Physiology: The Force Behind Healthcare Simulation – A Guide for Techs, Part 4: Diabetes
This article is part 4 of a series of posts related to physiology, with this article introducing the physiology of diabetes. Some simulation team members may have a limited background in physiology or medicine. An understanding of basic physiological concepts can enable non medical simulationists to better understand medical simulation. (Note: See the entire series linked at the bottom of this article).
Diabetic patients are prone to fluctuating blood sugars which must be treated promptly to prevent serious consequences. Later articles will discuss treatment of high blood glucose (hyperglycemia) and low blood sugar (hypoglycemia). Both situations make ideal simulation scenarios.
An estimated 30.3 million people of all ages—or 9.4% of the U.S. population—had diabetes in 2015. This total included 30.2 million adults aged 18 years or older (12.2% of all U.S. adults), of which 7.2 million (23.8%) were not aware of or did not report having diabetes. At least one in four hospitalized patients has diabetes. Medical simulation provides an opportunity for learners to care for patients with diabetes either as the primary admitting diagnosis or as a comorbidity.
Sponsored Content:
Diabetes is a progressive disease that interrupts fuel metabolism within the body. Diabetes is not just a disease of carbohydrate (CHO) metabolism but also of protein and fat metabolism.
Pancreas
- Elongated organ located behind stomach
- Exocrine function: Secretes digestive enzymes into the gut to breakdown food.
- Endocrine function: Secretes hormones (chemical messengers) that respond to changes in blood sugar.
- Glucagon – secreted in response to low blood sugar, low protein intake, exercise, starvation and low CHO diet.
- Somatostatin – inhibits release of glucagons and insulin
- Insulin – secreted by beta cells in response to increasing blood sugar
- Other hormones increasing blood sugar:
- Adrenalin (epinephrine)
- Growth hormone
- Glucocorticoids
- Insulin
- Insulin is the “key” that opens a lock in cell walls allowing glucose to enter a cell and be used for energy
- Principal regulator of metabolism of CHO, fats, and proteins
- Promotes excess storage of glucose in the liver in the form of glycogen.
- Promotes protein synthesis within cells
- Stimulates other critical metabolic pathway
- Note: the brain and livers do not need insulin for glucose uptake.
- Insulin production
- Remember the body tries to maintain body functions within a certain range – homeostasis.
- The hormones above are released so that blood sugar cycles between:
- 70-100 mg/dL
- Insulin is secreted in a continuous (pulsatile increments) basal rate with bolus when food ingested
- Insulin is measured in units – typically 40 to 50 units are secreted daily.
Diabetes Mellitus (GK: Passing through – dilute urine, mellitus honey)
- Diabetes is not one disease but a group of genetically and clinically heterogeneous disorders characterized by abnormalities in glucose homeostasis
- Untreated diabetes leads to vascular lesions and neuropathy which in turn may lead to:
- Stroke, cardiovascular disease, blindness, kidney failure, peripheral vascular disease, amputation
- Diabetes is the sixth leading cause of death in the US.
- Women more likely to die from diabetes
- Women with diabetes 4 times the risk of CV disease
- Etiology
- Current theories include genetic, autoimmune, viral, environmental factors (e.g. obesity, stress)
- Classification of diabetes – although there are several types of diabetes the most common are:
- Type 1 diabetes
- Absolute – pancreas produces no insulin or very little insulin.
- Progressive destruction of pancreatic beta cell function as a result of autoimmune process
- Hyperglycemia (high blood glucose) is not observed until 80-90% destroyed
- Requires exogenous insulin – from outside the body.
- Usually more rapid onset than type 2
- Lose weight rapidly since glucose cannot be used for metabolism, instead fats and muscle tissues are catabolized.
- Type 2 diabetes – 90% of diabetic patients.
- Relative – pancreas produces normal or excessive amounts of insulin but body is unable to use it effectively aka insulin resistance.
- Increases with age – half cases >55 but not called late onset.
- In the US increasing obesity in young people has led to a significant rise in Type 2 diabetes in this age group.
- No major weight loss because enough insulin is produced to prevent the breakdown of fat and muscle tissue.
- Type 2 pts are mostly obese.
- Prevalence depends on race – highest in Hispanics and African Americans
- Gestational diabetes – elevated blood sugars during pregnancy
- Type 1 diabetes
The Three Cardinal Signs of Diabetes
Sponsored Content:
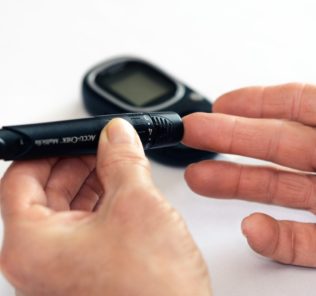
- When blood sugars start to rise to the renal threshold of 180 mg/dL, glucose spills over into urine.
- Excessive glucose attracts water – osmotic diuresis occurs resulting in polyuria
- Polyuria causes electrolyte loss (NA+, K+, Cl+, Phosphorus)
- This can lead to a serious imbalance of electrolytes
- Loss of water stimulates thirst center causing polydipsia (increased thirst)
- Cells are starved of fuel so pt. is excessively hungry and eats a lot more – polyphagia .
- The three cardinal signs are most often associated with Type 1 diabetes. In a simulation scenario a parent should report that their child has been noticeably thirsty, hungry and needs to urinate frequently.
- Excessive glucose attracts water – osmotic diuresis occurs resulting in polyuria
Diagnosis of Diabetes
- Fasting blood glucose levels (no food for 12 hours):
- Normal fasting blood glucose: 70-100 mg/dL
- Prediabetes (Impaired fasting blood glucose): >100 but <126 mg/dL
- Diabetes: >126 mg/dL
- Two-hour postprandial plasma glucose level (GTT)
- Normal: blood glucose drops to below 140 mg/dL
- Prediabetes (Impaired glucose tolerance) >140 but < 200 mg/dL
- Diabetes: >200 mg/dL
- Glycated Hemoglobin (HbA1c)
- Glucose attaches to red blood cells which have a lifespan of approximately 90 days.
- Provides an average blood glucose level over the past 3 months
- Normal <5.7%
- Prediabetes 5.7% to 6.4%
- Diabetes >6.5%
Diabetes can be incorporated into any existing scenario thereby increasing the complexity of the scenario. Alternatively a significant change in blood glucose levels can form the basis of a standalone scenario. Examples of learning outcomes related to care of the diabetic patient.
- Healthcare professional responding to grieving associated with the diagnosis of a new progressive disease.
- Patient education
- Prevention of serious complications associated with diabetes.
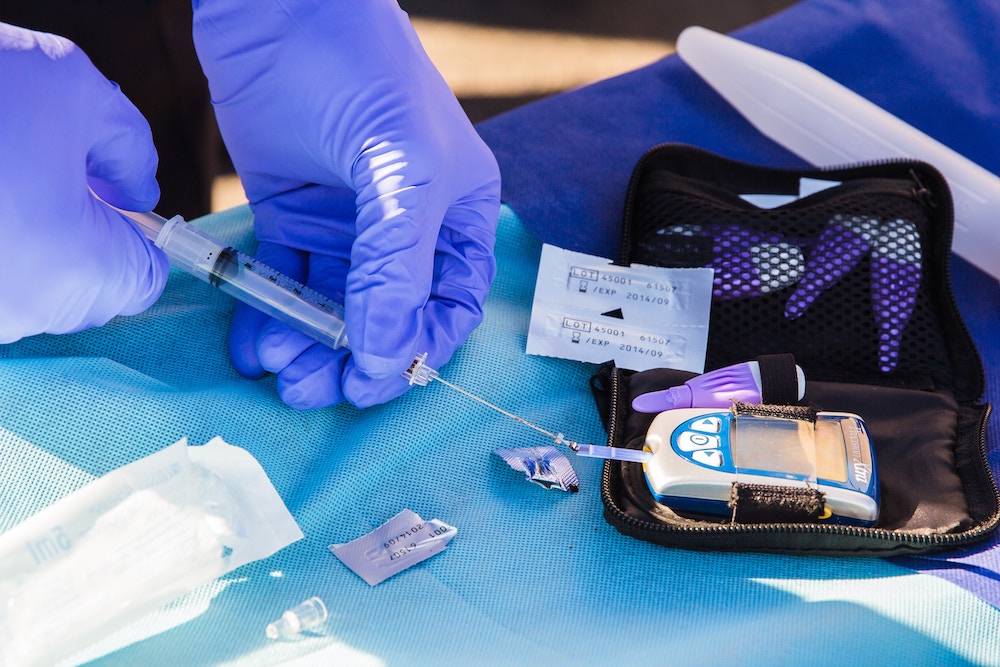
- Drawing up and injecting insulin
- Dietary requirements
- Lifestyle changes to reverse prediabetes
- Prevention of stroke
- Patient and child education for diagnosis.
- Routine hospital premeal and bedtime insulin regimens (ACHS)
- Sliding scale insulin administration
- Types of insulins
- Continuous insulin infusions.
- Assessing insulin and CHO requirements.
- Rapid response/treatment for hyperglycemia and hypoglycemia.
- Diabetic ketoacidosis (DKA)
- Hyperosmolar hyperglycemic state (HHS)
- Hypoglycemia
- When to call RRT
This article has introduced the basics of diabetes. In the coming months other articles will be published that will review the physiology behind specific treatment modalities for diabetic patients.
Read the Entire Physiology: The “Force” Behind Healthcare Simulation HealthySimulation.com Article Series:
- Part 1: Blood Pressure
- Part 2: Heart & Respiratory Rate
- Part 3: Pulse Oximetry
- Part 4: Diabetes
- Part 4B: Hypoglycemia & Excel Template for Simulated EHR
- Part 4C: Insulin
- Part 5: Sepsis
- Part 6A: Hypovolemia (Intro)
- Part 6B: Hypovolemia (Treatment & Simulation Tips)
- Part 7A: IV Fluids & Bags
- Part 7B: IV Pumps & Site Access
- Part 7C: PCA for Pain
- Part 8: ABGs
- Part 9: Sepsis Labs
Today’s article was guest authored by Kim Baily PhD, MSN, RN, CNE, Simulation Coordinator for Los Angeles Harbor College. Over the past 15 years Kim has developed and implemented several college simulation programs and currently chairs the Southern California Simulation Collaborative.
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Learn more about Diabetes here!
Dr. Kim Baily, MSN, PhD, RN, CNE has had a passion for healthcare simulation since she pulled her first sim man out of the closet and into the light in 2002. She has been a full-time educator and director of nursing and was responsible for building and implementing two nursing simulation programs at El Camino College and Pasadena City College in Southern California. Dr. Baily is a member of both INACSL and SSH. She serves as a consultant for emerging clinical simulation programs and has previously chaired Southern California Simulation Collaborative, which supports healthcare professionals working in healthcare simulation in both hospitals and academic institutions throughout Southern California. Dr. Baily has taught a variety of nursing and medical simulation-related courses in a variety of forums, such as on-site simulation in healthcare debriefing workshops and online courses. Since retiring from full time teaching, she has written over 100 healthcare simulation educational articles for HealthySimulation.com while traveling around the country via her RV out of California.
Sponsored Content: