To Moulage or Not to Moulage, There is No Question!
“When I do it correctly; I gain experience. When I do it poorly; wisdom. Mistakes are the portals of discovery.”
-James Joyce
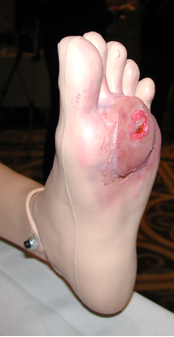
In this latest post, healthcare simulation moulage expert Bobbie Merica of Moulage Concepts reminds us just how powerful moulage can be to engage learners into medical simulation, as well as shares her secret recipe for successful wound drainage and secretions! Bobbie writes:
Sponsored Content:
Imagine This Scenario:
It is 0900 on a Monday morning at your Simulation Center. A large group of nursing simulation students have separated into blended learning stations in the adjacent conference room and you are prepping the first of many nervous looking participants for their “sterile dressing change” scenario. You offer a last minute piece of encouragement as they head off to receive report, “don’t worry, you are going to do great. Remember, this is no different then the clinical setting……”
Report to SRN:
0645: Good Morning, in room 228 is Laney Miller, a 60y female for Dr. Bryant. Ms. Miller is a type 2 diabetic who was admitted yesterday for blood sugar control and debridement of left foot ulcer. Ms. Miller weighs 109 kg and is on an 1800 cal. ADA diet. Her a.m. vitals were all normal and graphed in her patient chart per the floor CNA. Ms. Miller’s blood sugars were running high yesterday and we gave her insulin twice during the day according to her sliding scale. During my p.m. assessment I noted there was a small amount of light bloody drainage on her wound dressing which I measured and outlined with a marker; I did not change her dressing as it was well applied and Ms. Miller was beginning to doze off.
Sponsored Content:
Dr. Bryant has her scheduled today at 1100 for a 2nd wound debridement and has left new orders in her chart- including a wet-to-dry dressing change this a.m. Ms. Miller just rang her light for bathroom assistance; she has a bedside commode, and I told her there would be a change of shift with a new nurse who would be in to take her AS blood sugar, assessment and apply a dressing change. Breakfast will be here shortly but the aide has been instructed to hold it until you are finished. I need to go; I have to drop off my kids for school-do you have any other questions?
Scenario #1:
The students proceed into the simulation suite and following introductions move quickly to the tasks at hand. While one student listens to heart and lung sounds, the other begins to assess the left foot; preparing to begin the sterile procedure. A quick assessment of the foot reveals a clean, dry and intact wound dressing. The student looks slightly confused and reviews her handwritten notes regarding the patient report.
SRN #1 to patient: “Ms. Miller, has someone already been in to change your wound dressing this morning?”
Simulator: “I don’t think so; the last person who came in just took my blood pressure and temperature.”
A loud voice comes over the ceiling speaker: “Just pretend the dressing is saturated with a serous fluid and there is a wound underneath….”
The students exchange glances…..
The scenario continues with both students working quickly and effectively to meet most objectives; the patient assessment is finished, the wound dressing is changed and the simulation is “called” by the instructor.
During the debriefing, the attention is brought back to SRN #1 and her sterile technique during the procedure.
Instructor to SRN #1: “I noted you pulled the wrong gloves, the non-sterile ones…… While your overall technique was good, the non-sterile gloves compromised your entire field.”
SRN#1: “Yah, I know they weren’t sterile; they were the first gloves I saw, so I just pretended they were……”
Instructor to student: If you recall, we discussed this in the orientation/training. During healthcare simulation you are not to pretend, you should proceed exactly as you would in the clinical setting.
The students exchange glances….. OR
Scenario #2:
The students proceed into the simulation suite and following introductions move quickly to the tasks at hand. While one student listens to heart and lung sounds, the other begins to assess the left foot; preparing to begin the sterile procedure. A quick assessment of the left foot reveals the extremity is significantly cooler than the right prompting the student to ask the patient further evaluation questions regarding sensation, wound history and home care.
The SRN carefully removes the stained 4×4 dressing to reveal a “stage 3” ulcer with purulent, odorous drainage. The student catches her breath and instinctively wrinkles her nose before quickly composing herself as the now exposed wound drainage begins to permeate the simulation suite. The patient observes the SRN’s reaction and apologizes for the odor. The SRN, now embarrassed and unsure of how to respond, mumbles something inaudible and quickly finishes her dressing change without saying another word. The two SRN’s meet objectives and the scenario is “called.”
Debriefing:
Instructor to SRN #1: “What were your primary concerns in this case?”
SRN#1: “My primary concern was the sterile dressing change.” The student quickly followed with “But when I exposed the wound, I wasn’t prepared for the smell of the infection, and then I didn’t know what I should say to the patient…… I didn’t want to lie to her about the smell- because it really did smell bad, but I didn’t feel I should agree with her either….”
Prior to moving forward with the remaining debriefing questions, the instructor opens a round table discussion regarding appropriate responses to difficult questions, acknowledgments of concerns, suitable replies to delicate situations and how a lack of response may be perceived by the patient.
With moulage, all the students agree; they are gaining both experience and wisdom from their simulation scenarios!
Now learn to create your own infectious wound drainage that will engage all your simulation senses:
Drainage / Secretions Moulage
Wound drainage presents itself in a variety of situations; often the drainage is as diverse as the situation. Prior to beginning your moulage, consideration should be given to volume, consistency and odors to assist you in authenticating the scenario you are creating. When crafting your wound drainage, consider the following factors: What type of wound is it? Where is it located? What is the over-all health of the patient?
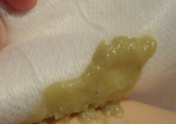
Purulent, odorous drainage moulage for healthcare simulation:
- 1 tsp. (condensed) cream of mushroom, chicken or split pea soup
- 2 tsp. Limburger cheese
- 2 drop Kimchee (Chinese seasoning)
- 4 drops water
- Caramel food coloring; thinned
In a small bowl combine cream soup, Limburger cheese, Kimchee and 2 drops of water. Stir mixture well for approximately 1 minute or until thoroughly combined. On wax paper, thin 1 drop of caramel food coloring with 2 drops of water, stirring well with small paint brush. Swirl paint brush with caramel coloring through purulent mixture to impart coloring and add depth.
Environmental Settings:
Using a small paint brush, apply purulent drainage to 4×4 wound dressing, gauze pads, and internal cavities and crevices of dimensional wounds. Use in conjunction with diabetic foot ulcer and wound dressing drainage. See: MoulageConcepts.com for more recipes.
Clean Up:
Using soft, damp cloth; wipe odorous drainage from skin of simulator. Treated dressings, gauze pads and wounds can be stored in the freezer indefinitely. Allow mixture to come to room temperature before proceeding to scenario. To refresh odor: Add 1 drop of Kimchee to dressing.
Time Saving Hint:
Odorous drainage can be made ahead, stored, covered, in the freezer or refrigerator. To reconstitute, add 2 drops tap water and stir several times.
“Wound Drainage” Dressing for Medical Simulation:
- 1 cup green tea; brewed, cooled
- 1 cup black coffee, cooled
- 2 20cc syringes
- Red watercolor marker
- 4×4 dressings, gauze dressing
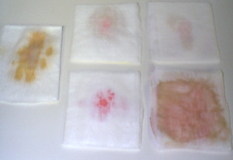
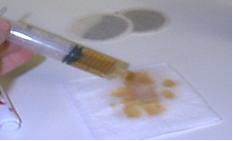
Serous drainage:
Fill (1) 20cc syringe with coffee and (1) 20cc syringe with tea. To a 4×4 dressing or wound dressing of choice, add (1 drop at time) of either mixture, slowly to center of dressing. The color will concentrate at (the site of dripping fluid) center, while feathering out as the dressing absorbs the fluid. Feathering should not exceed ¾ inch to edges. Allow dressing to sit for approximately 24 hours at room temperature or until fully dry.
Blood-tinged drainage: Fill (1) 20cc syringe with coffee and (1) 20cc syringe with tea. To center of 4×4 dressing or wound dressing of choice, create a small circle (approximately the size of a nail head) using red watercolor marker. Working quickly, add (1 drop at time) of coffee or tea mixture slowly over pen mark. The red of the pen will start to dilute and feather out as the dressing absorbs the fluid. Feathering should not exceed ¾ inch to edges. Allow dressing to sit for approximately 24 hours at room temperature or until fully dry.
Environmental Settings:
Use dressings in conjunction with any surgical case, wound dehiscence, diabetic foot ulcer, sterile dressing change or to authenticate a simulation scenario.
Clean Up:
Treated dressings and gauze pads can be made in advance and stored, dried in Moulage box indefinitely.
In Conclusion:
We hope this helps with your Healthcare Simulation Moulage! Please stop by and say hello at www.moulageconcepts.com, where you can learn more about “Bridging the Gap” in simulation.
Wishing you great success in all your Moulage endeavors!
–Bobbie Merica, Author/Business Owner of MoulageConcepts.com
Lance Baily, BA, EMT-B, is the Founder / CEO of HealthySimulation.com, which he started in 2010 while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas. Lance also founded SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife live with their two brilliant daughters and one crazy dachshund in Las Vegas, Nevada.
Sponsored Content: