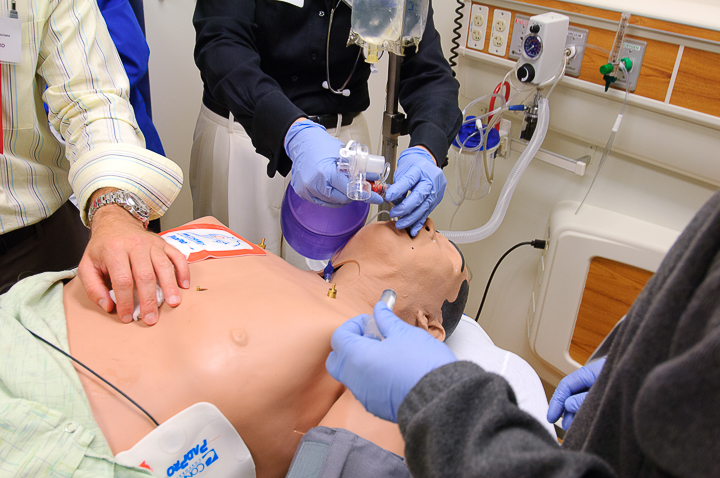
Types of Healthcare Simulation: Locations and Training – Who, What, and Where?
The latest Healthcare Simulation Book from the Springer Published Series has been published — and its all about operations! “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice“, provides a focus on the implementation of healthcare simulation operations, as well as the type of professional staff required for developing effective programs in this field. Chapter 2, by Jesika S. Gavilanes and Elena An, asks the “Who, What, and Where” of different “Types of Healthcare Simulation”, which we share excerpts of today. Please note, there are even more examples of how various professions utilize clinical simulation in the book.
Prehospital: Emergency Medical Services (EMS) and Other First Responders
Prehospital learners commonly practice skills training focusing on emergency stabilization of airway, breathing, and circulation. Simulation training may be con- ducted in a classroom, a simulation room, or in the field. EMT, paramedic, police, and fire and rescue personnel work individually as well as in groups for specific simulation trainings. Paramedic courses may include anatomy lab training that is directly applicable to their procedure training. Often, these trainings will be done in situ which includes training on the side of the road and integrating moulage to create a more immersive experience. Mobile simulation lab spaces have been added inside of functional ambulances with specialty cameras and recording devices to allow review and evaluation of learners as well as systems to control manikins on board. For example, EMS educator Penni Eggers Paramedic, M.Ed, CHSE, Doctoral student, Instructional Designer, EMS Educator, and Certified Healthcare Simulation Educator regularly utilizes high-fidelity manikins and simulation lab training spaces to “create specific formative assessments that include family centered care, full patient assessments, medication administration, crew resource management, and critical thinking.”
Sponsored Content:
While the implementation of medical simulation-based training uses multiple modalities, in situ training using field exercises is the most applicable to this group. This can be everything from practicing lifts and carries for firefighters performing a rescue, to police drills with active shooter scenarios and incorporation of curricula for tourniquet training and campaigns like “Stop the Bleed,” or working in lowlight conditions to evaluate a patient to provide stabilization and evaluation of a victim on the side of the road.
Nursing School Simulations
Nursing training focuses on management and coordination of care through patient assessment and procedural skills and patient care interventions. One of the most critical aspects of this role includes medication administration and monitoring. Nursing school at the undergraduate level has integrated skills training, high- fidelity manikin training, and often hybrid training with both standardized patients and manikins. There is strong literature that has come from nursing describing the debriefing components of simulation training and best practices for integration into curricula.
Skills training using task trainers is a common method to provide hands-on training to students prior to entering the clinical environment. This allows learners to demonstrate and educators to assess the evaluation and care for lines, tubes, IVs, surgical wounds, and examination skills. In addition to focused skills training, simulation centers have reproduced the look and feel of hospital wards, clinics, and intensive care units (ICUs) to allow familiarization with workflow, system processes, and equipment such as headwall systems, patient call requests, “code blue” activations, and medication dispensing units such as Pyxis and Omnicell that are ubiquitous in clinical practice.
Sponsored Content:
APN students integrate skills throughout their curriculum and have integrated Objective Structured Clinical Examinations (OSCEs) as well as the previously mentioned training for their initial nursing degrees.
Medical Simulation in Medical Schools
As the learners move toward preclinical experiences in their first and second years, there is an increase in use of simulation to build on fundamental medical education. These simulations include high-fidelity manikin scenarios and hybrid training opportunities. Some of these simulation experiences are of even greater need during the first 2 years of training as other clinical exposure is often limited. The carefully constructed ability to apply book knowledge to clinical cases is invaluable as a training and educational tool.
During the third and fourth years of medical school, exposure to patients truly begins and rotations through the primary specialties of medicine round out the educational experience. These core specialties include Pediatrics, Internal Medicine, Surgery, Family Medicine, Neurology, Obstetrics and Gynecology, and Psychiatry. Medical schools utilize integrated skills training and use simulation training with the OSCE and Clinical Performance Examination (CPX) with standardized patients. In order to complete medical school, three separate licensing examinations must be completed and passed. One of these is a high-stakes OSCE-based clinical skills test.
Additional Disciplines Covered in the Chapter
Other sections in Chapter 2 include breakdowns of the use of Clinical Simulation in Physician Assistant (PA) School, Pharmacy School, Graduate Medical Education, Professional Healthcare Teams, Military Simulations, Allied Health groups, and for the lay public.
More Key Take Aways From Latest Sim Ops Book Include:
- Practical guide helps prepare professionals for the broad scope of simulation in healthcare
- Defines the domains of medical simulation operations
- Focuses on the development of the healthcare simulation technology specialist
- Written and edited by leaders in the field of clinical simulation
Written and edited by leaders in the field, Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice is optimized for a variety of learners, including healthcare educators, simulation directors, as well as those looking to pursue a career in simulation operations as healthcare simulation technology specialists. Grab your copy today!
Get The Soft Cover Here!
Download the eBook Version Now!
Or Get from Amazon!
Lance Baily, BA, EMT-B, is the Founder / CEO of HealthySimulation.com, which he started in 2010 while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas. Lance also founded SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife live with their two brilliant daughters and one crazy dachshund in Las Vegas, Nevada.
Sponsored Content: