Healthcare Simulation Standards of Best Practice
The International Nursing Association for Clinical Simulation and Learning (INACSL) has developed the “INACSL Standards of Best Practice: Simulation” to advance the science of simulation, share best practices, and provide evidence-based guidelines for implementation and training. Developing a set of best practices can help any healthcare simulation flourish, as these guidelines help promote successful learning and training outcomes. These Standards provide a detailed process for evaluating and improving simulation operating procedures and delivery methods that every simulation team will benefit from. Adoption of the “INACSL Standards of Best Practice: Simulation” demonstrates a commitment to quality and implementation of rigorous evidence-based practices in healthcare education to improve patient care by complying with practice standards.
INACSL begins these recommendations by explaining that the early development of simulation-based education was largely provided by equipment managers. Now, more attention is being paid to the “pedagogy underlying the practice.” Further, a more participant-centered and evidence-based approach has helped the field mature as a whole. This progression is what ultimately has led to the need for professional standards and the recognition by regulatory bodies that simulation – necessary for continued professional development.
Through the publication of these guiding criteria, professionals can more easily set expectations for individuals and simulation programs to demonstrate adherence to professional SBE standards. Although roles and responsibilities vary from institution to institution, based on organizational resources and the previous experience, knowledge, and skills of the simulationist, all professional development standards provide a roadmap.
Sponsored Content:
In 2022, INACSL established a Healthcare Simulation Standards Endorsement to recognize healthcare institutions and practices that have demonstrated excellence in applying all four clinical simulation standards from the Healthcare Simulation Standards of Best Practice (HSSOBP) in their educational simulation programs. The four standards include Prebriefing: Preparation and Briefing, Facilitation, Professional Integrity, and Debriefing.
Standards of Best Practice
You can find the latest Standards by INACSL here.
Professional Development
Initial and ongoing professional development supports the simulationist across their career. As the practice of simulation-based education grows, professional development allows the simulationist to stay current with new knowledge, provide high-quality simulation experiences, and meet the educational needs of the learners.
Sponsored Content:
Criteria Necessary to Meet this Standard
- Perform an educational needs assessment that includes a gap analysis to provide the foundational evidence for a well-designed professional development plan.
- Participate in professional development activities that address desired learning outcomes and align with an individual’s role and the priorities of the institution.
- Reevaluate the professional development plan on a regular basis using formative and summative methods by both the individual and the organization.
Prebriefing
Prebriefing information prior to simulation-based experiences is vital for learner success and may enhance debriefing and reflection. Deliberately designed preparation and prebriefing can balance the cognitive load demands of the learner and increase the effectiveness of the simulation-based experience. The high-quality simulation requires simulationists and educators who are knowledgeable in pedagogy, including the prebriefing phase.
Criteria Necessary to Meet This Standard
- The simulationist should be knowledgeable about the scenario and competent in concepts related to prebriefing.
- Prebriefing should be developed according to the purpose and learning objectives of the simulation-based experience.
- The experience and knowledge level of the simulation learner should be considered when planning the prebriefing.
Simulation Design
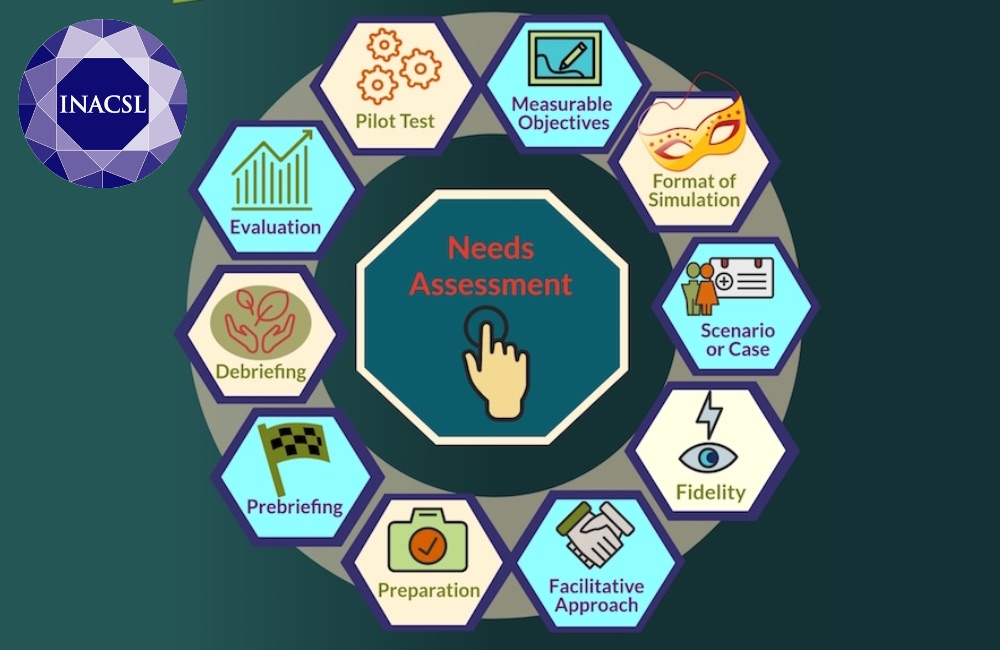
Simulation-based experiences are purposefully designed to meet identified objectives and optimize the achievement of expected outcomes. All simulation-based experiences require purposeful and systematic yet flexible and cyclical planning. To achieve expected outcomes, their design and development should consider criteria that facilitate their effectiveness. Following this standard supports the development of relevant/ educationally sound simulation-based experiences.
Criteria Necessary to Meet this Standard
- Simulation-based experiences (SBE) should be designed in consultation with content experts and simulationists knowledgeable in best practices in simulation education, pedagogy, and practice.
- Perform a needs assessment to provide the foundational evidence of the need for a well-designed simulation-based experience.
- Construct measurable objectives that build upon the learner’s foundational knowledge.
- Build the simulation-based experience to align the modality with the objectives.
- Design a scenario, case, or activity to provide the context for the simulation-based experience.
- Use various types of fidelity to create the required perception of realism.
- Plan a learner-centered facilitative approach driven by the objectives, learners’ knowledge and level of experience, and the expected outcomes.
- Create a prebriefing plan that includes preparation materials and briefing to guide participant success in the simulation-based experience.
- Create a debriefing or feedback session and/or a guided reflection exercise to follow the simulation-based experience.
- Develop a plan for evaluation of the learner and of the simulation-based experience.
- Pilot test simulation-based experiences before full implementation.
Facilitation
Facilitation of a simulation-based experience requires a facilitator who has the education, skill, and ability to guide, support and seeks out ways to assist participants in achieving expected outcomes. To maintain skill as an effective facilitator, one must pursue continuing education and assessment of his/her facilitation skills. The selection of a facilitation method is guided by theory and research. Facilitation methods may vary based on the levels of the participants, the simulation objectives, and the context of the simulation-based experience while considering cultural and individual differences that affect participants’ knowledge, skills, attitudes, and behaviors.
Criteria Necessary to Meet This Standard
- Effective facilitation requires a facilitator who has specific skills and knowledge in simulation pedagogy.
- The facilitative approach is appropriate to the level of learning, experience, and competency of the participants.
- Facilitation methods before the simulation-based experience include preparatory activities and a prebriefing to prepare participants for the simulation-based experience (Follow the Healthcare Simulation Standards of Best PracticeTM (HSSOBPTM) Prebriefing: Preparation and Briefing).
- Facilitation methods during a simulation-based experience involve the delivery of cues (predetermined and/or unplanned) aimed to assist participants in achieving expected outcomes.
- Facilitation after and beyond the simulation-based experience aims to support participants in achieving expected outcomes.
Debriefing
Learning is dependent on the integration of experience and reflection. The evidence is clear that essential learning occurs in the debriefing phase of the simulation-based experience. Reflection is the conscious consideration of the meaning and implication of an action, which includes the assimilation of knowledge, skills, and attitudes with pre-existing knowledge. Reflection can lead to new interpretations by the participants; cognitive reframing is essential to learning. The skills of the debriefer are important to ensure the best possible learning outcomes.
Criteria Necessary to Meet This Standard
-
- The debrief is facilitated by a person(s) competent in the process of debriefing.
- The debrief is conducted in an environment that is conducive to learning and supports confidentiality, trust, open communication, self-analysis, feedback, and reflection.
- The debrief is facilitated by a person(s) who can devote enough concentrated attention during the simulation to effectively debrief the simulation-based experience.
- The debrief is based on a theoretical framework for debriefing that is structured in a purposeful way.
- The debrief is congruent with the objectives and outcomes of the simulation-based experience.
Operations & Translations
Simulation operations encompass the infrastructure, people, and processes necessary for the implementation of an effective and efficient simulation-based education (SBE) program. The interactions of these pieces must form a system that integrates with larger educational and healthcare entities to realize the goals of SBE. SBE is no longer an adjunct to health care training and/or professional development programs but an all-inclusive integrated program requiring business acumen and technically knowledgeable personnel that serve as team members providing leadership and support in the delivery of SBE.
Criteria Necessary to Meet This Standard
- Implement a strategic plan that coordinates and aligns the resources of the SBE program to achieve its goals.
- Provide personnel with appropriate expertise to support and sustain the SBE program.
- Use a system to manage space, equipment, and personnel resources.
- Maintain and manage the financial resources to support stability, sustainability, and growth of the SBE program’s goals and outcomes.
- Use a formal process for effective systems integration.
- Create policies and procedures to support and sustain the SBE program.
Professional Integrity
Professional integrity is demonstrated and upheld by all involved in simulation-based experiences. Professional integrity refers to the ethical behaviors and conduct that are expected of all involved throughout simulation-based experiences (SBE); facilitators, learners, and participants. Professional integrity is a person’s internal system of principles encompassing a number of additional interrelated values such as compassion, honesty, commitment, collaboration, mutual respect, and engagement in the learning process.
- Criteria Necessary to Meet This Standard
- Honor and uphold the Healthcare Simulationist Code of Ethics.
- Follow standards of practice, guidelines, principles, and ethics of one’s profession.
- Create and maintain a safe learning environment (Follow the HSSOBPTM Facilitation)
- Practice inclusion by respecting equity, diversity, and inclusivity among all involved and in all aspects of SBE.
- Require confidentiality of the performances and scenario content based on institution policy and procedures.
Simulation-Enhanced-IPE
Simulation-enhanced interprofessional education (Sim- IPE) enables learners from different healthcare professions to engage in a simulation-based experience to achieve linked or shared objectives and outcomes. The complex healthcare needs of today’s society require healthcare professionals to work as a collaborative team. Safe, quality health care depends on the ability of the health care team to cooperate, communicate, and share skills and knowledge appropriately. Sim-IPE is the overlap of the pedagogy of simulation and interprofessional education (IPE), providing a collaborative approach to the development and mastery of interprofessional practice competencies.
Criteria Necessary to Meet This Standard:
- Conduct Sim-IPE based on a theoretical or conceptual framework.
- Utilize best practices in the design and development of Sim-IPE.
- Recognize and address potential barriers to Sim-IPE.
- Devise an appropriate evaluation plan for Sim-IPE.
Participant Evaluation
Simulation-based experiences support the evaluation of knowledge, skills, attitudes, and behaviors demonstrated in the cognitive (knowledge), affective (attitude), and psychomotor (skills) domains of learning. Formative evaluation of the participants fosters personal and professional development, to assist the participant in the progression toward achieving objectives or outcomes.
The summative evaluation focuses on the measurement of outcomes or achievement of the objectives at a discrete moment in time, often at the end of a program of study. High-stakes evaluation refers to an assessment that has major implications or consequences based on the result or the outcome (such as on merit pay, progression or grades).
Authentic evaluation of the participants using simulation-based experiences includes the following elements: (a) determine the intent of the simulation-based experience, (b) design the simulation-based experience to include timing of the evaluation, the use of a valid and reliable assessment tool, and evaluator training required, and (c) complete the evaluation and interpret the results. Potential consequences of not following this standard may lead to inaccurate assessment, poor participant experiences, poor learning outcomes, failure to progress, inappropriate selection of tools, or assessment bias.
Criteria Necessary to Meet This Standard
- Determine the method of participant evaluation before the simulation-based experience.
- Simulation-based experiences may be selected for formative evaluation.
- Simulation-based experiences may be selected for summative evaluation.
- Simulation-based experiences may be selected for high-stakes evaluation.
HealthySimulation.com Standards of Best Practice Webinars
Introducing INACSL’s New Simulation Standard: Professional Development: In August of 2021 the new and updated Healthcare Simulation Standards of Best Practice (formerly known as the International Nursing Association of Clinical and Simulation Learning standards) were published. Included in this publication was a new standard: Professional Development. This webinar will describe the evidence behind the new standard, review the criteria and discuss how the simulationist can meet these described criteria. In addition, there will be a review of the changes made to the previously published standards and the additional new standards.
Introducing INACSL’s New Simulation Standard: Prebriefing: Prebriefing ensures that learners are prepared for the educational content of a simulation and are also informed about their expectations of them during the simulation-based experience. Because the current literature refers to prebriefing as both preparatory activities and briefing activities, this new standard incorporates both as pre-simulation activities. Historically, the terminology related to prebriefing has varied and included numerous terms. The lack of consistency in terminology can create confusion for educators and simulationists. Standardization of terminology and methodology can help to create more standardization in future use.
How to Implement INACSL’s Healthcare Simulation Standards of Best Practice Into Your Program: This CE presentation provides an overview of the ten Healthcare Simulation Standards of Best Practice(TM) and describes opportunities for application in the areas of writing outcomes and objectives, prebriefing, facilitation, debriefing, simulation design, operations, professional development, professional integrity, simulation-enhanced interprofessional education, and evaluation of learning and performance. We will highlight exemplars from academic and practice settings who have operationalized the Standards successfully and discuss a stepwise approach to using the Standards to improve simulation quality.
More About INACSL
The International Nursing Association for Clinical Simulation and Learning (INACSL) is the global leader in transforming practice to improve patient safety through excellence in healthcare simulation. INACSL is a community of practice for simulation where members can network with simulation leaders, educators, researchers, and industry partners. INACSL also provides the INACSL Standards of Best Practice: Simulation, an evidence-based framework to guide simulation design, implementation, debriefing, evaluation, and research. Learn more about the organization’s Standards of Best Practice on the INACSL website or by reading the articles below.

How to Develop a Healthcare Simulation Scenario Outside Your Clinical Expertise

Uses of Simulation Educator Needs Assessment Tool (SENAT)

6 Additional Medical Simulation Keywords You Need to Know About

Research Update: Clinical Simulation in Nursing | December 2022

INACSL Awards New Healthcare Simulation Standards Endorsement

Research: A Prebriefing Guide for Online, Virtual, or Distant Simulation Experiences

Should Clinical Learners Wear Uniforms During Healthcare Simulation Experiences?

Registration Open: INACSL Simulation Education Program

HealthySimulation.com Announces Partnership with New Affiliate, ASPE

INACSL Standards of Best Practice: Prebriefing | Preparation & Briefing

More than a Job: The Ongoing Professionalization of Healthcare Simulation
Sponsored Content: