An understanding of basic physiological concepts can enable Healthcare Technology Simulation Specialists (aka Sim Techs) without medical backgrounds a better understanding of the “why and the what” behind medical simulation. Extending beyond our recent articles entitled “Physiology: The Force Behind Simulation, A Guide for Techs Part 4: Diabetes” today we take a closer look at Hypoglycemia and blood sugars. We also share a free Excel template also furthering our previous articles on “Creating a Low Cost EMR” and “Tips and Tricks for Using Excel”. (Note: See the entire series linked at the bottom of this article).
Other Articles Similar to the Topic
About Diabetes
Diabetic patients are prone to fluctuating blood sugars which must be treated promptly in order to prevent serious consequences. Low blood sugar (hypoglycemia) is a constant concern because it can quickly lead to changes in the level of consciousness which in turn can impair a person’s ability to drive or safely operate machinery. Any patient with known diabetes or other condition that are likely to cause fluctuations in blood pressure will be monitored in the hospital on a routine basis. Routine monitoring often consists of AC/HS blood sugars (AC = before meals, HS bedtime). Some patients might need more frequent monitoring for example every 2 hours or an additional night time measurement at 2 or 3am. In addition, if healthcare practitioners suspect hypoglycemia, they will randomly check a finger stick blood sugar (FSBS).
Here you can download a FREE Template for a Hypoglycemia Protocol in
Excel Format for Your DIY Simulated EHR!
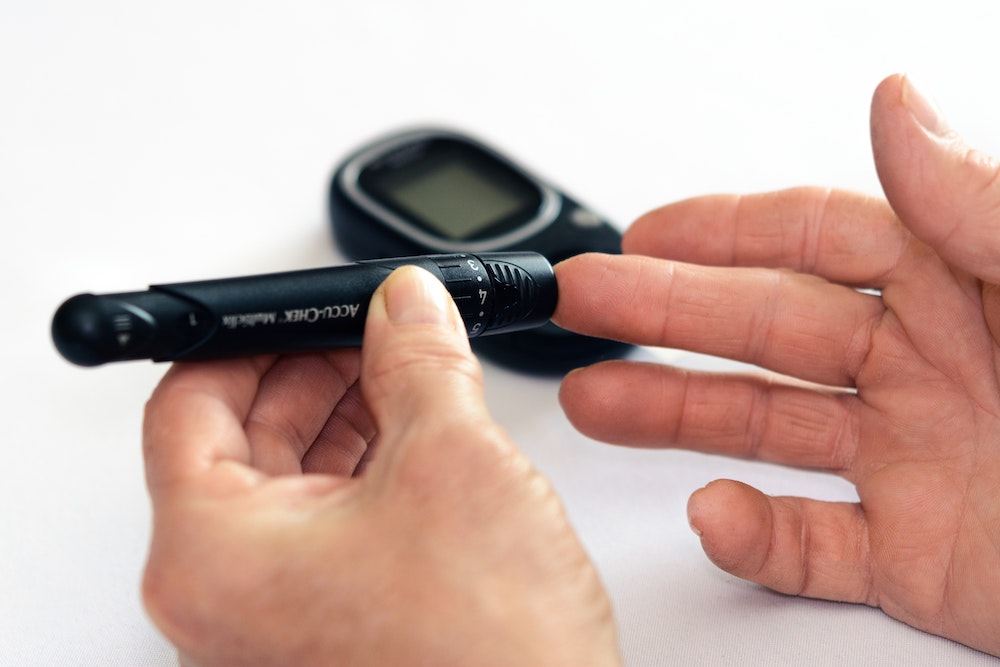
Technique for Finger Stick Blood Sugar
- Wash hands (Patients and Providers)
- Clean finger to be tested according to facility policy
- Explain the procedure to the patient
- Check the expiration date on the test strips
- Calibrate the monitor (if necessary) according to the manufacturer’s instructions
- Ensure the displayed calibration code matches the code on the calibration bar and the code on the test strip package insert
- Insert a test strip in the monitor according to the manufacturer’s instructions
- Lance the patient’s finger, obtain a sample of blood
- Apply the blood sample to the test strip when prompted by the monitor
- Dispose of the used lancets safety
- Record the result
- Document any intervention
- Note for simulation:
- Obtaining blood sugars takes time. Allow time for learner to complete the FSBS
- Do not have the monitor in the patient’s room. Learner must make a decision whether they should leave the patient or call for help
Causes of Hypoglycemia
- Not eating after insulin or oral medications to reduce blood sugar
- Too much insulin
- Some medications:
- Quinine, a drug used for malaria
- High doses of salicylates
- propranolol for hypertension
- Alcohol abuse
- Some liver diseases:
- Drug-induced hepatitis can cause hypoglycemia
- Kidney disorders
- Increased activity
- Endocrine problems
- Severe illness
Signs and Symptoms of Hypoglycemia
- Adrenergic – symptoms are related to release of stress hormones in response to low blood sugar:
- Shakiness
- Rapid/fast heartbeat
- Nervousness or anxiety
- Sweating, chills and clamminess
- Tingling or numbness in the lips or tongue
- Neuroglycopenia – low glucose supply to the brain
- Irritability or impatience
- Confusion, including delirium
- Lightheadedness or dizziness
- Hunger and nausea
- Sleepiness
- Blurred/impaired vision
- Headaches
- Weakness or fatigue
- Anger, stubbornness, or sadness
- Lack of coordination
- Nightmares or crying out during sleep
- Seizures
- Unconsciousness
- Note: Beta blockers may block the adrenergic responses making it difficult for patients to assess low blood sugar.
- Add a beta blocker to a sim scenario and limit symptoms to those related to neuroglycopenia.
Hypoglycemia Protocol
All diabetic patients in hospital should be covered by a hypoglycemic protocol (please see link for Excel Hypoglycemic template). The adult treatment depends on the patients level of consciousness and IV access.
- Awake, alert and able to swallow
- Unconscious or confused (unable to safely swallow or open mouth) with IV access
- Unconscious or confused (unable to swallow or open mouth), no IV access.
The attached hypoglycemia template may be adapted to match any facility. Running sim with a matching policy is desirable however, if students from different clinical sites will run through the same sim, let learners review the policy before the simulation.
The image shown in this article is of a Paramedics in Southern California attending a diabetic man who lost effective control of his vehicle due to low blood sugar (hypoglycemia) and drove it over the curb and into the water main and backflow valve in front of this industrial building. He was not injured, but required emergency intravenous glucose.
Read the Entire Physiology: The “Force” Behind Healthcare Simulation HealthySimulation.com Article Series:
- Part 1: Blood Pressure
- Part 2: Heart & Respiratory Rate
- Part 3: Pulse Oximetry
- Part 4: Diabetes
- Part 4B: Hypoglycemia & Excel Template for Simulated EHR
- Part 4C: Insulin
- Part 5: Sepsis
- Part 6A: Hypovolemia (Intro)
- Part 6B: Hypovolemia (Treatment & Simulation Tips)
- Part 7A: IV Fluids & Bags
- Part 7B: IV Pumps & Site Access
- Part 7C: PCA for Pain
- Part 8: ABGs
- Part 9: Sepsis Labs
Today’s article was guest authored by Kim Baily PhD, MSN, RN, CNE, previous Simulation Coordinator for Los Angeles Harbor College and Director of Nursing for El Camino College. Over the past 16 years Kim has developed and implemented several college simulation programs and previously chaired the Southern California Simulation Collaborative.
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!