Lifecast Manikins Encourage Learner Engagement Through Realism
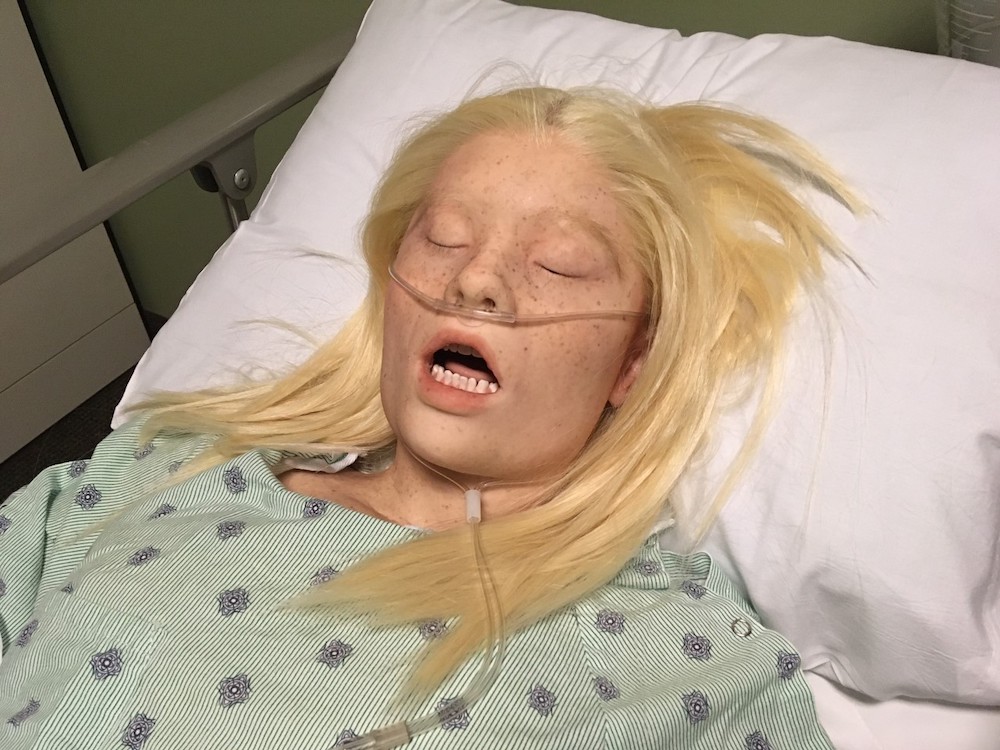
While clinical simulation is not real, healthcare educators need learners to treat each simulated learning activity as if the scenario is real, to maximize the educational benefits of simulation-based learning (SBL). The clinical simulation team at Baylor University Louise Herrington School of Nursing (LHSON) in Dallas, Texas, chose to upgrade their skills lab with Lifecast manikins in 2020 and to great effect. The goal was that the manikins’ more lifelike features would impact healthcare simulation learning, and the impact was immediate. Learners and faculty responded favorably to the individuality of the medical simulation manikins; no longer were the eight patients identical in their lifeless, plastic-like appearance. Instead, a diverse patient population is now presented with features such as freckles, facial hair, acne, tattoos and body piercings that speak to the uniqueness of each patient and elicit a more genuine interaction between the learner and patient. This article will look at how Baylor University’s LHSON considered the reasons behind creating realistic medical simulation activities and the benefits they found from doing so.
Manufactured in North America by Echo Healthcare, Lifecast manikins employ a 3D process utilized in the special effects industry, to create an exact copy of a human body. Sophisticated molding and casting techniques allow for replication of fine details such as fingerprints, pores, veins and underlying structures; they include airways and articulated mouths for practicing airway management. Now, Baylor’s manikins range in age from 16 to 89, and represent African American, Native American, Asian, Latino and Caucasian ethnicities. They also present a diverse array of chronic and acute health issues, including COPD, cystic fibrosis, diabetes, cellulitis of the right foot and a sacral decubitus.
Several factors go into creating learner buy-in for SBL; the level of fidelity, or realism, is chief among them. Fidelity in simulation is a multi-dimensional concept corresponding to the degree of realism being created through the selection of simulation equipment, setting and scenario. Fidelity also refers to the degree of exactness achieved and corresponds to the believability of the experience for participants.
Sponsored Content:
The concept of fidelity is not unidimensional; the concept is discussed in terms of levels (low-, mid- and high-fidelity) and types (physical, psychological and conceptual). There is ongoing discussion regarding the necessary level of fidelity when developing SBL: when is more better and when is more too much? The INACSL Standards of Best Practice notes that simulation design does not dictate a level of fidelity; rather, the standards state that the level of realism should be that which promotes the achievement of the expected learning outcomes.
Engagement and the transferability of learning are of prime interest to educators. Simulation activities that closely resemble real-life add a degree of authenticity that encourages engagement and allows learners to take the knowledge and skills they develop in the simulated setting and apply them in clinical practice. The type and level of fidelity required is dependent upon the skills being practiced: proficiency in technical skills is achieved with higher physical or functional fidelity; clinical reasoning and decision-making skills benefit from increased levels of conceptual fidelity, and the level of emotional fidelity impacts development of some of the so-called soft skills, such as teamwork, communication and leadership skill development.
When discussing manikins, most often, the level of fidelity corresponds to the level of sophistication of the internal computer components of the manikins. Lifecast manikins turn this correlation on its head. They exhibit an uncanny level of realism with absolutely no electronic workings. Lifecast manikins heighten all three types of fidelity – physical, conceptual, and emotional or psychological – engaging learners in ways not possible with static or low-fidelity manikins.
Lifecast manikins are available in a wide range of ages and ethnicities. They are created with the weight and height of the simulated patient and have unprecedented range of motion at all joints, thereby encouraging more natural handling and bringing a new level of realism to simulation training. All three types of fidelity are increased with the Lifecast manikins. Physical fidelity, which is important for developing kinesthetic skills that involve muscle memory, is addressed with the accuracy of the manikin’s weight, skin texture and joint fluidity. Conceptual fidelity, or the realism that facilitates formation of if-then relationships and development of clinical reasoning, is realized when the student does not properly position the patient’s head and neck when attempting to ventilate and therefore the chest does not rise.
Sponsored Content:
Perhaps psychological or emotional fidelity realizes the biggest gains with the Lifecast manikins. The intricate details and the extreme individuality of each manikin elicit an emotional response from every person who interacts with these manikins. Trainees feel a connection that is strengthened by the unique patient profile created for each manikin.
Along with addressing all types of fidelity, the Lifecast manikins also impact all three domains of learning: cognitive, psychomotor and affective. The realistic weight of the manikin, along with the increased range of motion of the joints, allow the patient to be positioned properly while practicing skills such as Foley catheter and nasogastric tube insertions. The increased realism of facial and body features, as well as skin texture, prompts authenticity in the student’s actions and responses, helping them develop empathy and caring behaviors.
Prior to the installation of the Lifecast manikins, the LHSON healthcare simulation staff noted an increasing incidence of the older manikins being treated as manikins, not patients. When questioned, students would often respond, “Well, I would never do that to a real patient, but he isn’t real.“ Or, “I would never do that in the clinical setting.“ The staff found this concerning; they wanted the students to treat simulation as real and use their time in the skills lab developing safe behaviors.
Echo Healthcare is the licensor, manufacturer and distributor of Lifecast Body Simulation Products in North America. Lifecast Body Simulation has developed a range of highly accurate and lifelike medical manikins which are transforming the way that healthcare simulation and education are delivered and absorbed. Lifecast manikins are a 3D scanned head and body of a real person with the characteristics of human features.
The artisans at Echo Healthcare worked with the LHSON sim team to create eight unique patients. According to Kevin King, CEO of Echo Healthcare, the staff at LHSON Simulation went one step further than any other customer in North America and worked collaboratively with the design team in Sarasota to customize their manikins to reflect real patients with specific conditions. “This first-of-its-kind request is groundbreaking and will allow an emotional connection between students and technology.”
Learn More About Healthcare Simulation Manikins
References:
- Carey, J., & Rossler, K. (2020). The how when why of high fidelity simulation.
StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK559313/ - Dieckmann, P., Gaba, D., & Rall, M. (2007). Deepening the theoretical foundations of patient simulation as social practice. Simulation In Healthcare: The Journal of the Society for Simulation in Healthcare, 2(3), 183-193. doi:10.1097/sih.0b013e3180f637f5
- Harder, N. (2018). Dealing with the fidelity of simulation-based learning. Clinical Simulation in Nursing, 25, 20-21. doi:10.1016/j.ecns.2018.10.004
- Kim, J., Park, J., & Shin, S. (2016). Effectiveness of simulation-based nursing education depending on fidelity: A meta-analysis. BMC Medical Education, 16(1). doi:10.1186/s12909-016-0672-7
- Rudolph, J.W., Simon, R., & Raemer, D.B. (2007). Which reality matters? Questions on
the path to high engagement in healthcare simulation. Simulation In Healthcare: The Journal of the Society for Simulation in Healthcare, 2(3), 161-163.
doi: 10.1097/sih.0b013e31813d1035 - Smink, D. S., Yule, S. J., & Ashley, S. W. (2017). Realism in simulation: How much is enough? JAMA Surgery, 152(9), 825. doi:10.1001/jamasurg.2017.1086
- Ward, G., Robinson, L.B., & Ware, L.J. (2017). Promoting caring by increasing realism
in the simulated environment. International Journal of Nursing & Clinical Practices, 4:257, doi: https://doi.org/10.15344/2394-4978/2017/257
Jeanne Carey is the Director of Simulation at Baylor University Louise Herrington School of Nursing in Dallas, Texas. She holds advanced certification as a simulation educator and has 10 years of experience in all aspects of simulation, including the development and implementation of new simulation-based learning activities, training of simulation facilitators, and recruitment and management of standardized patients. Carey and the LHSON Simulation Team created the Two-Heads-Are-Better-Than-One (2HeadsR>1) strategy for role assignment in simulation. She is active in several simulation organizations and currently serves as an INACSL Nurse Planner.
Sponsored Content: