooms, operation theaters, critical care units, labor and delivery rooms, general medical-surgical floors (wards) and pediatric intensive care units. Some academic healthcare institutions and hospitals have a single simulation lab with or without separate debriefing and control rooms. Healthcare simulation programs use a simulation lab environment so there is a protected learning space and the ability to change clinical equipment around to match the desired learning outcomes.
HealthySimulation.com is dedicated to providing the latest Simulation Lab news and nursing simulation resources from around the world. To follow along, sign up for our free medical simulation email newsletter, follow @HealthySim on Twitter and @HealthySim on Facebook, or join our HealthySimulation.com LinkedIn Company Page!
Large simulation centers have a cluster of medical sim labs or nursing sim labs, along with clinical simulation debriefing rooms, control rooms, preparation rooms and storage rooms. In addition, there may be patient examination rooms, separate labs for task trainers and surgical simulators as well as classrooms and computer rooms for computer assisted learning and virtual reality. This environment allows for a variety of modalities of healthcare simulation to be delivered as well as a variety of levels of fidelity as well.
Sponsored Content:
Simulation labs contain a variety of specialized patient manikins (models), electronics and audio video equipment. The quantity and type of equipment depends on the learning needs of the participants, the available space and the budget to operate, build, maintain and staff each laboratory.
Simulation Lab Equipment Examples
-
- Human Patient Simulators or manikins: Simulate symptoms and diseases.
- Examples: SimMan from Laerdal, Noelle from Gaumard, HPS from Elevate Healthcare
- Fidelity – the degree of realism to which the manikin mimics physiological functions
- High Fidelity Simulators – Patient manikins that mimic many complex biological systems such as cardiac and respiratory functions, measurable blood pressure, palpable pulses, EKG displays, pulse oximeter, arterial waveforms, pulmonary artery waveforms and anesthetic gasses.
- Possible interventions e.g. bag-mask ventilation, intubation, defibrillation, chest tube placement, cricothyrotomy and others.
- Manikins are computerized, contain hydraulics and compressors and have external monitors which display various physiological waveforms.
- Specialized manikins such as trauma manikins, birthing manikins, newborn, premature babies and pediatric manikins.
- Mid-fidelity – limited number of physiological characteristics such as cardiac and respiratory indicators.
- Audio-video equipment such as cameras, microphones and speakers. This equipment is used in the scenario to provide information to the learners involved in the scenario, to relay sound and video to learners who watch in other rooms and to record and playback the scenario for debrief at the completion of the scenario.
- Bedside computers for access to simulated electronic health records and lab results.
- Human Patient Simulators or manikins: Simulate symptoms and diseases.
-
- Medication administration devices
-
- Headwalls – typically mimics those found in hospitals – may contain oxygen and air outlets, suction, lights, diagnostic equipment such as blood pressure cuffs and sphygmomanometers.
- Additional Medical Room Equipment:
- Crash carts
- EKG machines and other diagnostic equipment
- Anesthesia equipment
- Surgical instruments
- Ventilators
- Defibrillators
- Telephone
- Furniture such as hospital bed, over-the-bed table, bedside cabinet, crib, bassinet, baby-warmer etc.
- Equipment and medical supplies to be used in the scenario e.g. IV catheterization supplies and chest tubes.
View the LEARN CE/CME Platform Webinar A Room with a View: Maximizing Low Cost Sim Lab Outcomes to learn more!
Considerations To Build a Simulation Lab
Clearly to design and build a simulation lab takes much preparation and a plan. All stakeholders such as facilities, IT and pharmacy should be consulted and involved in the initial phases. Learning outcomes and learner levels should be identified as well as budget and available space. Faculty development is key to ensure that healthcare simulation programs are successful. High fidelity patient simulators will go unused if faculty do not understand healthcare simulation pedagogy such as clinical simulation scenario development and debriefing.
Budget is required for healthcare simulation technologists to operate, maintain, repair and replace equipment as the equipment becomes obsolete. Annual maintenance contracts are helpful but costly. Budget for healthcare simulation program managers and administrative staff should also be included and considered. There is always the risk with the purchase of expensive high fidelity manikins and then the manikin sits rarely used in a cupboard. The purchase of a high fidelity manikin alone is not enough to make a healthcare simulation program successful. Less expensive mid-fidelity patient manikins may work very effectively for some healthcare simulation programs.
Simulation Lab Benefits
The use of a nursing simulation lab has increased dramatically in the past 15 to 20 years. The benefits of healthcare simulation to improve medical education is now well documented. Clinical expertise comes with practice and experience of the management of an array of clinical situations. Clinical Sim Labs provide the ideal learning space where healthcare professionals of all levels can practice and improve their clinical skills without any potential harm to patients.
A simulation lab provides a protected environment for healthcare simulation to be able to occur. In situ clinical simulation is great as this provides the opportunity to be able to test the clinical environment. This also allows the opportunity to find potential latent safety threats in clinical environments and reduce harm and risk of errors to patients in clinical care. This also allows healthcare staff to be able to practice and hone their clinical care in a real clinical environment.
However, there are many challenges to in situ clinical simulation. Clinical simulation which is delivered in situ can be canceled due to a lack of bed space availability or clinical staff are pulled back into clinical workload demands. A simulation lab is a protected space and ready made environment which is always ready to be able to deliver healthcare simulation based education.
Sim Lab Latest News

Dr. Pam Jeffries Upcoming Webinar on Developing Healthcare Simulation Centers to Create Realistic Clinical Scenarios!
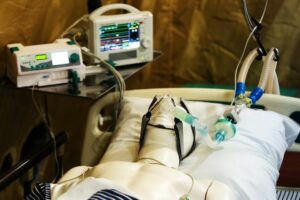
How to Run a Clinical Simulation Program Without a Simulation Center

Healthcare Simulation Sustainability: Reuse, Refill, Recycle, Request
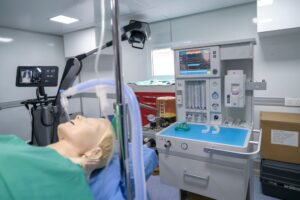
Sim-Zones: Sistema de Organización para el Aprendizaje Basado en Simulación Clínica

How Automation is Advancing Quality Healthcare Simulation

New Clinical Simulation Center Updates | January 2022
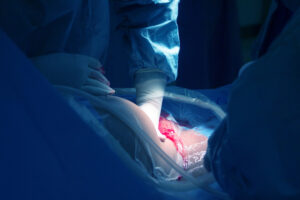
How to Run a Postpartum Hemorrhage Nursing Simulation Scenario

Celebrating the Holiday Season Across Healthcare Simulation

Healthcare Simulation Scenarios: Why Preparation is Essential for Learners

New Clinical Simulation Center Updates | September 2022

How Simulation Centers Can Expand Use and Support Innovation

Healthcare Simulation Escape Room Tips & Tricks | Part 1
Sponsored Content:














