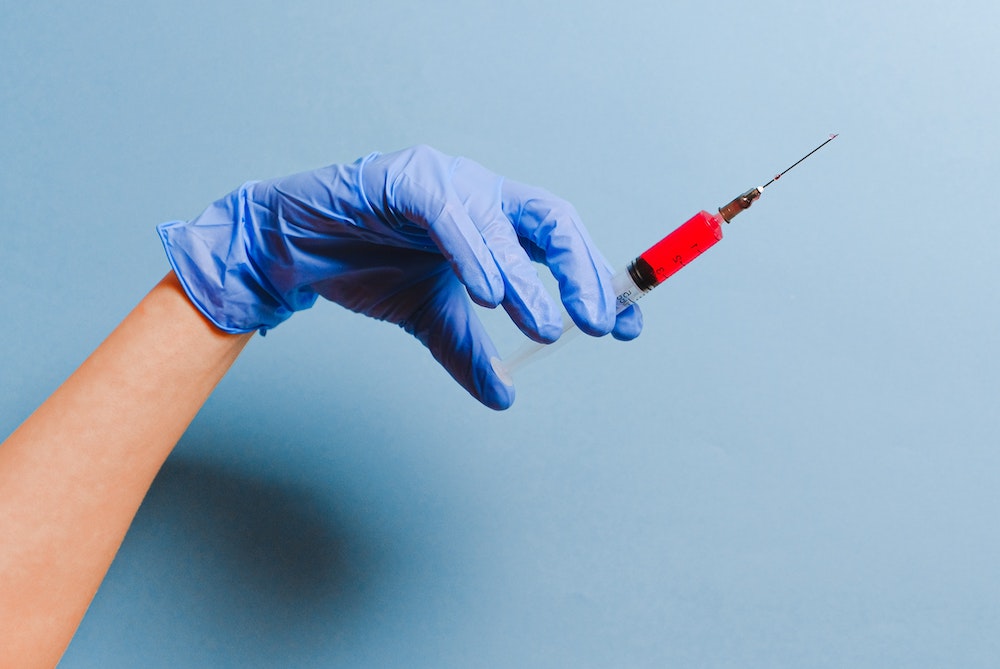
Should Educators Allow Nursing Simulation Students to Practice with Needles At Home?
While some nursing simulation centers and sim labs are working on reopening their facilities, many still remain closed. With the California State School system recently announcing that campus-based classes would not be returning in the Fall, the hard realities of the COVID-19 pandemic are still becoming clear this summer. Today Dr. Kim Baily PhD, MSN, RN, CNE, previous Simulation Coordinator for Los Angeles Harbor College and Director of Nursing for El Camino College, considers whether nursing simulation students should be able to practice needle sticks at home outside of the simulation labs.
While some fundamental nursing skills may be practiced at home safely, should nursing students be allowed to take home needles, syringes and glass vials to practice parenteral medication administration? After all, nursing students have reached a certain level of education and knowledge. Cannot faculty reasonably assume that students are responsible and careful enough to secure their equipment and take adequate precautions if they are allowed to practice at home?
In the regular clinical setting, needle stick injuries (NSI) and injuries from opening ampoules or vials are still a cause for concern. Smith and Leggat (2005) reported that 38 out of 273 nursing students reported a needle stick or sharps injury during the previous 12 months. Regarding prior usage, 81.6% of all injuring items were unused, 15.8% had been used on a patient and the status of 2.6% was unknown.
Sponsored Content:
Most needlestick injuries occurred either in the nursing laboratory (45%) or the teaching hospital (37%). Opening the needle cap was the most common causative event (28% of all cases). A total of 39.5% of needlestick injuries were not reported. The main reason for non-reporting was that the item was unused (42%) (Smith, D. & Leggat, P. (2005). Needlestick and Sharps Injuries Among Nursing Students. J Adv Nurs. Sep;51(5):449-55). Allowing nursing students to take home potentially hazardous equipment involves a risk versus benefit situation. Some considerations include the below:
Current College Policy for On-Campus Injury
Although lab injuries are relatively rare they do occur. What is your college policy for on-campus injury versus during clinical experiences? What if anything, is covered under the college insurance policy? Some institutions will delineate between injury related to an instructional experience and those considered employment related injuries. Such instructional experiences are not likely to be covered by Worker’s Compensation policies. Who will pay for any medical treatment needed?
Most colleges offer some kind of student health insurance. Check to see if the insurance will cover skills lab injuries at school and at home. Can a student wave the school’s healthcare policy if they provide their own healthcare insurance? If so, would the student’s own health insurance policy cover a lab injury? Note that if a student seeks assistance at a clinic not approved by the college under the college healthcare plan, the student will most likely be liable for all costs.
Sponsored Content:
Injury Reporting Form
All needle sticks or lacerations should be reported to a supervisor (skills lab supervisor) and when appropriate be referred to a healthcare professional for evaluation. Your college should have a standard reporting form to record any injury and any follow up from the injury. Usually there is a time frame for the completion of this form. Students should be current with tetanus vaccinations but if not, they may need a tetanus shot. Follow up visits are not likely to be needed but on the rare occurrence that an infection sets in antibiotics might be needed or if the wound is deep, stitches may be required.
This type of injury may often be dealt with at a college health center, providing the facility is open, or at a local health center which is connected to the college. This may seem overkill for a simple needle stick or cut from a broken vial however every college will have policies governing student injury which must be followed. If needles and other potentially sharp equipment are to be taken home by nursing students, the nursing department will need to speak to the administration to determine if the college health policy will cover any “at home” injuries.
Nursing Department Policy Development (See Below)
The college nursing department will need to write specific policies related to the use of sharps at home and in the event of an injury, who the student should report to and where should they go if they need medical attention? Nursing students would be required to sign a policy (possibly placed in a handbook) that they will be solely responsible for the needles safe keeping and the student has a plan for the safe disposal of needles or follows guidelines in a protocol for disposal. Students unable to confirm that they have a safe place to store needles should be excused from participating.
Theft or Use of Equipment By A Person Other Than The Nursing Student
On a rare chance that someone other than the nursing student steals or plays with the needles, who would be liable if any injury occurs? Will it be the student for failing to secure the needles/sharps, or the college for allowing students to take the equipment home in the first place? Would a student malpractice insurance cover such an incident? The author spoke with a representative from a large malpractice company and they were doubtful whether their insurance would cover any injury in this circumstance. Malpractice insurance is designed to cover a patient’s claim against a student who the patient believes suffered an adverse event related to a student’s nursing care. Each claim is reviewed separately. The malpractice insurance agent could not speculate about a hypothetical case, although they thought it unlikely that the company would consider paying a claim.
State Boards of Nursing
Does your State Board of Nursing have any regulations regarding skills practice at home that involves sharps?
Policy Development
If after a consideration of college liability and potential risks, the college administration and nursing faculty decide to proceed with allowing nursing students to take home needles and sharps, the following consideration should be considered:
- A specific policy should be created which governs the use of take home equipment which every nursing student would be required to sign. The policy could be part of a general handbook which includes multiple policies or a separate document which then becomes part of the student’s record.
- The policy should include a statement to the effect that the nursing student will be solely responsible for the needles/sharps safe keeping.
- There is an identified plan for the storage and disposal of all sharps. This may include purchase or provision of a small sharps container and a plan for disposal of the container.
- All equipment should be listed and accounted for at the end of the skills experience. Unused equipment should be returned to the college.
- Students unable to confirm that they have a safe place to store needles or practice with the needles uninterrupted should be excused from participating.
- In the event of an injury, the student would be required to complete a standard college injury reporting form within a set time frame (e.g. within 24 hours). Information should be provided on how to access this form and where it should be sent once it is completed (often the Academic Affairs Office). Specific contact information should be included.
- The policy should include a statement that practice is strictly limited to injection pads or other non animate devices. Absolutely no injections into self, family members or other individuals are permitted. The family pet is also excluded!
- Information regarding who the student should report to and where they should go if they need medical attention?
- Requirements for reporting stolen supplies.
- Define consequences for not following policy.
- Time frame for completion of skills practice and return of unused, unopened equipment and disposal of sharps containers.
- A statement to the effect that under no circumstances can home experiences with parenteral medication administration be counted as completion of parenteral medication administration checkoff.
- Release of liability by the college if a student injury occurs.
From the college risk department, the answer to an inquiry about students taking needles home, is likely to be an emphatic “No”! This may be very frustrating to faculty who have the best interests of their students at heart and students who only want to practice their skills however, in this litigious society, the lawyers usually have the last say!
Additional Reading: Needlestick and Sharps Injuries Among Nursing Students (Smith et al.): This paper reports the first investigation of the prevalence and nature of needlestick injuries among Australian nursing students. Needlestick and sharps injuries are the most efficient method of transmitting blood-borne pathogens between patients and healthcare staff. Although nurses are known to be a high-risk subgroup for these events, nursing students may be at even greater risk due to their limited clinical experience. Despite this fact, the epidemiology of needlestick and sharps injuries among nursing students has not been clearly elucidated in Australia.
From a group of 319 students, 274 successfully completed questionnaires were obtained (overall response rate 85.9%). A total of 38 students (13.9%) reported a needlestick or sharps injury during the previous 12 months. By causative item, 6.2% of students had been injured by a normal hollow-bore syringe needle, 3.6% by a glass item and 3.3% by an insulin syringe needle. Regarding prior usage, 81.6% of all injuring items were unused, 15.8% had been used on a patient and the status of 2.6% was unknown. Most needlestick injuries occurred either in the nursing laboratory (45%) or the teaching hospital (37%).
Although hepatitis B vaccination coverage among the students was excellent, it is important that the principles of infection-control training and reporting of all needlestick and sharps continue to be emphasized throughout undergraduate nursing education.
Subscribe to HealthySimulation.com’s Newsletter for More Great Sim Resources!
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Dr. Kim Baily, MSN, PhD, RN, CNE has had a passion for healthcare simulation since she pulled her first sim man out of the closet and into the light in 2002. She has been a full-time educator and director of nursing and was responsible for building and implementing two nursing simulation programs at El Camino College and Pasadena City College in Southern California. Dr. Baily is a member of both INACSL and SSH. She serves as a consultant for emerging clinical simulation programs and has previously chaired Southern California Simulation Collaborative, which supports healthcare professionals working in healthcare simulation in both hospitals and academic institutions throughout Southern California. Dr. Baily has taught a variety of nursing and medical simulation-related courses in a variety of forums, such as on-site simulation in healthcare debriefing workshops and online courses. Since retiring from full time teaching, she has written over 100 healthcare simulation educational articles for HealthySimulation.com while traveling around the country via her RV out of California.
Sponsored Content: