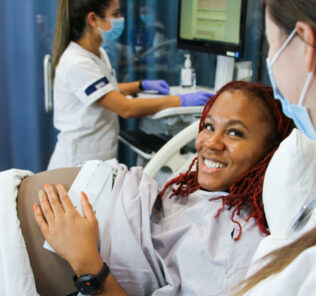
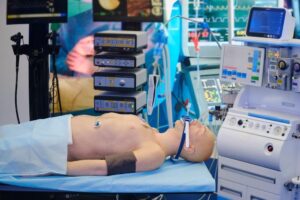
A Systems View on Clinical Simulation Suites: An Outsider’s Perspective
*Special Update: Join Terry Tomorrow for his Webinar “Simulation Programs and Online Learning: 3 Converging Trends“. The Marquess of Salisbury, three-time UK Prime Minister (1885-1902), said: “No lesson seems to be so deeply inculcated by the experience of life as that you never should trust experts. If you believe the doctors, nothing is wholesome. If you believe the theologians, nothing is innocent. If you believe the soldiers, nothing is safe.” (Dale, 2020).
Experts today are under pressure due to the coronavirus, but the late prime minster’s observation has wider relevance to clinical training, which is pulled by advancing technology and pushed by social distancing. Will progress require specialists or generalists to realize the potential available? This essay, by Terry Young, FBCS, Professor Emeritus at Brunel University London and Principal of Datchet Consulting Ltd., explores clinical simulation suites from three angles: computer modeling, business processes, and higher education. Professor Young spent 16 1/2 years in the healthcare simulation industry designing devices and systems, and 17 years as a professor leading large multi-disciplinary research teams in healthcare. He has also developed key pedagogical innovations and generated new ideas for wider benefit.
Young started in research and development with Finite Elements (Young, 1988), winning the 1989 IEE Premium Award, and learned to put a value on every invention we considered. Later, his research as a university professor demonstrated that healthcare needed to make better use of industrial methods (Young, et al., 2004). This also introduced him to health economics. In his 40s, and facing hundreds of students, he learned about pedagogy from scratch. So, what has his journey taught him, and how does that relate to simulation suites? Young writes…
Sponsored Content:
1. Health and education don’t fully grasp the importance of prototypes and simulation.
Although the health and education fields understand complexity and abstraction, both have developed incrementally through person-to-person communication. As I see it, neither grasps the extent of the system outside the lecture or operating room, nor appreciates how profoundly that world governs what happens inside either theatre.
The idea that a cut-down representation of reality – a mock-up, a dummy, a computer program or a prototype – could improve the delicately physical delivery of health or education has perplexed traditional thinkers, at least until the great lockdowns of 2020.
However, models and synthetic representations (as well as augmented reality) are powerful ways to prototype systems and services, as well as to train practitioners (Young, 2018). Industry understands systems and uses tools that health and education find exotic. I think that tide is turning.
Sponsored Content:
2. Teaching and learning could be much improved.
Over two decades, I have worked with smart educators and discovered that normal practice is well behind what the best deliver. However, great lecturers are unable to leverage their competencies across their communities.
When I first looked at blended learning, I was asked what theory I would use. When I visited U.S. colleges, I discovered that MOOCs (massive open on-line courses) were still in their infancy. When I implemented a basic mix of online and in-person delivery, the students showed me that I was suddenly an accidental expert. It’s a funny world where you know nothing and yet know so much at the same time.
Then there was assessment! I discovered threshold, or criterion-based, grading, and realized it applied far beyond grading students: to balanced scorecards, for instance, refereeing projects, even career development. To share these insights, starting this autumn we are promoting a three-part model.
This consists of hard learning that students do by themselves or in groups; challenging discussion in facilitated groups; and stretching assessments that provide learning opportunities and also demonstrate key competencies for grading. The series also explores how to make face-to-face encounters work online, and how to explore the web for content for your students. For me, it saved grading time, too!
3. Tracking cost and benefits is hard, necessary, and possible
Alongside learning and assessment, I discovered health economics through my research, where intangible benefits such as better health could be included in business planning (Girling, et al., 2015). In the UK, the QALY (quality adjusted life year) is the quantum of health – and the increments by which your health improves or worsens can be measured and valued when planning new services.
I have argued in the Times Higher (what higher education can learn from healthcare reforms) that we need similar ways to capture educational benefits, especially when people start from such different places and follow such different paths. Even without that, a simple business model shows that group teaching is affordable under lockdown (An industry-style focus on teaching costs is vital to survive the pandemic).
Finally, what is the return-on-investment of using models to prototype systems? A staging post in a trilogy of papers (the last is under review) reports a cost-effectiveness analysis of using a discrete event simulation to design a stroke service (Soorapanth & Young, 2019). It was shortlisted for the Operational Research Society’s Goodeve Medal this year. Sadly, it didn’t win. Still, the puzzle pieces are coming together.
I’ve enjoyed my journey and see exciting times ahead for simulation suites in education and designing better services. By linking their technology with educational advances in higher education, simulation suite managers can offer mixed-mode education that accredits key skills.
Through connecting to economic and business methods, they can measure and demonstrate the value they add to the career of every student who passes through. Additionally, by creatively restructuring the syllabus, they can offer students a more curiosity-driven learning experience and avoid burning themselves out.
About Datchet Consulting
Academia, healthcare and industry face separate but similar problems. They need to nurture talent and cultivate the next generation of innovators, products, systems and services. Datchet Consulting’s experience of cross-sector working has shown these borderlands to be a rich environment for innovation. It is committed to fostering the flow of ideas across cultural divides, supporting better education and training and faster development of higher quality systems and services.
Datchet Consulting specialises in helping academics develop strategy for reaching out, and those in healthcare and industry to reach across to academics. The reality is that life is usually complicated and successful collaboration relies on relationships that work at more than one level, which deliver short-term and long term gains in each direction.
Learn More on the Datchet Consulting Website!
References:
- Dale, I., 2020. The Prime Ministers: 55 Leaders, 55 Authors, 300 Years of History. Kindle Edition ed. London: Hodder & Stoughton.
- Girling, A., Lilford, R., Cole, A. & Young, T., 2015. Headroom approach to device development: current and future directions. International journal of technology assessment in health care, 31(5), pp. 331-338.
- Soorapanth, S. & Young, T., 2019. Assessing the value of modelling and simulation in health care: An example based on increasing access to stroke treatment. Journal of the Operational Research Society, 70(2), pp. 226-236.
- Young, T., 2018. What is a Simulation Suite For: Training, Troubleshooting, or is it a Design Tool?. MT Magazine, Issue 2.
- Young, T. et al., 2004. Using industrial processes to improve patient care. BMJ, Volume 328, pp. 162-164.
- Young, T. P., 1988. Design of integrated optical circuits using finite elements. IEE Proceedings A, 135(3), pp. 135-144.
I am a well-organised thinker, shaper, and an extraordinary networker who can attract bright people from diverse backgrounds, encourage them to orientate their thinking around a common challenge, and then co-create new ideas and knowledge with them and their served communities. For 16 years I designed devices and systems at GEC and Marconi and for the past 16 years as a professor at Brunel, I have built and led large multi-disciplinary research teams in healthcare, while developing key pedagogical innovations. Analytical and creative, I can co-create strategy and nurture it into practice. In the ‘80s, this meant building an internationally recognised photonic design platform, in the ‘10s it has been The Cumberland Initiative as a multi-partner network to re-design health systems and services.
Sponsored Content: