INACSL Hayden Vanguard Lectureship: 30 Minutes of Weekly Simulation in Every Hospital Around the World
Completing her coverage of the 2020 International Nursing Association for Clinical Simulation and Learning (INACSL) Virtual Conference, HealthySimulation.com staff writer Dr. Kim Baily PhD, MSN, RN, CNE, previous Simulation Coordinator for Los Angeles Harbor College and Director of Nursing for El Camino College recaps the CAE Healthcare funded the Hayden Vanguard Lectureship entitled “Team Engagement to Improve Outcomes – Global Network for Simulation in Healthcare (GNSH) 30 Minute Initiative”, presented by Dr. Carol Durham from The University of North Carolina at Chapel Hill and Dr. Pamela Jeffries from The George Washington University School of Nursing.
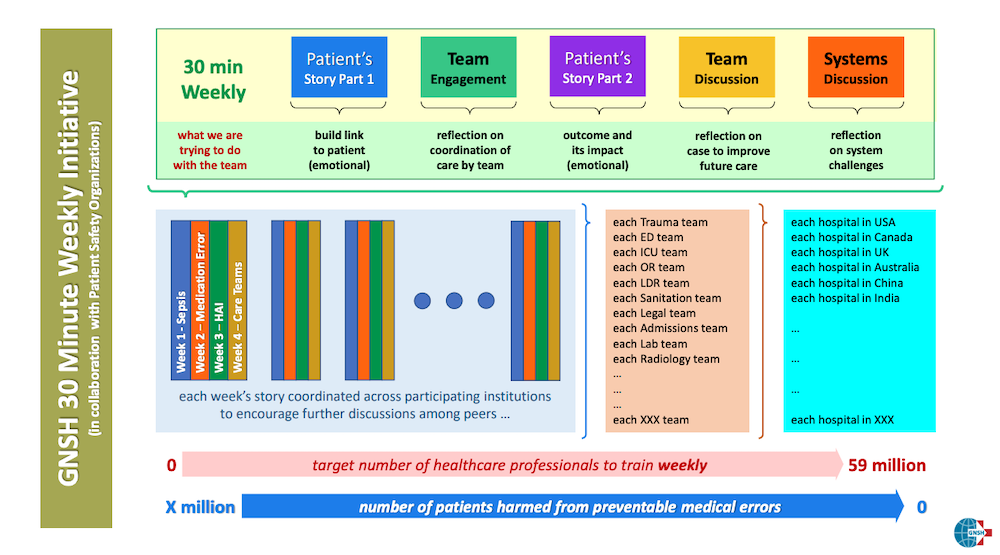
In 2010, representatives from sixteen regional, national and international organizations attended a UK summit to form a Global Network for Simulation in Healthcare (GNSH). The mission of the GNSH is to advance healthcare training through modern approaches and innovative solutions and foster a healthcare culture that empowers people and systems to maximize safety outcomes for patients and staff. GNSH began by creating a tool kit to be used by hospitals to examine the cause healthcare errors and offer suggestions for training staff. More recently the organization has expanded the tool kit to include a series of case studies based on real patient errors designed to be presented as a 30-minute weekly initiative.
The case studies use stories, team engagement, and system considerations to create a space for teams to consider ways to improve their care in a similar situation and to consider what system issues might have contributed to the outcome and how they can mitigate those within their systems. The case studies focus on 4 areas of practice, sepsis, medication errors, healthcare associated infections (HAIs), and care teams. The idea is to bring healthcare professionals together to discuss cases and learn collaboratively.
Sponsored Content:
Each scenario provides a baseline framework to build upon. The patient’s history and vitals are presented where appropriate. The scenario should be presented by knowledgeable facilitators who are encouraged to improvise where necessary. The scenario should be easily adaptable for given staff/equipment support availability and for the available simulation technology. The session should include a debrief that is interactive and fully engages every team member. The goal is for the team to jointly recognize system issues and determine how they, as a team, need to change their practice.
Five components of Case Studies:
- The patient’s story
- Short simulation (simulator, simulated patient or table-top role play)
- An opportunity for the team to discuss what they think is going on and what they are most concerned about.
- Completion of the patient’s story (final outcome).
- Team discussion related to what they could do to improve the outcome in a similar situation, what system issues may have contributed to this outcome and what checks and balances are in place in their institution to prevent the outcome in the case study.
Examples of Case Studies:
- One of the case studies presented during the lecture involved the moving real patient story of a little girl that died from a central line infection. Video included the bereft parents talking about their daughter. The case study leads the learners through a consideration of the patient’s actual life and the cause/s of the errors that led to child’s death. The materials focus on the system causes of the error and how the system and team behaviors could be changed to prevent the error occurring in the future.
- A second video told the story of a nurse who incorrectly read a glucometer and was later disciplined for the mistake. Several weeks later however, a second nurse made the same error. The hospital set about investigating the errors and concluded that there were system and human factor errors that led to misreading of the glucometer. The glucometer and blood sugar protocols changed to prevent the error from occurring again and the disciplinary action was removed from the nurse.
During the case studies, every team member is asked what system errors might have contributed to the outcome and what systems are in place to prevent the outcome happening again.
Sponsored Content:
The case study materials were designed to be used in healthcare institutions and are presented for free on the GNSH website. One of the unexpected consequences of the Covid19 pandemic and the move of healthcare education to a virtual platform is the high use of case students in academia.
Pilot Campaign: The GNSH team is seeking healthcare institutions to participate in a pilot campaign to implement the 30 Minute Initiative for 12 weeks in their facilities this year. The campaign will include a follow up research component to determine the effectiveness of the intervention. The anticipated date for the study is late 2020 however, the exact date will depend on the status of the COVID-19 pandemic.
Visit the GNSH Website to Learn More!
Dr. Kim Baily, MSN, PhD, RN, CNE has had a passion for healthcare simulation since she pulled her first sim man out of the closet and into the light in 2002. She has been a full-time educator and director of nursing and was responsible for building and implementing two nursing simulation programs at El Camino College and Pasadena City College in Southern California. Dr. Baily is a member of both INACSL and SSH. She serves as a consultant for emerging clinical simulation programs and has previously chaired Southern California Simulation Collaborative, which supports healthcare professionals working in healthcare simulation in both hospitals and academic institutions throughout Southern California. Dr. Baily has taught a variety of nursing and medical simulation-related courses in a variety of forums, such as on-site simulation in healthcare debriefing workshops and online courses. Since retiring from full time teaching, she has written over 100 healthcare simulation educational articles for HealthySimulation.com while traveling around the country via her RV out of California.
Sponsored Content: