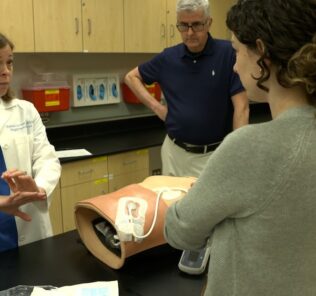
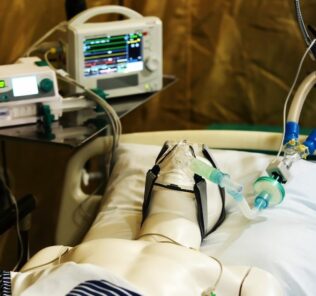
How to Build Resilience into Your Clinical Simulation Program
The need to build resilience in a healthcare simulation program team is of great importance. A resilient team enables response to alterations in plans and unexpected events. As psychological safety is so incredibly paramount in clinical simulation, there is a very high importance placed on the ability of clinical simulation educators to adapt to participant requirements in the moment and cope with these changes. As a global collective, attempts are being made to draw in, educate, and retain healthcare staff. The resilience of healthcare simulation programs is crucial to educate the next generation of healthcare workers. A resilient clinical simulation program is a successful clinical simulation program. This article by Erin Carn-Bennett, MSN, RN, will explore critical steps for leaders and team members of clinical simulation programs to build and enable resiliency now and in the future.
People Progression Requires Unique Attention
The most valuable asset in any healthcare simulation program is the people who work in the clinical simulation program. Investment in staff members of a clinical simulation, both personally and professionally, will pay off over time. Simulation staff investment may come in the form of mentorship or supervision within the team and external to the clinical simulation program to enable an acceleration of professional development. Growth and progression of individuals will also occur with attendance to a variety of educational courses.
Sponsored Content:
A high value and importance placed on education will enable staff to seek out and make time to attend a variety of courses that will progress them as a member of the clinical simulation team. In-person or hands-on education is often the most valuable, but online courses, webinars, and conferences should also be considered. Clinical simulation conferences are incredibly vital to the progression of team members. Connections made at local and international conferences can be invaluable to share and gather resources from others. If only some team members could attend an educational program, a post-conference report or presentation for other team members could be useful to share the experience amongst the team. A team value of lifelong learning means that team members emphasize education of all modalities to enable team growth and development.
Growth Mindset from Adversity
Mistakes will be made and are part of life. Healthcare simulation is no different, and mistakes should be welcomed and explored in a psychologically safe manner. There should be processes in place to review and debrief certain levels of courses, if not all, within healthcare simulation programs. A structured approach to post-course debriefing and after adversity is an essential opportunity for team growth, which should be noticed.
A preset document template to fill in post courses from the faculty perspective alongside participant feedback is important to keep on file. Any adverse events or errors should be explored as a team with curiosity and without judgment. Errors should be welcomed and normalized to assist with the growth of resilience in clinical simulation programs. Learn more about developing a growth mindset in clinical simulation.
Sponsored Content:
Communication and Psychological Safety
Team communication on a daily basis matters, as does the manner in which this is conducted. To foster and encourage psychological safety in a clinical simulation program is critical to resilience and the acceleration of innovation and creativity. When team members feel able to share ideas freely to challenge the status quo without fear of reprimand, this contributes to the team’s strength and resiliency.
Care of the Team Means Better Care
Care of the clinical simulation program staff is critical as burnout is at an all time high post covid. Build resiliency in the clinical simulation program with wellness initiatives and rituals. These can be as simple as team coffee every morning and lunchtime walks outside in nature. Placement of importance onto simple care aspects, such as support of staff with flexible work conditions, can be invaluable to build resilience in a program.
View the HealthySimulation.com LEARN CE/CME Platform Webinar Simplifying Simulation: Empowering Educators to Deliver Meaningful Experiences to learn more!
Preparedness and Contingency Plans
The unexpected will generally happen when hosting a clinical simulation course. Resilience in a clinical simulation program is the ability to respond to these events and not impact the course overall. This circles back to the importance of development and investment in team members. A forward and growth vision will enable the team members to have opportunities to present and progress themselves when ready and able before the unexpected happens.
Consideration of contingency plans for when the unexpected happens will also assist with resiliency in a clinical simulation program. Have enough faculty for a clinical simulation course that if a team member cannot make the course, other options can take their place. Consider the amount of staff in the clinical simulation program and how many hours each work. For some programs, more staff with fewer hours can add a lot of breadth to their clinical simulation program. For larger courses external faculty may be required to be able to add resilience.
Empathetic Leadership Empowers Teams
Empathy and emotional intelligence are incredibly essential in all healthcare leaders. These skills will assist in the retention of staff. Leadership that places an emphasis on team growth can be an invaluable asset to the progression and retention of a resilient clinical simulation program. This leadership style can be enhanced by team activities such as team planning days that provide an overview of where the team is currently and the future aims. When leadership shares down and allows team members to have input into the program’s direction, this can enhance the team greatly and add to resiliency through staff that feel valued and able to contribute.
Regular team meetings, ideally on a monthly basis with minutes taken, allow for staff to have their voices at the table with clinical simulation leadership. This input can contribute to steering the clinical simulation program, which can be rewarding for team members to experience. Monthly meetings are also an opportunity for team members to share the progress of projects and new connections that others may have yet to be aware of.
This article has explored possible ways clinical simulation teams can build resilience into their clinical simulation program. Strategy, as described, to build a resilient clinical simulation program can be essential to the longevity of a healthcare simulation program. With care and a main focus on the progression of people, a sustainable and resilient healthcare simulation program is possible.
Learn More About Improving Patient Outcomes and Building Resiliency!
Erin Carn-Bennett is a Simulation Nurse Educator for the Douglas Starship Simulation Programme in Auckland, New Zealand. Carn-Bennett has her Masters of Nursing and has an extensive nursing career within pediatric emergency and also nursing management. She is passionate about debriefing and all things simulation. Carn-Bennett is a member of the IPSS board of directors. Carn-Bennett is the lead host of the podcast Sim Nurse NZ.
Sponsored Content: