How to Incorporate Ethical Awareness in Healthcare Simulation Practice
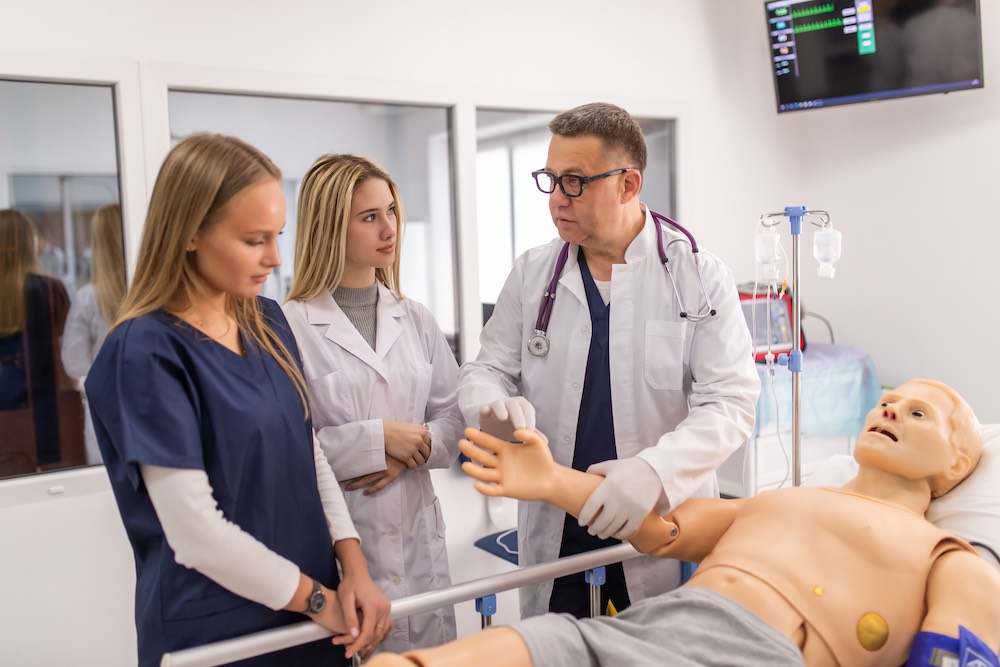
Simulation-based learning activities have become an important component of healthcare education. The practice is of great relevance and should comply with all International Nursing Association for Clinical Simulation and Learning (INACSL) Healthcare Simulation Standards of Best Practice. Designed to advance the science of medical simulation these standards provide guidance that benefits educators and learners, helping them navigate through the academic simulation experience. One of the INACSL Standards is postulated as professional integrity, which refers to the ethical behavior that is expected of all participants (teachers and learners) in the simulation experience. The Society for Simulation in Healthcare (SSH) has similarly developed a comprehensive “Healthcare Simulation Code of Ethics” which is shared and discussed here as well. This HealthySimulation.com article explains how to incorporate ethical awareness in healthcare simulation practice.
Components of the Design of Ethical Clinical Simulation Experiences
In the construction and design of a healthcare simulation experience, having three principal factors in mind is essential. They are the learners, educators, and designers. In terms of learners, the educator or instructor is responsible for fully engaging learners in the healthcare simulation experience. Yet, the learners must also come prepared with foundational knowledge, ready to engage in a self-assessment – leading to self-regulated learning and ethical behavior.
Sponsored Content:
Healthcare Simulation educators are additionally responsible for providing comprehensive pre-briefing information and promoting a safe environment. They must incorporate the appropriate fidelity to enhance realism. They must also ensure that they will not negatively influence the simulation while being transparent with their actions and ethical behavior. The design of the healthcare simulation environment should never be harmful or potentially dangerous. Learning objectives must be clear and measurable while being supported by the principle of justice and asserting key aspirational values.
Actors involved in a clinical simulation need to be involved in the simulated scenery, through which the learner must work to solve the clinical problem. The scenario is designed and raised by the educator to know the clinical skill acquired in a certain area. This interaction is framed by specific aspects: attributes, standards, concepts, and ethical principles.
Healthcare Simulation Code of Ethics
On January 13, 2018, a group of healthcare simulationists from around the world collaborated on a unifying open access Healthcare Simulation Code of Ethics from the Society for Simulation Healthcare. The code was designed to assert aspirational values at the highest, general level for all healthcare simulation professionals. The Healthcare Simulationist Code of Ethics asserts key aspirational values important to the practice of simulation: Integrity, Transparency, Mutual Respect, Professionalism, Accountability, and Results Orientation. The Code identifies values important to the welfare of all parties in the healthcare simulation community of practice, and it asserts our identity and commitment to healthcare simulation as a profession. The goal is for the code to help develop key aspirational values that are important to the practice of simulation. Values that must be incorporated into daily practice include:
Sponsored Content:
1. Integrity: Healthcare simulationists shall maintain the highest standards of:
- Respect
- Honesty
- Truthfulness,
- Fairness
- Judgment
2. Transparency: Healthcare simulationists promote transparency and clarity in the design:
- Communication
- Decision-making processes
3. Mutual Respect: Healthcare simulationists shall practice empathy and compassion to support beneficence and non-maleficence towards all involved in simulation activities:
- Honor the knowledge, skills, values, and vulnerability of learners
- Listen to others
- Exhibit humane behavior,
- Maximize safety
4. Professionalism: Healthcare simulationists shall conduct themselves in a manner that upholds the professional standards:
- Demonstrate professional competence
- Continuous personal and professional development.
- Encourage and develop
- Cultivate opportunities
5. Accountability: Healthcare simulationists shall be accountable for their decisions and actions:
- Reflect on, and incorporate feedback
- Professional review
- Role models
- Exhibit professional conduct
- Identify and notify relevant aspects
- Design simulation
6. Result Orientation: Healthcare simulationists shall serve to support activities that enhance the quality of the profession:
- Assure the reliability and credible
- Engage in continuous quality improvement.
- Create and measure the impact
- Incorporated and use the Code of Ethics
- Advanced public knowledge about healthcare simulation
The Healthcare Simulationist Code of Ethics is designed to assert aspirational values at the highest, general level for all healthcare simulation professionals. The Code of Ethics is available in Arabic, Chinese, French, German, Hausa, Igbo, Irish, Italian, Japanese, Malay, Norwegian, Polish, Portuguese, Spanish, Turkish and Yoruba.
What to Expect to Incorporate the Simulation Healthcare Code of Ethics?
A comprehensive and systematic approach to the integration of the ethics simulation code allows the safe practice, improved performance, and quality. Giving healthcare simulationists the tools (values) to move the training routines to another level helps them secure the knowledge and skills needed. With these skills, the learner can go on to manage a patient’s illness in a respectful and professional way.
Learners and educators must understand that healthcare simulation serves as an integration activity. Through medical simulation, simulationists can come to transfer knowledge and act as a role models, complying with the following characteristics:
- Theoretical Knowledge
- Develop a teaching preparation
- Creating learning environments based on relevant problems, attractive and inclusive.
- Trust that students want to learn
- Demanding and having high expectations of their student’s progress
- Ethical principles
When the practice of clinical simulation develops in this framework learners will acquire knowledge in specific areas of healthcare, and they will get other valuable skills like communication, ascertain dialog capacity, empathy, and own recognition of the actions made during simulation debriefing. They will be able to assess the way the clinical simulation experience was developed and obtain objectives.
Is the Simulation Health Ethic Code Applicable in New Sceneries of Practice?
In actuality, healthcare simulation practice has been complemented and enhanced by technological tools such as immersive virtual reality simulation, interaction with virtual patients, or being involved in a simulation scene via a video conference – participating at distance. These technologies help learners and educators to make the healthcare simulation practice more realistic. This also helps facilitate access for the learners. In this type of practice, the key aspirational values of ethic codes will enhance the practical experience and optimize communication skills.
Time to incorporate Ethical Awareness into the Simulation Practice
The practice of clinical simulation has taken a place of great importance in the training and education of learners. Current evidence shows there is an urgent need to implement safe, useful, and ethical pedagogical dynamics. In addition to transmitting the knowledge of the teacher in a specific area, healthcare simulations should also be carried out training in ethical aspects. This must be contemplated within the planning of each clinical simulation practice, making them more real, universal, and above all more human. The objective is to make efficient and empathic healthcare providers.
Sharing The Experience of Incorporating Ethical Code into the Healthcare Simulation Practice
The medical simulation practice, both before and after and including the code of ethics, has presented relevant and important changes. The code has allowed for an approach to learning that keeps human aspects in mind, additionally allowing them to contemplate points within the planning that were not previously relevant. They can also identify aspects that were just being ignored and can have them optimized. The empathy and the communication of the learners with their patients should be guided by real value tools with the best interest of their future medical career in mind.
Learn More About the Ongoing Professionalization of Healthcare Simulation
Dr. Catalina Vanegas Ortiz is a medical specialist in obstetrics and gynecology. She also has a master’s degree in medical education with an emphasis on public health. Dr. Vanegas is a professor of medicine faculty the University of La Sabana, and CEO and founder of Custom Praxis.
Sponsored Content: