Standardized Patient
A Standardized Patient (SP) is an individual who has been trained to portray the role of either a patient, family member or others in a consistent, standardized manner for the educational benefit of a healthcare learner or professional. Outside of the United States SPs are commonly referred to as Simulated Patients. Standardized Patients can be thought of as the “actors and actresses” within the realm of healthcare education and medical simulation.
Medical schools and other healthcare educational institutions will utilize SPs to teach and assess their learners throughout their coursework. Students are always told they will be working with SPs and are expected to act as though they are examining real patients. For administrators, Standardized Patients offer a lifelike simulated scenario without the risks associated with using actual patients.
The conceptual origin of the Standardized Patient dates back to 1963, when Dr. Howard S. Barrows MD, a neurologist and medical educator, created the first standardized patient in 1963 for his third-year neurology clerkship while teaching at the University of Southern California. By directly observing the students, Barrows and the physician SP realized that a number of skills were being incorrectly performed because students were unaware of the inaccuracy. Barrows also experienced difficulties when he tried to find patients with specific findings for Psychiatry and Neurology board examinations for and realized that some findings could be simulated. Thus Barrows was inspired to create his first “simulated patient.” The birth of the simulated patient came out of a need for a more comprehensive method to evaluate the clinical skills of third-year medical students. In the 1960s, Barrows’ innovative teaching and assessment methodologies were not widely accepted amongst his peers but eventually they would become the standard for educating and training specialties within healthcare!
Sponsored Content:
What does a Standardized Patient do?
In many cases, the programs that employ Standardized Patients train them to best represent another person’s actual patient case to base their simulated experience upon. The Simulated Patient may then be interviewed or examined by the learners as though they were that person in the doctor’s office or other healthcare setting. This means that SPs should be able to provide a full patient history and simulate their physical signs (such as pain or difficulty walking).
While Standardized Patients are not permitted to take any blood or other samples, they are able to perform a number of other, more general tasks. Common exercises that learners may perform during an examination include:
- Listening to the heart and lungs with a stethoscope
- Pressing on the abdomen looking for tenderness or swellings
- Looking into eyes, ears and throat
- Taking blood pressure
- Assessing muscle strength
- Checking reflexes
- Checking pulses
Some SPs are comfortable with more invasive medical exams like pelvic exams or chest exams, and are compensated at higher rates for allowing medical professionals to train on these delicate procedures.
Sponsored Content:
These roles are essential within academia and training so that learners have the opportunity to practice their healthcare skills, communication skills, history and record keeping skills on a physical patient prior to treating actual patients. Treating a Standardized Patient further provides learners with insight into how to prepare for patients in varying conditions.
Teaching learners about the appropriate ways to examine a patient is critical to helping build their confidence and performance in the field–especially when performing more challenging exams. For this reason, gynecological, breast and genitourinary exams are always monitored by a faculty member.
To serve their purpose, Standardized Patients must be carefully recruited and trained to take on the characteristics of the real patient being simulated. This thereby affords learners the opportunity to learn and to be evaluated on skills in a controlled and simulated clinical environment. In this setting, they are less apprehensive and can be subjected to feedback at each step. Sometimes SPs where specialized makeup called moulage to better represent the signs and symptoms of the patient they are portraying. The most famous video regarding SPs is from the character of Kramer on Seinfeld who worked as a Standardized Patient in one episode.
How do Standardized Patients Benefit Clinical Simulation?
Typically, there are a number of set interactions that a Standardized Patient can expect to have with the learner they are working with. For example, during one of their interactions, the SP may present case histories in response to a question the learner has. They may also undergo a limited physical examination at the learner’s discretion.
At other times, a Standardized Patient may be asked to provide learners with necessary medical news and information, or they can be matched with cases using specific criteria. These criteria can include factors such as age, gender, race, etc.
Alternatively, during an interaction with a learner a SP may be asked to help them work on and develop their interpersonal communication and clinical skills. Assisting a learner in working through difficult emotional situations within a healthcare environment is another benefit of this guided simulation. Simulated Patients serve a much greater purpose than simply to serve as a simulated body.
Each experience utilizing a SP as a tool is designed to be as realistic as possible and to enhance the total learning experience. However, the mission of the SP Program is not to have a Standardized Patient realistically convey an illness to a student, but to instead offer an educational tool that is both consistent and measurable for review.
By doing this, programs are able to accurately teach and assess students according to one standard per case. The stronger the standards put into place, the more accurately a case can be reproduced.
Who is an ideal Standardized Patient?
Those interested in contributing to the development of health care professionals may apply to be chosen to work as SPs through facilities and institutions which rely on their services. While some may think having worked as an actor would be similar to serving as a Standardized Patient, there are clear differences. For instance, the work of an SP can be extremely repetitive and observant.
Making the role of a Standardized Patient increasingly unique is that they are usually asked to balanced and objective feedback, and stay flexible to the needs of the faculty in each situation. Due to the nature of the work, an SP is not permitted to share their learning material with those outside of the program or other healthcare personnel involved.
The act of portraying someone with a certain medical condition or issue is safe, and the examinations are normally very basic. If there is ever a point where the Standardized Patient may be subject to any discomfort, they are warned and are able to opt out of participating in that examination.
Individuals who are interested in healthcare and helping students learn and navigate their way through the field are ideal SP applicants. Many Standardized Patients find this role extremely rewarding, in addition to being interesting.
If committed to becoming a Standardized Patient, individuals can expect to spend a minimum of 15 hours in training sessions with a Standardized Patient Trainer. The amount of time that will be needed for further training will vary depending on the complexity of each case and the SP’s experience.
Having no biases toward gender, race, religion, national origin, or physical characteristics is essential for all Standardized Patients. They should also be professionals who are able to understand and respect confidential matters. Being comfortable healthcare is another plus in this role.
Overall, men and women of all ages can serve as Standardized Patients. Prospective SPs should always be upfront about any preexisting conditions, as they can either help or prohibit the individual from participating in certain cases. Being a strong communicator, who can learn quickly, accept direction and adapt easily to a variety of different situations is also largely beneficial as a Standardized Patient.
About the Association for Standardized Patient Educators (ASPE)
ASPE is the international organization of simulation educators dedicated to: promoting best practices in the application of SP methodology for education, assessment and research, fostering the dissemination of research and scholarship in the field of SP methodology, and advancing the professional knowledge and skills of its members.
Standardized Patient Latest News

Healthcare Simulation Research June 2024

Global Medical Simulation Industry News Update June 2024

2024 ASPE Annual Conference

Global Medical Simulation News Update April 2024

AvMentor Provides Standardized Patient Program Development, Training & Services

Enhancing Healthcare Simulation-Based Education with High-Fidelity Standardized Patients

Women in Leadership Virtual Event Empowers Clinical Simulation Community
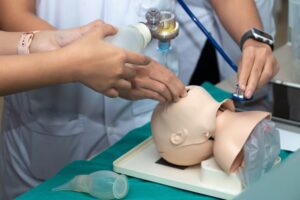
Developing a Healthcare Simulation for the Novice Simulation Educator

Latest Clinical Simulation News From Around the World | March 2023

How Healthcare Simulation Can Help Mitigate Workplace Violence
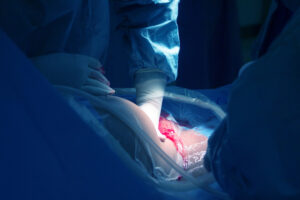
How to Run a Postpartum Hemorrhage Nursing Simulation Scenario
Sponsored Content:















