Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 5: Sepsis
This article is the 5th in a series of posts related to physiology, the force behind simulation. Some simulation team members may have a limited background in physiology or medicine. An understanding of basic physiological concepts can enable non medical simulationists to better understand medical simulation. As timely diagnosis and intervention of sepsis are key factors in preventing mortality, simulation provides a unique opportunity to prepare clinicians and students in the identification and treatment of sepsis. This article, which includes basic information about the definition, cause, risk factors and pathophysiology of sepsis, is intended for simulation team members whose background is non medical or for those who need a refresher. (Note: See the entire series linked at the bottom of this article), but now Part 9 Covers Sepsis Labs in Medical Simulation.
A previous article “Understanding Lab and Vital Sign Indicators for Simulated Sepsis Scenarios” reviewed laboratory and other tests associated with the diagnosis of sepsis.
A Background on Sepsis
Sponsored Content:
- The exact definition of sepsis is still under debate!
- In 2001, the Sepsis-2 definition was developed:
- “an individual must have at least 2 SIRS criteria and a confirmed or suspected infection”.
- Systemic Inflammatory Response Syndrome (SIRS) criteria:
- Tachycardia (heart rate >90 beats/min)
- Tachypnea (respiratory rate >20 breaths/min)
- Fever or hypothermia (temperature >38 or <36 °C)
- Leukocytosis, leukopenia, or bandemia (white blood cells >1,200/mm3, <4,000/mm3 or bandemia ≥10%).
- For more than 2 decades the definition of sepsis and septic shock remained unchanged.
- This definition of sepsis and SIRS is still in use today.
- Recently in 2016, the Society of Critical Care Medicine (SCCM) and the European Society of Intensive Care Medicine (ESICM) recommended a new definition of sepsis – Sepsis-3.
- A “life-threatening organ dysfunction caused by a dysregulated host response to infection”.
- The new definition abandoned use of host inflammatory response syndrome criteria (SIRS) in identification of sepsis and eliminated the term severe sepsis.
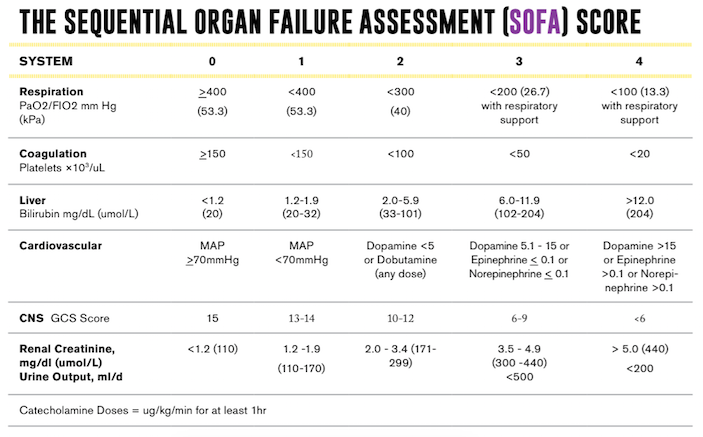
- The Sequential Organ Failure Assessment (SOFA) was recommended for diagnosis of sepsis (see link for details).
- Whatever the definition, sepsis is a life-threatening organ dysfunction which must be recognized and treated promptly in order to prevent septic shock (organ failure and death).
- Any type of infectious pathogen can lead to sepsis including viruses, protozoa and fungi.
- Antimicrobial resistance is a major factor leading to sepsis and overall risk of mortality in hospitalized patients.
- Some clinicians divide sepsis into three levels:
- Sepsis – two of the following symptoms plus a probably or confirmed infection.
- Body temperature above 101 F (38.3 C) or below 96.8 F (36 C)
- Heart rate higher than 90 beats a minute
- Respiratory rate higher than 20 breaths a minute
- Severe sepsis – one of the following signs and symptoms of organ failure
- Significantly decreased urine output
- Abrupt change in mental status
- Decrease in platelet count
- Difficulty breathing
- Abnormal heart pumping function (HR > 95, low BP)
- Abdominal pain
- Septic Shock – signs and symptoms of severe sepsis plus very low blood pressure which does not respond to intravenous fluids.
- Sepsis – two of the following symptoms plus a probably or confirmed infection.
Incidence of Sepsis
- According to the World Health Organization, the global epidemiological burden of sepsis, although difficult to estimate, is estimated to affect more than 30 million people worldwide every year.
- Higher rates occur in low and middle income countries.
- An estimated 3 million newborns and 1.2 million children suffer from sepsis every year.
- Sepsis is also the biggest killer of children under 5 worldwide.
- One in ten deaths associated with pregnancy and childbirth are due to maternal sepsis worldwide.
- In the US, the exact number of sepsis cases depends on the criteria used to measure sepsis however, in one study:
- “Clinical indicators of sepsis were present in 6%of hospitalized patients, of whom 21% died in the hospital or were discharged to hospice. Sepsis was present in 35% of all hospitalizations that culminated in death.” (2017. Rhee et al. Incidence and Trends of Sepsis in US Hospitals Using Clinical vs Claims Data, 2009-2014. JAMA Published online, Sept. 13, 2017)
- I.e. One in three hospital deaths is related to sepsis.
- The CDC estimates 2.7 million adults in the US develop sepsis each year and 270,000 die.
- Sepsis is the most expensive condition in U.S. hospitals costing over $15 billion per year.
- Some articles suggest the sepsis is increasing, while others refute this
- “Clinical indicators of sepsis were present in 6%of hospitalized patients, of whom 21% died in the hospital or were discharged to hospice. Sepsis was present in 35% of all hospitalizations that culminated in death.” (2017. Rhee et al. Incidence and Trends of Sepsis in US Hospitals Using Clinical vs Claims Data, 2009-2014. JAMA Published online, Sept. 13, 2017)
- General causes of increase in sepsis:
- Aging population.
- Drug-resistant bacteria – possibly a route cause of sepsis.
- Weakened immune systems – more patients living with HIV, cancer treatments or transplant medications.
- Other terms used for sepsis include blood poisoning, toxic shock syndrome, endotoxemia, or blood stream infection.
Risk Factors of Sepsis
- Very young, very old.
- Male
- US black race
- Certain genetic variants
- Respiratory tract infections
- Gram-positive infections are more frequent that Gram-negative sepsis
- Compromised immune system
- Very sick, intensive care patients.
- Wounds or injuries, such as burns
- Invasive devices, such as intravenous catheters, breathing tubes, dialysis catheters.
- Pregnancy
- Liver cirrhosis
- Kidney disease
- Autoimmune diseases and no spleen
Pathophysiology of Sepsis
Sponsored Content:
- Sepsis occurs when chemical mediators released into the bloodstream to fight off an infection (noxious stimuli) trigger bodywide inflammatory responses. These responses in turn, trigger a cascade of changes that can damage multiple organ systems, causing them to fail.
- The body responds to bacterial invasion by a complex process that involves:
- Localization and control of the invasion
- Repair of injured tissue.
- Circulating and fixed phagocytic cells activation.
- Proinflammatory and anti-inflammatory mediator release.
- Sepsis may result from viral, protozoan and fungal infections as well as bacteria.
- SIRS consists of changes in clinical signs including an abnormal body temperature, increased heart rate, increased respiratory rate, an abnormal white cell count (either decreased or elevated), or an increase in band neutrophils.
- Neutrophils mediate cellular change leading to vasodilation and inflammation.
- The inflammatory reaction is mediated by the release of cytokines, including tumor necrosis factor-alpha, interleukins, and prostaglandins, from neutrophils and macrophages.
- Cytokines are released which activate the extrinsic coagulation cascade and inhibit fibrinolysis.
- Fluid can leak from the circulation into the interstitial space:
- Intravascular volume decreases and hypotension occurs.
- Inadequate tissue perfusion leads to cellular hypoxia and lactic acidosis.
- Tachypnea occurs in response to lactic acidosis.
- Nitrous oxide is produced in the endothelium – this adds to hypotension.
- Fluid can leak from the circulation into the interstitial space:
- These overlapping processes result in microvascular thrombosis; thrombosis is one potential factor producing organ dysfunction.
- Activation of the coagulation system leads to consumption of endogenous anticoagulants (e.g., protein C and antithrombin); this may be an important factor in the development of microvascular coagulation.
- May lead to Disseminated Intravascular Coagulation (DIC).
- Anti-inflammatory mediators as well as inflammatory mediators have a role in sepsis, and an excess of either can result in poor patient outcomes.
- Inflammation affecting neurons, glial cells, and endothelial cells can lead to leakage of the blood brain barrier and depressed neurological function.
- Reduction in cardiac output leads to stimulation of the compensatory mechanisms which include:
- Stimulation of baroreceptors in the carotid sinus and aortic arch which leads to stimulate of the sympathetic nervous response.
- Adrenaline release from the adrenal glands
- Vasoconstriction
- Increased heart rate and contractility.
- The renin-angiotensin-aldosterone system helps to maintain blood pressure (retention of sodium and water by the kidneys and vasoconstriction).
- Patients die from multi organ failure, hypotension and mesenteric ischemia (loss of blood flow to the gut).
Prevention of Sepsis
-
- Prevention of microbial transmission and infection
- Handwashing and other effective hygiene practices
- Vaccines
- Prevention of the evolution of an infection to sepsis conditions.
- Early detection and treatment.
- Appropriate use of antibiotics
- Fluid resuscitation.
- Early detection and treatment.
- Prevention of microbial transmission and infection
Understanding the pathophysiology behind medical disorders enables non medical simulation team members to more fully understand scenario goals. Look for new Healthysim articles on the treatment of sepsis and sepsis scenario development in the coming months.
Read the Entire Physiology: The “Force” Behind Healthcare Simulation HealthySimulation.com Article Series:
- Part 1: Blood Pressure
- Part 2: Heart & Respiratory Rate
- Part 3: Pulse Oximetry
- Part 4: Diabetes
- Part 4B: Hypoglycemia & Excel Template for Simulated EHR
- Part 4C: Insulin
- Part 5: Sepsis
- Part 6A: Hypovolemia (Intro)
- Part 6B: Hypovolemia (Treatment & Simulation Tips)
- Part 7A: IV Fluids & Bags
- Part 7B: IV Pumps & Site Access
- Part 7C: PCA for Pain
- Part 8: ABGs
- Part 9: Sepsis Labs
Today’s article was guest authored by Kim Baily PhD, MSN, RN, CNE, previous Simulation Coordinator for Los Angeles Harbor College and Director of Nursing for El Camino College. Over the past 16 years Kim has developed and implemented several college simulation programs and previously chaired the Southern California Simulation Collaborative.
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Learn more about Sepsis – Understanding the Physiology Behind Simulation.!
Dr. Kim Baily, MSN, PhD, RN, CNE has had a passion for healthcare simulation since she pulled her first sim man out of the closet and into the light in 2002. She has been a full-time educator and director of nursing and was responsible for building and implementing two nursing simulation programs at El Camino College and Pasadena City College in Southern California. Dr. Baily is a member of both INACSL and SSH. She serves as a consultant for emerging clinical simulation programs and has previously chaired Southern California Simulation Collaborative, which supports healthcare professionals working in healthcare simulation in both hospitals and academic institutions throughout Southern California. Dr. Baily has taught a variety of nursing and medical simulation-related courses in a variety of forums, such as on-site simulation in healthcare debriefing workshops and online courses. Since retiring from full time teaching, she has written over 100 healthcare simulation educational articles for HealthySimulation.com while traveling around the country via her RV out of California.
Sponsored Content: