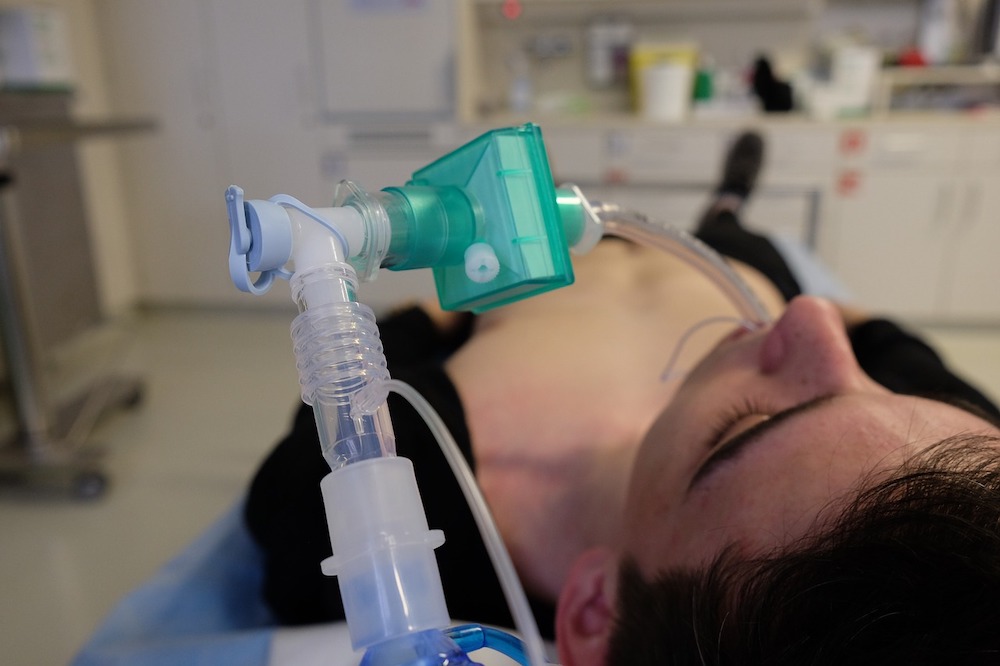
COVID-19 Ventilator Training Resources For Healthcare Simulation Programs
In the current COVID-19 pandemic, staff from general medical surgical floors may be relocated to intensive care areas where ventilators are commonplace. Today’s article, guest authored by Kim Baily PhD, MSN, RN, CNE, previous Simulation Coordinator for Los Angeles Harbor College and Director of Nursing for El Camino College, provides us ways that clinical simulation can be used to train for the use of mechanical ventilators. This post may be especially useful for simulation technicians following along with Dr. Baily’s “Physiology: The Force Behind Healthcare Simulation – A Guide for Techs” series, as it covers Ventilators from beyond a clinician-only perspective. As well, she provides us with links to downloadable resources on operating ventilators made available with appreciation from the Alameda Health Care Program.
Some healthcare professionals may have little experience operating ventilators. Healthcare simulation offers an obvious and effective strategy to train staff to manipulate ventilators and respond to alarms in a safe environment without potential harm to patients. Medical simulation will also allow the learner to familiarize themselves with the ventilator without having to worry about taking busy staff away from patients or the need to wear cumbersome PPE. Many newer human patient simulators, or manikins, can allow for ventilation training devices to be directly connected for high-fidelity simulation exercises, which could be of great benefit for healthcare professionals during the COVID19 pandemic.
Mechanical ventilation supports gas exchange which includes both alveolar ventilation and arterial oxygenation. The ventilator moves gas into the lungs while expiration remains passive. Ventilation assistance may be needed for a variety of reasons:
Sponsored Content:
- Anaesthesia during surgery
- Respiratory distress
- Failure of oxygenation with a PaO2 less than 60 mm HG and low or normal PaCO2 or ventilation where the ABG shows acidosis with a PaCO2 greater than 50 mmHg. (See Previous article on ABGs).
- Patients may be a candidate for noninvasive positive pressure ventilation (NIPPV) for example with an exacerbation of chronic obstructive pulmonary disease (COPD) or acute cardiogenic pulmonary edema).
- Altered mental status (head injury, drug overdose)
- Airway obstruction
- Apnea
- Ineffective clearance of secretions
- High risk aspiration
- Planned procedure short-term ventilation
Kati MaxKenzie from the Alameda Health Care program has generously offered to share the documents from their 90 minutes RN training program Care of the Patient receiving Mechanical Ventilation. The documents include a competency evaluation, detailed workshop agenda for care of the ventilator program, post class knowledge check, powerpoint presentation, and additional notes.
Ventilator Terms Relevant to Clinical Simulation:
- Rate (f): Number of ventilator-delivered breaths per minute: usually 12 to 15 in adults.Tidal Volume (Vt): Amount of gas delivered with each ventilator breath – usually 8 to 10 mL/Kg of body weight.
- Oxygen Concentration (FIO2). Percentage of oxygen delivered with ventilator breaths varies between 21% and 100%.
- I:E Ratio: Duration of inspiration to expiration usually 1:2 to 1:1.5
- Flow Rate: Speed at which air is delivered.
- Sensitivity: Effort required by patient to initiate a ventilator-assisted breath.
- Pressure Limit: Maximal pressure within airways that will terminate a ventilator breath.
- Compliance: Change in Volume/Change in Pressure. As lung compliance decreases, the same volume of gas will increase pressure and vice versa.
Types of Ventilators: There are two broad types of ventilators. Negative pressure ventilators create negative pressure externally to draw the chest outwards and air into the lungs (e.g. iron lung) and are mainly used to treat patients with neuromuscular disorders. Positive pressure ventilators, which are more commonly used, push air into the lungs via an endotracheal tube (ETT) or tracheostomy. Non-invasive positive pressure ventilation may be used in the form of nasal or face masks.
The basic settings of a ventilator include rate of flow, volume of gas, timing for ventilator cycles, pressure within the airways, pressure at the end of expiration and oxygen percentage. A trigger mechanism initiates the ventilator breath which can be initiated by the patient or the ventilator. At the end of inspiration, the ventilator cycles causing the breath to end and passive exhalation to occur. The limit of the cycle is reached if a set pressure or volume is reached.
Sponsored Content:
Modes: A number of different modes or patterns of ventilation may be used with positive pressure ventilators. The mode determines whether the breath is initiated by the patient or the ventilator and the pattern of airway support provided by the ventilator. Noninvasive ventilation (NIV) provides pressure support using a tight fitting face mask thus avoiding intubation. It’s primary use is to support patients with obstructive sleep apnea, neuromuscular disease, or impending respiratory failure. The degree of success varies, primarily limited to by patient intolerance due to the physical and psychologic discomfort of wearing a mask when dyspneic.
Spontaneous Breathing: Patient has full control of rate, tidal volumes and pressures.
Continuous Positive Airway Pressure (CPAP) applies positive pressure to the airways of a spontaneously breathing patient. CPAP may be used with either endotracheal intubation or a tight fitting face mask. All breathing is spontaneous and pressure controlled. CPAP is used to help maintain open airways and alveoli, decreasing the work of breathing. BiPAP ventilation provides inspiratory positive airway pressure as well as airway support during exhalation.
Continuous Mandatory Ventilation (CMV), or Assist Control: In continuous mandatory ventilation, the ventilator can be triggered either by the patient or mechanically by the ventilator. Patients can trigger a ventilator to deliver breaths at preset volume and inspiratory flow rate. Breaths will be delivered at preset rate if the patient does not initiate a breath (back up rate). For example if the preset rate is 14, and the patient breathes spontaneously above this rate, the ventilator will not add additional breaths.Typical volumes lie between 400-500 mL or 8mL per Kg ideal body weight.
Synchronized Intermittent Mandatory Ventilation (SIMV): Mandatory breaths delivered by ventilator are synchronized with the patient’s inspiratory effort. SIMV allows the patient to breathe spontaneously, without ventilator assistance, between delivered ventilator breaths. Mandatory or ventilator controlled breaths are delivered at a preset rate, volume, and/or pressure, coordinated with the patient’s inspiratory efforts. This mode of ventilation is used to support ventilation, to exercise respiratory muscles between the ventilator assisted breaths and during the weaning process.
Positive End-Expiratory Pressure (PEEP): Requires intubation and can be applied to any of the previously described ventilator modes. With PEEP, a positive pressure is maintained in the airways during exhalation and between breaths. Keeping alveoli open between breaths improves ventilation perfusion relationships and diffusion across the alveolar-capillary membrane. This reduces hypoxemia and allows use of lower percentages of inspired oxygen. PEEP is particularly useful for treating ARDS.
Pressure Support Ventilation(PSV): Pressurized inspiratory flow supports the patient’s inspiratory effort, decreasing the work of breathing. Ventilator assisted breaths are delivered when the patient initiates an inspiratory effort. This cycle is flow-limited; inspiration is terminated when inspiratory airflow falls below a preset rate. This mode decreases the work of breathing. It can be used in combination with SIMV when the respiratory drive is depressed. Ventilatory support can be gradually withdrawn during weaning.
Pressure-Control Ventilation (PCV) in contrast, controls pressure within the airways to reduce the risk of airway trauma. Ventilation is time triggered and time cycled, but pressure is limited. The ventilator maintains a preset airway pressure throughout inspiration. Because all breaths are controlled by the ventilator, heavier sedation may be required to prevent competition between inspiratory effort and ventilator control.
High Frequency Ventilation (HFV) provides small gas volumes delivered at a rapid rate. It is indicated in patients who are hemodynamically unstable and intolerant of conventional mechanical ventilation.
Complications: Although endotracheal intubation and mechanical ventilation can be life-saving in respiratory failure, they are not without risk. Improper endotracheal tube placement or advancement of the tube into a mainstem bronchus can result in ventilation of one lung only. The inflated lung becomes over distended and traumatized, and the uninflated lung develops atelectasis. In noninvasive ventilation, associated complications include gastric dilation, aspiration, facial skin necrosis, drying of the eyes and mucous membranes, stress and claustrophobia.
Nosocomial pneumonia infection is a significant risk associated with intubation and mechanical ventilation. Normal upper respiratory tract defense mechanisms are bypassed, with loss of air humidification and trapping of pathogens. Oral secretions and gastric contents can enter the respiratory tree through the open epiglottis. Frequent, meticulous oral hygiene is vital in preventing ventilator-associated pneumonia. Often the cough reflex is inhibited or impaired by the underlying disease process and the continued presence of the endotracheal tube. Even when strict asepsis is used for suctioning and other respiratory procedures, the lower airways are contaminated within 24 hours of incubation. Secretions often become thick and tenacious, increasing the risk of atelectasis.
Barotrauma is lung injury due to alveolar distention. Both the volume of delivered gas and the pressure under which it is delivered can contribute to barotrauma. As a result, over-distended alveoli rupture allowing air to escape into the pulmonary interstitial space and the mediastinum, pleural space and other tissues. Subcutaneous emphysema causes a crackling or bubbling sensation when the chest skin is palpated.
Cardiovascular effects: Positive pressure ventilation increases intrathoracic pressure, which can interfere with venous return to the heart and ventricular filling. As a result, cardiac output falls. Use of PEEP increases the effects of mechanical ventilation on cardiac output. The decreased cardiac output can affect liver and kidney function secondarily.
Gastrointestinal effects/complications are commonly associated with prolonged mechanical ventilation. Stress ulcers may develop leading to painless gastrointestinal hemorrhage.
Preventing ETT complications: Prevent skin breakdown around the tube and note location of ETT cm marking at the teeth, gums or nare. This will serve as a reference point when assessing whether the tube may have moved. Routinely assess for airway injury or displacement. Communicate with patients if they are awake with use of a communication board or by writing notes. If a patient is expected to need ventilation for a long period of time, there is obstruction of the upper airways or the patient has neuromuscular disease, a tracheostomy tube may be placed instead of an endotracheal tube (ET). Note: When first intubated, keep the patient on 100% oxygen until first ABG (usually at 30 minutes).
Staff caring for patients on ventilators must have a clear understanding of alarms. The Alameda Health Care program provides a competency test for care of the ventilated patient and appropriate response to alarms. Simulation in Healthcare provides an ideal method to help staff learn about ventilators, general care of patients on ventilators and responding to alarms.
Download the Alameda Health System Ventilator Refresher Resources Here!
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Dr. Kim Baily, MSN, PhD, RN, CNE has had a passion for healthcare simulation since she pulled her first sim man out of the closet and into the light in 2002. She has been a full-time educator and director of nursing and was responsible for building and implementing two nursing simulation programs at El Camino College and Pasadena City College in Southern California. Dr. Baily is a member of both INACSL and SSH. She serves as a consultant for emerging clinical simulation programs and has previously chaired Southern California Simulation Collaborative, which supports healthcare professionals working in healthcare simulation in both hospitals and academic institutions throughout Southern California. Dr. Baily has taught a variety of nursing and medical simulation-related courses in a variety of forums, such as on-site simulation in healthcare debriefing workshops and online courses. Since retiring from full time teaching, she has written over 100 healthcare simulation educational articles for HealthySimulation.com while traveling around the country via her RV out of California.
Sponsored Content: