Healthcare Simulation News Updates From Around the World – December 2018
Each month we take a look at the latest healthcare simulation news from programs and companies from around the world, to highlight the continued growth of this emerging professional industry. From new Sim Centers and grant purchases, to IPE simulation and Military training engagements, and from new startups to new product innovations — this is the latest medical simulation from around the world! Share your news stories through our quick article submission form!
Sinclair continues to add programming for high-demand fields including Simulation: Other jobs-focused courses available to students this year include a new professional pilot certificate program and an Associate of Applied Science degree in health care simulation technology. The short-term pilot program is designed to allow students to earn Federal Aviation Association credentials and ratings to become a professional pilot, and the applied science degree is meant to prepare students for the development and delivery of healthcare simulation.
GPH runs outbreak simulation: As health professionals practiced the simulation of a surge in patients, staff at the West Central District Health Department began investigating to learn more about the disease, Wheeler said. Health professionals that treated the “patients” were given anti-viral, personal protective equipment — such as gowns and gloves — to prevent themselves from getting sick in the outbreak. The drill was completed in about two hours, with another hour for debriefing, Wheeler said. All in all, participating agencies did well, she said. Priority Medical Transport was originally scheduled to help transport the surge in patients, but had too many real-world patients to do so, Wheeler said.
Sponsored Content:
CNR Opens New Simulation Clinic At Nursing School: Nursing students at The College of New Rochelle School of Nursing & Healthcare Professions got the chance to show off their clinical practice skills on Tuesday, December 4 during a demonstration of the College’s newest high-tech simulated hospital center. Like a real hospital, CNR’s new $100,000 facility has an intensive care unit, EKG machines, intravenous pumps, and carts to simulate dispensing medication and entering electronic medical records. But the highlight of the demonstration were two high-fidelity mannequins that can mirror a wide range of medical conditions and provide lifelike patients on which students can hone their skills.
Simulation program at SDSU gets provisional accreditation: South Dakota State University’s College of Nursing has been granted provisional accreditation for its simulation program. The Society for Simulation in Healthcare will formally recognize the college Jan. 26, 2019, in San Antonio. The society currently has accredited 126 entities in 15 nations. South Dakota State is one of the first land-grant universities to earn this achievement. SSH accreditation is a peer-reviewed, customized evaluation of a health-care simulation program. Accreditation examines the simulation program’s processes and outcomes in: assessment; research; teaching/education; and systems integration. “This is a stamp of quality and excellence,” said Assistant Dean Leann Horsley, who led South Dakota State’s efforts toward accreditation. She said the college sought provisional accreditation and after two years of data have been obtained, the college will apply for full accreditation.
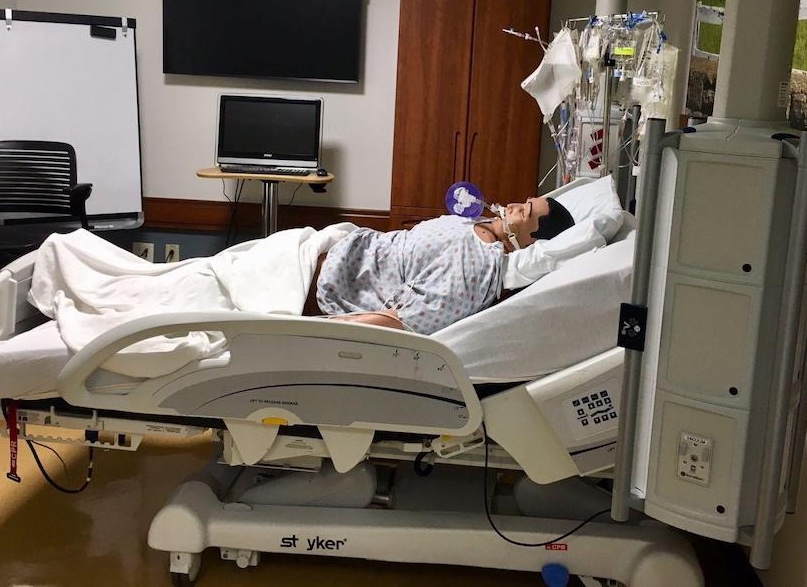
‘It will talk to you’: UK patient simulators give realistic training: Consisting of three patient rooms on the second floor of the hospital, the UK HealthCare Simulation Center provides a realistic training environment for future health care providers and advanced technology for current researchers, UK HealthCare officials said. In each patient room there is a simulator, which could very easily be mistaken for an actual human as they look and act like real people. The center features an Intensive Care Unit, an Operating Room and a Flex Room. Students and researchers use these rooms and simulators in order to produce the most accurate and real-life situations that they’re likely to encounter in the real world. There are five simulators and each one is meant to help train different things. HPS, the Operating Room simulator, is worth $250,000 and for a good reason. “It can duplicate almost all human physiology that you could think of. It cries, it seizes, it will vomit, it will talk to you,” said Dr. Zaki Hassan, a professor of anesthesiology and surgery. “If you give (the simulator) a drug, it will recognize what drug it is and the concentration. It will recognize the drug, the concentration and the volume given and will respond appropriately.” P(Photo provided by Ramakanth Kavuluru).
Medical Simulation Startup Wins Top TechCelerator Prize: The judges ultimately selected Medulate, which is creating a suite of startup simulators to increase efficiency and effectiveness of medical education, with products for all levels from nursing programs to surgical residency. Medulate was co-founded by Scarlett Miller and Jason Moore, both associate professors in Penn State’s College of Engineering. Miller is an expert in engineering design human factors product design and Moore is an expert in robotics and tissue modeling. “We’re thrilled we were able to convince others to believe in our company as much as we do,” Miller said in a news release. “This money means a lot as we build our business and improve the educational experience for medical students. If you asked us three months ago that we would be in this position, we wouldn’t have believed you. Thank you to Ben Franklin and Invent Penn State for this incredible opportunity.”
Sponsored Content:
KGS TraumaDX Wins NTSA Award for K9 Simulator: TraumaFX, a division of Kforce Government Solutions (KGS), received the National Training and Simulation Association’s (NTSA’s) Modeling and Simulation Acquisition Team Award for helping create K9 Diesel. K9 Diesel is an advanced simulation tool made to improve the ability of first responders and veterinary professionals to save working dogs’ lives. The man-made patient includes 28 different features and medical intervention sites, complete with full anatomical skeletal motion, audio queues, such as barking and growling, and CPR chest compression with resistance. The company and extended team were recognized for outstanding achievements in government-industry collaborative development and fielding of a new medical simulation capability to better meet the unique training needs of special operations.
Dental, EMS, and nursing students collaborate for medical simulations at PPCC: During the simulation, the dental students recognize the issue and start basic care. It’s not just dental emergencies – students saw simulations of issues like choking, allergy complications, seizures, and chest complications. The dental students then call EMS students, who stabilize, assess, transport and give life-saving medication. From there, the patient is then passed to the nurses who work with the physician to reassess the patient and give a further diagnostic. This is the first time that these three programs have run a simulation together. “Dependently, the programs here under the Allied Health umbrella at Pikes Peak Community College do simulations, we’ve just never conducted simulation together, so this is a first of its kind,” Wilk said.
PNU Has the Largest Simulation Center in the World for Medical Experimental Education: Princess Nourah Bint Abdulrahman University has established the largest simulation center for medical education and training in the world. It is designed in the form of a hospital in which students practice realistic medical scenarios and medical cases in a guided environment that uses more than 224 interactive medical dummies and virtual reality equipment to provide a reality-like environment between a patient and a doctor. The trainees experience new, rare, complicated and urgent situations, which may happen in real life. The Center achieves one of the University’s strategic objectives by equipping students with the skills to succeed in life, offering an environment for innovative learning that focuses on the students, and providing high-quality curricula that prepare students for success and make them capable of entrepreneurship and earn professional ethics.
US Army Emergency medicine residents prepare for battlefield medicine: Carl R. Darnall Army Medical Center’s medics, nurses and doctors continually train through various venues to ensure they are providing the most up to date evidence-based medical care to the Soldiers and families here. But ensuring the readiness of the force is only one part of their job. They must maintain their own readiness, as Army Surgeon General Lt. Gen. Nadja West has directed Army medicine to focus on readiness and modernization to modify or create capabilities to better support warfighters’ needs on the battlefield. “Emergency Medicine Residency Program graduates will be heading to a FRST or a field hospital, so it’s critical they get the experience of what they will be facing downrange,” he said. The main thing that I stress to my residents, is that when they graduate from the program, they know hospital care really well. But it’s a challenge to utilize your skills in an austere environment.”
Doctors hone craft in Las Vegas hospital’s new simulation center: The high-tech dummy is one of several training tools in MountainView Hospital’s new simulation center to help medical residents learn basic operations and procedures before they begin working on the living. The hospital unveiled the facility and introduced Harold and his counterpart, a pregnant woman named Lucy, at an open house Tuesday. “The simulation allows the residents to get that real-life, hands-on experience,” said CEO Jeremy Bradshaw. “If they’re going to make a mistake, we want them to be able to do that on a simulated patient.” The simulation center, open 24/7, is available to about 150 residents at MountainView and Southern Hills Hospital and Medical Center as part of the Sunrise Health Graduate Medical Education program. Both facilities are part of the Sunrise Health system, which includes Sunrise Hospital and Medical Center and Sunrise Children’s Hospital.
This Tri-Cities hospital is using human simulators to save lives: He’s not a person, but a human-like piece of equipment used to help Kadlec Regional Medical Center employees prepare and practice for real-world situations with real-life patients. In medical parlance, Stan is a “high-fidelity human patient simulator.” Kadlec has several simulators in its simulation lab — from a tiny preemie to 170-pound Stan. “(Simulation) is, by far, the most effective educational tool for improving people’s clinical performance,” said Mike Anderson, who runs the lab. “You can read and look at videos all you want, but until you stand there and feel a pulse, until you do the chest compressions, until you do all that stuff — it’s a huge, huge advance in learning.”
Simulation training in palliative care: state of the art and future directions: The growing need for palliative care (PC) among patients with serious illness is outstripped by the short supply of PC specialists. This mismatch calls for competency of all health care providers in primary PC, including patient-centered communication, management of pain and other symptoms, and interprofessional teamwork. Simulation-based medical education (SBME) has emerged as a promising modality to teach key skills and close the educational gap. This paper describes the current state of SBME in training of PC skills. In a total of 78 studies, 76% involved learners from medicine and 38% involved learners from nursing, while social work (6%) and spiritual care (3%) learners were significantly underrepresented. Only 16% of studies involved collaboration between participants at different training levels.
Subscribe to our free bimonthly newsletter for all the latest Simulation News!
Lance Baily, BA, EMT-B, is the Founder / CEO of HealthySimulation.com, which he started in 2010 while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas. Lance also founded SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife live with their two brilliant daughters and one crazy dachshund in Las Vegas, Nevada.
Sponsored Content: