AHRQ’s CANDOR Toolkit Helps Ensure Safer Patient Safety Response
The Agency for Healthcare Research and Quality (AHRQ) provides a number of patient safety tools and training materials, including the Communication and Optimal Resolution (CANDOR) toolkit. This patient safety resource essentially gives hospitals and health systems a roadmap for responding when a patient is harmed. The toolkit includes eight different learning modules, each containing PowerPoint slides with facilitator notes. This resource was designed in response to the potential for medical errors to harm patient safety.
Further, the toolkit was based on expert input and lessons learned from the Agency’s $23 million Patient Safety and Medical Liability grant initiative launched in 2009. According to AHRQ, “despite the best efforts of hospitals, doctors, nurses and other healthcare professionals, about 1 in 10 patients is harmed by the care they receive. Harms such as hospital-acquired infections or medication errors can happen during any stage of care.”
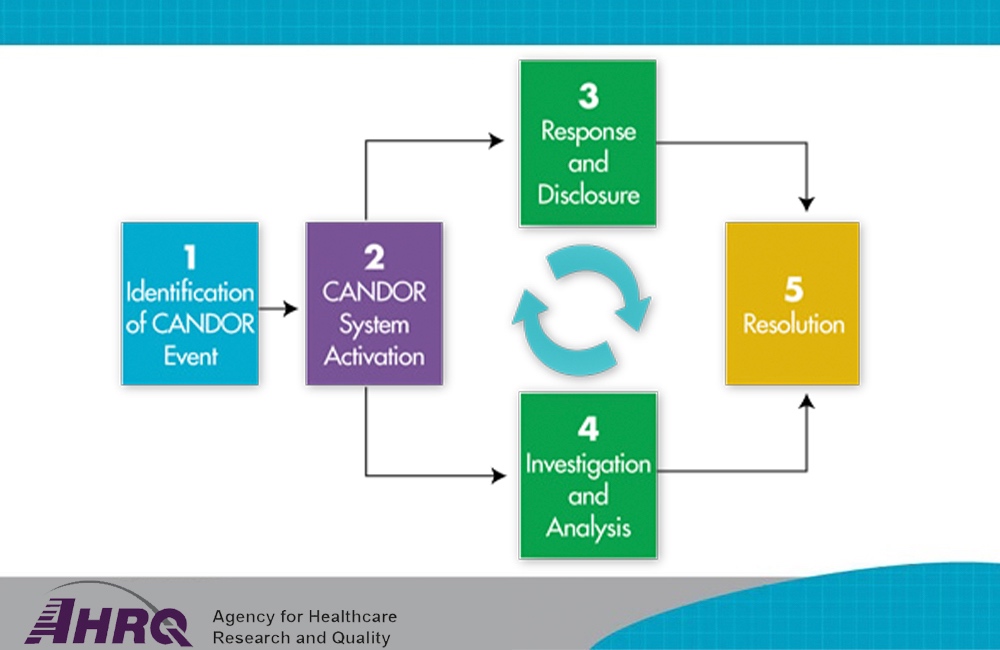
The CANDOR process begins with identification of an unexpected event that involves physical, emotional or financial harm. This activates the initiation of coordinated post-event processes. Depending on the activated CANDOR system, the learner will progress to either “response and disclosure” or “investigation and analysis.”
Sponsored Content:
The final step in the process is a “resolution” module. This module defines the CANDOR process resolution component, the steps of the resolution process, and the roles of the resolution team and other stakeholders. Ultimately, the CANDOR toolkit modules assist organizations in implementing each of these phases:
- Phase I: Assessments:
- Module 1: Overview of the CANDOR Process.
- Module 2: Obtaining Organizational Buy-In and Support.
- Module 3: Preparing for Implementation: Gap Analysis.
- Phase II: CANDOR Process Implementation:
- Module 4: Event Investigation and Analysis.
- Module 5: Response and Disclosure Communication.
- Module 6: Care for the Caregiver.
- Module 7: Resolution.
- Phase III: Organizational Improvement and Sustainment:
- Module 8: Organizational Learning and Sustainability.
Generally, organizations can expect that it will take at least 12 to 18 months to implement the CANDOR process. A CANDOR Implementation Team is responsible for the organization-wide implementation of the CANDOR process.
AHRQ recommends that the CANDOR Implementation Team Leader should be a senior leader with influence and authority to make decisions, and to support the widespread culture change associated with the CANDOR process. He or she is responsible for ensuring that individual team members have what they need to implement the steps they own in the CANDOR process. The CANDOR Implementation Team Leader is also responsible for recruiting diverse team members who will be responsible for guiding key processes during implementation of the CANDOR process.
Another AHRQ recommendation is that the team leaders should schedule an introductory meeting with all team members to orient the team to the project. Leaders should promote the organization’s commitment to this change of process using existing communication vehicles such as posting flyers in public areas of the building; including information about the project in the organization’s newsletter (if applicable); and announcing the opportunities to serve on teams at staff, patient, and family council meetings.
Sponsored Content:
Together, team members can perform a Gap Analysis, which is used to help them establish a baseline from which to measure change over time. Prior to implementation, information provided in the Gap Analysis and the metrics defined in the Building the Business Case Worksheet will provide them with a starting point to identify the data they wish to collect to evaluate the short- and long-term success of CANDOR process implementation.
Through activities like these, the overarching mission of implementing the CANDOR toolkit is to help institutions and organizations to improve the overall quality of healthcare by making patient safety the primary goal. The resource is also intended to engage patients and families in disclosure communication following adverse events. Another goal is to help organizations implement a Care for the Caregiver program for providers involved in adverse events. Other goals include:
- Investigating and analyzing an adverse event to learn from it and prevent future adverse events.
- Reviewing and revising the organization’s current processes to align with the CANDOR process.
- Establishing a resolution process for the organization.
“At its heart, CANDOR is aimed at stimulating patient safety and optimal patient care … It is only through honesty that we can identify our problems and improve. By focusing on safety improvement, the claims crisis will take care of itself.” said Richard C. Boothman, J.D., chief risk officer of the University of Michigan Health System.
Example of CANDOR Program Implementation
MedStar Health saw danger in the inability to resolve events that have caused serious patient harm. As a result, the healthcare system chose to initiate a five-year strategic plan to improve patient safety at the system’s 10 acute care hospitals and 250 ambulatory care sites in 2012.
In 2013, MedStar collaborated with leaders from around the United States to develop and pilot test the CANDOR toolkit. In partnership with AHRQ, MedStar piloted the toolkit in eight hospitals. Then, in 2015, MedStar extended the implementation of CANDOR to all 10 MedStar hospitals, having since expanded into all ambulatory care sites and diversified business units.
According to MedStar, CANDOR is now initiated whenever a serious patient harm event is reported. This follows an immediate investigation at the local care site, a discussion with the patient safety and local care team, and early communication with the patient and family. CANDOR implementation also follows the activation of the health system’s critical incident response process, including care for the care teams; notification of leadership; and claims and risk management.
To describe the lessons learned after implementing the comprehensive contemporary communication and resolution program at MedStar Health, several researchers published the study, “Lessons learned from implementing a principled approach to resolution following patient harm.” This research suggests that the overall resolution process is complex, and improvements can be made in support of organizational transparency. For example, MedStar is committed to patient safety and recognizes the importance of partnering with patients and/or families to prevent serious patient harm from happening to others, thus leading to the implementation of the CANDOR toolkit.
Learn More About the CANDOR Toolkit
Lance Baily, BA, EMT-B, is the Founder & CEO of HealthySimulation.com, which he started while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas back in 2010. Lance is also the Founder and acting Advisor to the Board of SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife Abigail Baily, PhD live in Las Vegas, Nevada with their two amazing daughters.
Sponsored Content: