New York Times Covers Growing Use of Simulation in Healthcare
While usually we cover news stories once a month like our recent Global News Update for Healthcare Simulation in October article, coverage by The New York Times warrants its own celebration. Last week writer Laura Pappano published “Training the Next Generation of Doctors and Nurses” which covered the expanding use of patient simulators and virtual reality in medicine to train tomorrow’s healthcare professionals. The article covers how students “see technology as a driving force behind the improvement in health care” as it importantly provides “repeated practice”. Check out the excerpt and full link below!
New York Article “Training the Next Generation of Doctors and Nurses” Excerpts:
Repeated practice is important. But so is unscripted human interaction, which is why medical and nursing schools also are embracing nontech innovations that put students in clinical settings sooner, often outside of the hospital. Ms. Alfaro that could make visits more efficient for her future patients. “You want to do the most for your patients in those 10 minutes,” she said, so they walk out “with their needs met.”
Sponsored Content:
As schools seek to make learning more efficient, technology — including virtual reality, augmented-reality software and high-fidelity simulations (mannequins “breathe,” cry, sweat and respond to medication) — is a big part of that. And it must be, given that students have to learn more information, faster. Much of medicine is slow; you can’t shortcut taking a medical history. But visiting the pathology lab to study a colon sample?
This is where Greg Dorsainville, a multimedia developer and one of 28 full-time staff members in the N.Y.U. institute, steps in, using a 360-degree camera to film a 45-minute session with a pathologist. He cut the lesson to 5:46, time that a medical student can spare to don goggles, zoom in and see what a polyp actually looks like, making it something to be remembered as “a visual in their mind. It’s not just a concept.”
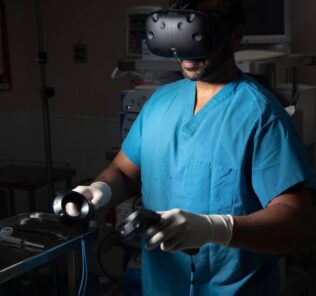
Marlene Alfaro, a second-year student at the University of California Riverside School of Medicine, can slip on goggles and — in virtual reality — call up a 3-foot 3-D image of a ruby red beating heart and, with a controller, probe its structures. In the textbook, she said, “it was hard for me to visualize the whole 360” degrees. Virtual reality “lets me see real quick how everything goes together.” No one wants to be the first human a student intubates (navigating a breathing tube down a patient’s throat), yet students have often trained on real patients.
While it can take years to develop the dexterity, control and confidence to smoothly insert a central line, lifelike simulations are giving students more chances to practice before plunging in for real.
Sponsored Content:
In replica hospital rooms fitted with bed-bound mannequins programmed to mimic conditions like strokes and seizures, and that can bleed, blink and give birth (there’s even a realistic placenta), students get “deliberate practice,” said Robert Morgan, director of the Greenville Health Care Simulation Center in South Carolina, which is used by the University of South Carolina School of Medicine, Greenville and Clemson University School of Nursing. Rather than hope to encounter a teaching opportunity in the hospital, Dr. Morgan said, “you come here and start your first 10, 15, 100 I.V.s before you actually have to place one in a patient.”
Read the Full New York Times Article Here!
Lance Baily, BA, EMT-B, is the Founder / CEO of HealthySimulation.com, which he started in 2010 while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas. Lance also founded SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife live with their two brilliant daughters and one crazy dachshund in Las Vegas, Nevada.
Sponsored Content: