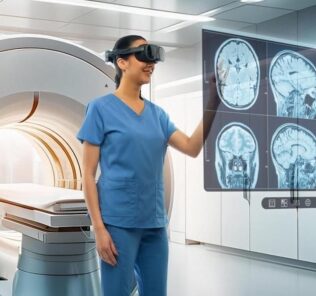
Augmented Reality vs Virtual Reality in Healthcare Simulation
Have you ever wondered about the differences between Augmented Reality vs Virtual Reality? There is no doubt that the very nature of medicine has been forever changed by the COVID-19 pandemic and the healthcare industry’s response. The trickle-down effect has also impacted healthcare simulation and the way clinical simulation participants must now approach interactive learning. In this new approach, quite a few new modalities have risen to the top as the most innovative and eye-catching which all fit under the category of “XR” or Mixed Reality training. Virtual Reality (VR) and Augmented reality (AR) companies have developed at an increasing rate to help deliver quality healthcare simulation training while maintaining attention to safety in regard to COVID-19 protocols. This HealthySimulation.com article details some of the new simulation technologies available and helps identify which may be more ideal for certain facilities, institutions, learners, and educators. First, some clarifications on terminology:
Virtual Reality (VR) in medical simulation utilizes a computer-generated 3D image or environment that can be viewed and interacted with through the use of special electronic equipment. An example of this type of equipment is a head-worn apparatus and the use of specially calibrated selector wands. The apparatus and wands then offer a fully immersive experience when the participant interacts with are computer generated.
Augmented Reality (AR) in medical simulation utilizes the addition of a computer-generated image or environment to real-world space. Much like in virtual reality, the image or environment in AR can be viewed and interacted with through the use of special electronic equipment. An example of this equipment would include just the head-worn apparatus. The selector wands would be eliminated through the use of specialized mapping software which allows the use of the participants’ own hands.
Sponsored Content:
A Breakdown of Virtual Reality (VR)
While the advancement of technology is always exciting across healthcare simulation, taking a step back and looking at the technology with logic and sound reasoning is beneficial. Creating a pros and cons list is the quickest and easiest way to achieve this goal. Starting with virtual reality, the pros list could include full immersion in changing environments, low cost, and a large marketplace of creative companies. Imagine being in the back of an ambulance doing CPR training one moment, and then being instantly transported to a surgical training on the International Space Station the next!
VR gives an immersive and highly interactive experience that is usually well received and encourages a high level of engagement from the learner. Full immersion allows the learner to be transported to a completely different environment without leaving the room. The room alone will open the doors to a number of training possibilities. Many companies are wading into the virtual realm which helps with the cost of VR equipment and software. Examples of companies that develop VR tools in medical simulation include SimX, VRpatients, PCS, UbiSim, and FundamentalVR among others.
In terms of negatives associated with VR, the resource comes with the potential for injury, software limits, and reliance on paired technology. When a participant is in full immersion, the level of potential injury is ever-present. Wearing a headset that fully covers the eyes and potentially the ears, the participant cannot see the actual environment around them, potentially harming themselves if left to act out the virtual actions in the real environment.
Sponsored Content:
As the market for these types of VR software becomes larger with time, the limits of VR programming can leave learners with the inability to suspend disbelief. Aiding in their disbelief, the use of selector wands can be both a pro and a con. The wands are well calibrated with the VR experience making them easy to use. Still, on the negative side, the wands are just wands and not a user’s own hands.
A Breakdown of Augmented Reality (AR)
Taking a look at augmented reality, inherent benefits include spatial awareness, real-world incorporation, and software integration. An AR platform will incorporate the environment that surrounds the learner into the visualization created by the headset. More importantly, the environment and the elements that make up a room can be seen, providing for increased safety with AR. Companies that manufacture AR in clinical simulation include CAE Healthcare, GigXR and MedCognition.
This technology incorporates the user into the interface, such as the use of the learner’s own hands as selectors which leads to a more realistic and interactive experience. Software integration is a large part of AR programming, and although the integration is not across the board, most AR platforms are based on software that easily integrates with the typical Windows and Mac OS.
The negatives of AR simulation are cost, lack of programs, and hardware requirements. If a healthcare simulation program were to compare an AR platform to a VR platform, solely on cost, the AR platform would look overpriced. The average AR headset ranges from $1k to $3k, making these headsets a difficult item to justify within a budget. If a clinical simulation program were to compare the two platforms on the availability of healthcare-related programs, AR would lose out again.
Additionally, augmented reality simulation is the younger of the two technologies, which means that there are a lot more VR than AR programmers. The hardware also requirements for an AR platform are much higher than for a VR platform. Usually requiring a processor and visual system upgrade to any off-the-shelf computer.
In addition to these pros and cons, a medical simulation program must ask pertinent questions when considering any VR or AR purchase. For example, “Does a VR or AR platform enhance the simulation program?” While both new technologies are exciting and alluring, one platform may be more beneficial than the other. The harder truth may be that the addition of a VR and/or AR component would not enrich or add value to a healthcare simulation program in a practical sense. On a tight budget, the technologies would not be practical to invest in a training tool that has no enrichment value and sits on a shelf collecting dust till it is obsolete.
From a business sense, a healthcare simulation program must ask if the addition of one or both technologies will yield a return on the investment. This return does not have to be monetary. A return on investment can be calculated in usage and appeal. If the technology gains a heavy track record of usage, then the solution(s) was a good investment, even with no compensation.
The appeal of healthcare simulation technology can be beneficial by drawing in interested parties which could lead to their discovering more of what a clinical simulation program has to offer. The opposite can be the reality of both usage and appeal, so an objective and logical evaluation prior to purchase is required.
AR vs VR: Additional Implementation Advice
When considering a new technology like AR or VR, the speed at which those technologies grow needs to be evaluated and thoroughly considered. New technologies can grow in a number of ways, but two growth pathways are important for a healthcare simulation program.
First, the growth may be the number of companies that either adopt the technology or companies that started from the technology. This particular type of growth should be watched closely for the emergence of a superior product. Simulation technology does not have a track record of fast-paced turn over so waiting to see if a superior product emerges may lie beyond a program’s open time window for evaluation.
Second, the growth of sophistication in technology should be considered. New programmers and ideas reshape technology like VR or AR devices and software regularly. A clinical simulation program must objectively ask if the chosen technology is going to remain viable for a long enough period to have a successful return on investment.
In healthcare simulation, the learners are the priority and the reason why any institution or facility should decide on implementing VR or AR simulation technology. A shiny new toy may not be the best use of a limited budget, or the technology could be the ticket to encouraging increased learner engagement. Taking a step back to weigh the pros and cons, as well as taking a logical look at the technology and the potential short and long-term impact on a healthcare simulation program will aid in making a decision that ultimately gives back to the healthcare learners using these resources.
Learn More About XR in Healthcare Simulation
Kirk Atkinson is a Navy Veteran with over 15 years of experience in medicine and healthcare simulation. He started his path in medicine as a Hospital Corpsman, and deployed to Afghanistan in 2010 with the 1st Medical Battalion.
When back in the U.S., he was given the opportunity to help develop a medical simulation training platform for deploying medical units based on Camp Pendleton, California. After 1st Medical Bn, he was assigned to Naval Hospital Camp Pendleton, where he was the Training Site Faculty and Administrator for the BLS, ACLS, and PALS programs. He also became a TCCC and CLS instructor for forward deploying Corpsmen and Marines.
After the Navy, he moved back to Texas where he was hired by the American Red Cross and an urgent care facility. Then an opportunity arose at UT Southwestern for a Simulation Educator/Simulation Operations Specialist.
Atkinson currently works with a very talented team to deliver high-quality healthcare simulation to all of the UT Southwestern system.
Sponsored Content: