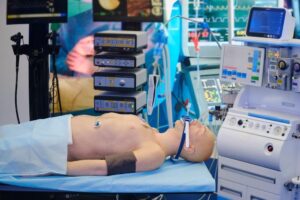
Patient Safety Movement Foundation: The Importance of High Reliability and Safer Care Through Simulation
To help offset unreliability and medical error, the Patient Safety Movement Foundation (PSMF) provides free resources to healthcare simulation organizations across the continuum of care become more highly reliable across the globe. PSMF works with hospital systems, critical access hospitals, ambulatory care centers, outpatient clinics, primary care offices, long-term care facilities, and many others to implement best practices in patient safety and sustain continuous improvement skills. through clinical simulation. The organization’s Actionable Patient Safety Solutions (APSS) are freely available on the organization’s website and include evidence-based summaries of best practices, performance improvement plans, clinical workflows, videos, articles, and more.
PSMF believes that high reliability should no longer be optional in healthcare, and that going on a journey to become an HRO will eventually have to happen in every system, whether by proactive choice or in response to new regulatory requirements. The COVID-19 pandemic has shown healthcare providers that safety “foundations” in healthcare are precarious and that the field of healthcare must do a better job to keep everyone safe, including healthcare workers, patients and families.
Educators can effectively help organizations become highly reliable through the use of healthcare simulation. High reliability organizations (HRO) are those able to go for long periods of time without any errors, such as the aviation and nuclear power industries. Notably, after 346 people died in two air crashes in 2019, the Boeing 737 MAX was grounded for nearly two years while engineers studied what went wrong and validated the safety of the aircraft.
Sponsored Content:
Although we have been talking about the importance of creating highly reliable systems and safer healthcare processes for the past 20 years, preventable medical errors continue to take the lives of more than 200,000 people annually. The public would never stand for such statistics from the airline industry, and yet being an HRO remains optional for many healthcare systems.
A handful of organizations have adopted key features of an HRO, such as Lean improvement and Six Sigma, and these initiatives have proven fruitful. However, most organizations have not yet made the commitment to high reliability, often due to cost constraints, competing for organizational priorities, and a discrepancy between realistic frontline experience and perceived experience by leadership. Additionally, the distress and exposure of the COVID-19 pandemic will continue to shake healthcare systems into reactivity and subsequent poor care if they do not begin to develop safer, more reliable healthcare care systems and processes across the continuum.
Creating and sustaining an organizational safety culture that anticipates medical errors and learns from mistakes will become a requirement for all healthcare organizations in the near future. Healthcare educators and administrators can play a critical role in helping organizations become HROs through clinical simulation. This type of training is an excellent method for the system-wide, aligned education that needs to occur for such a transformation to suceed.
PSMF believes three critical components are required for an organization to become highly reliable. These include a person-centered culture of safety; a holistic, continuous improvement framework; and an effective model for sustainment. The switch to a safety mindset must be driven by the board of directors and the CEO, who should prioritize the safety of all individuals, including patients, staff, consultants and vendors.
Sponsored Content:
This means that “the right hand knows what the left hand is improving, and there is alignment between all of the improvement work happening across the organization.” This helps facilitate a mechanism to track when errors occur or nearly occur, and when a process needs to be revisited. Equally critical, aligning improvement means having a standard way to communicate, educate, and promote accountability. Healthcare simulation can be used to hardwire each of these three components. Even if an organization has not yet embarked on its HRO journey, it can still incorporate these concepts into its current curriculum and effectively improve patient outcomes as a result.
PSMF encourages every organization to begin its journey now with a current state assessment of all education and simulation activities in the organization. Healthcare organizations should consider redundancy, gaps and the sheer number of educational activities the frontline staff have to complete and subsequently assess their effectiveness and translation into practice for improvement. Further, they should assess the variation in educational activities, including online modules, classes, skills fairs, and simulations, to understand those most efficacious and seek to evaluate how meaningful these activities are for frontline clinicians. If frontline clinicians are completing these activities because they are required, and are not extracting meaningful information for behavior change, they should consider reassessing how this information is delivered.
Healthcares provider should approach this assessment as they would any performance improvement project. They must design a current state map of the education curriculum that includes all activities staff and leaders must complete and that names the author the content. Then, they should include orientation and onboarding, annual competency validation, continuing education, and required certifications. They should look for conflicting or duplicate content, content that is not tailored to the team member’s role and learning needs or lack of alignment of education with quality initiatives. By thinking about this from a “consumer” perspective, simulation educators can understand inefficiencies and how often learning outcomes are truly met through behavior change.
After a thorough current state assessment, educators can begin to brainstorm the suggestions in this article series, which can help hardwire the three critical components of safe and reliable care. Simulation is an optimal way to hardwire these concepts, and the alignment of organizational improvement initiatives and tactical educational activities is critical in organizations on a journey to high reliability.
More About the Patient Safety Movement Foundation
Headquartered in Irvine, California, the goal of PSMF is to reduce the number of preventable deaths due to medical error to zero by creating a sense of urgency and unifying humanity. PSMF is working toward preventing these deaths by presenting specific, high-impact solutions to meet patient safety challenges, or Actionable Patient Safety Solutions, to encourage medical technology companies to share the data for which their products are purchased and by asking hospitals to make commitments to implement Actionable Patient Safety Solutions.
PSMF works with all stakeholders to address problems with actionable solutions for patient safety and convenes at the World Patient Safety, Science & Technology Summit. The Summit brings together some of the world’s best minds for thought-provoking discussions and new ideas to challenge the status quo. PSMF notes that improving patient safety requires a collaborative effort of all stakeholders, including patients, healthcare providers, medical technology companies, government, employers and private payers.
Learn More About Patient Safety Movement Clinical Support Products and Services!
Today’s article was guest authored by Donna M. Prosser, DNP, RN, NE-BC, FACHE, BCPA, Chief Clinical Officer at Patient Safety Movement Foundation. This article is the first in a series of four from the Patient Safety Movement with tips on how to effectively use clinical simulation to hardwire a foundation for patient safety and reliable care to make safety the number one priority of all providers. The next article, to be published in March 2021, will focus on how to use simulation to hardwire a person-centered culture of safety.
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Dr. Donna Prosser has been in the healthcare industry for more than 30 years and is currently the Chief Clinical Officer at the Patient Safety Movement Foundation. She spent the first fifteen years of her career at the bedside and transitioned into administration after a personal experience helped her to understand just how fragmented and unsafe patient care can be. This experience ignited a passion to improve healthcare quality and safety in her that continues to burn to this day.
Prior to joining the Patient Safety Movement Foundation, Dr. Prosser worked as a healthcare consultant, helping organizations across the United States to improve quality and safety, increase patient engagement, and reduce clinician burnout. Before beginning her consulting career, she served as a Chief Nursing Officer and was responsible for clinical practice improvement across two healthcare systems.
Sponsored Content: