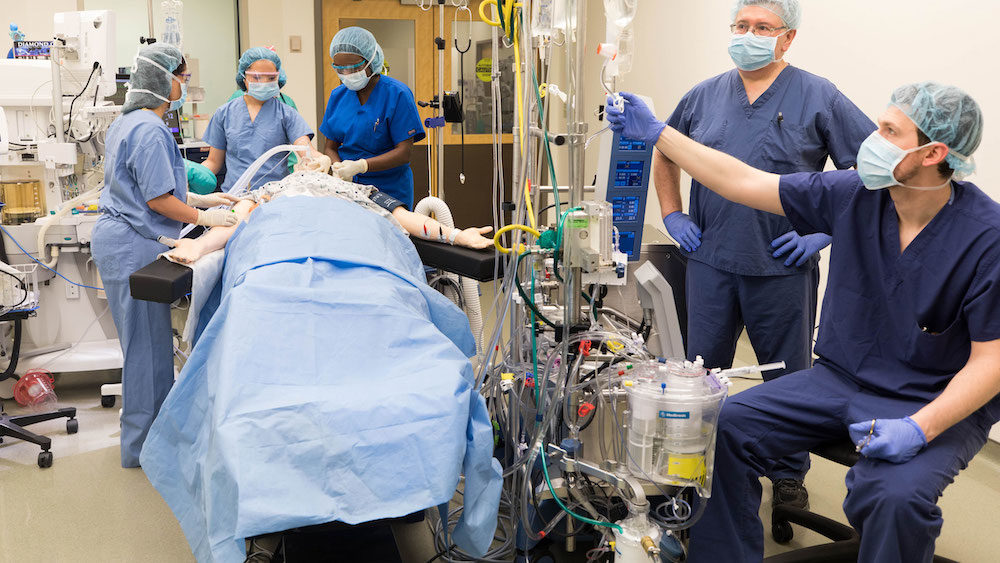
How to Develop a Successful Large Scale IPE Simulation Event
While developing Interprofessional Education (IPE) can present a series of unique challenges, developing a large scale IPE training event be down right overwhelming. Today’s article, guest authored by Matthew Charnetski, MSMS, NRP, Director of Simulation Learning at NYIT at Arkansas State University and Adjunct Faculty at Drexel University, provides a closer look at what it takes to develop large scale IPE events by providing experienced advice on the matter.
Interprofessional Education (IPE) has become increasingly recognized as an essential component of both high-quality healthcare and as a component of even early stages of education in many healthcare education programs. Depending on one’s curriculum and the availability of other professional groups in close proximity, it can be difficult to offer engaging, valuable, and efficient IPE activities. Engaging two or more distinct professions in a meaningful way can be simulated on a small scale remarkably well. Nearly every healthcare team functions inter-professionally. However, healthcare education programs often have large volumes of learners at different levels of education. Moreover, these volumes of learners typically need to all have similar experiences and meet the same outcomes, goals, and objectives.
Enter Large Scale IPE events. An organization can either increase the number of individuals involved in an event or extend the amount of time involved. With so many other demands on learners’ time, the only option is often to increase the number of learners that participate at one time. How does one avoid just checking the box of delivering an IPE activity and, instead, engage the learners in a meaningful simulated activity? Read on for tips to create a meaningful and smooth operating IPE activity.
Sponsored Content:
1. Start Early
Everyone has had the experience of being given short notice to put together some element of their curriculum. While many educators perform sometimes herculean feats to deliver high quality programming in remarkably short periods of time; Large Scale IPE is not the place for this.
At least six months out it is essential to start pulling together the personnel and lining out the logistics for a large-scale IPE healthcare simulation event. Everyone involved in nearly every stage of this will be incredibly busy and have competing priorities. Starting early allows for time to put the pieces together and for buffering to accommodate all of the other priorities that everyone involved already has.
2. Expert Modeling
Sponsored Content:
The best way to ensure a quality experience for every profession involved is to practice the elements that are espoused in IPE during the planning process. As one engages in the process of putting this together, consider the following elements of IPE:
- Understanding Teams and Teamwork
- Defining Roles and Responsibilities
- Effective Task Distribution and Close Loop Communication
- Elements of regular and urgent communication
- Navigating conflict and negotiating priorities
- Leadership and followership
If one engages these elements in the planning process the same elements are more likely to show through to the participants. Both in the activity and in their observations of the faculty and leadership.
3. Stakeholders At The Table Early and Often
One of the most common issues encountered in creating any multi-professional event is getting all of the interested parties to the table and keeping them there throughout the process. The only way to ensure that each professional is adequately represented and has the opportunity to engage and be part of the activity is if the activity is planned under the watchful eye of a representative of their profession.
Additionally, the individual that has been tapped as the stakeholder and representative in planning this event needs to have a familiarity with the practice of the profession, the surrounding curriculum, and some decision-making authority. With the right individuals at the table, the event has a significantly greater chance of success. With the right individuals consistently engaged at the same table, the opportunity for success increases exponentially.
4. Learning Outcomes, Goals, and Objectives Objectives Objectives
This cannot be stressed enough. Begin with the end in mind. Be specific. In the first meeting, outline the learning outcomes for the event. What kind of learner needs to exit this experience? The stakeholders at these early meetings then need to be prepared to come up with goals that support these learning outcomes that relate to each of their specific profession. Then, as planning continues, objectives can be created for each profession to reflect the activities the learners will engage in in order to achieve the goals and, ultimately, learning outcomes that have been created.
For instance, if the learning outcome is “create empathetic professionals that are capable of therapeutic communication with patients and other professionals.” Then each engaged profession would come up with a goal that is specific to their professional to support this. A supporting goal for paramedics might be to “communicate with patient, family, and other healthcare professionals related to an urgent medical situation.” Subsequently, the objectives for this would then be “Obtain informed consent from the patient to perform a physical examination of the patient,” “Describe patient condition and next steps to family that is present,” and “provide a concise and complete patient care report to the receiving nurse that also engages patient input.”
5. Choose Wisely
Once the Outcomes, Goals, and Objectives have been chosen; it is vital to consider what methodology is best to give the learners the opportunity to achieve the objectives. Are the objectives largely humanistic? Perhaps an experience with a standardized patient is best. Are their specific skills that need to be performed? Task trainers and/or manikins will be essential. Just as importantly, how will this experience be designed to fit within any time bounds with the volume of learners who are present?
If choices are not made to specifically and efficiently meet the expressed need, the experience can quickly grow out of control or feel contrived to the learner. This is the opportunity to consider how to get where one wants to end up. This is also the time to revisit those outcomes, goals, and objectives in case the aspirations of the team were too lofty for the time or volume of learners who are present.
6. Think Globally, Act Locally
While the ultimate goal is for an interprofessional experience, each of the stakeholders needs to consider their respective professions needs and advocate for them. Throughout the design of outcomes, goals and objectives, and in the selection of activities; each of the stakeholders needs to actively advocate for their learners. Medical Simulation provides the opportunity to design the activity to meet the needs of everyone present. If information needs to be added to the case to give a specific group of learners what they need, add it! If a specific context doesn’t work for a learner group, negotiate with the other stakeholders to find a context that will work for all of the learners who are present.
7. Professional Presence Start to Finish
Stakeholder presence has been key in several steps of this process. Truly, having faculty and/or practicing professionals from each of the representative groups is essential to a quality IPE event. From planning to implementation to debriefing and follow up, the presence of these individuals can help to maintain the professional aspect of interprofessional education and can frequently add to the experience for both the learners within their profession as well as the learners from other professions. Furthermore, having practicing professionals present can assist in avoiding the inadvertent propagation of stereotypes about any single profession.
8. Debrief Small, Debrief Big
When discussing the experience and event as a whole, start small. Give each profession a chance to debrief amongst themselves. Provide some structure, but also allow the group to share with one another in a more comfortable space what they learned and what they thought. Then, make sure there is also an opportunity for the professions to come together and debrief as a whole. These shared experiences, both large and small group, will further spread and cement the take home points and observations of the everyone involved to create the richest possible experience for all.
Concluding, large scale IPE experiences can be daunting. And, if done poorly, can be contrived and act in opposition to the goals of an IPE program. Using the above considerations can substantially increase buy-in and the overall value of a Large Scale IPE experience for the learners, facilitators, and respective professions and programs involved.
Subscribe to HealthySim’s Free Newsletter Today for More Great Simulation Advice!
About the Author: Matthew Charnetski, MSMS, NRP, Director of Simulation Learning at NYIT at Arkansas State University and Adjunct Faculty at Drexel University. The last 20-ish years have been a strange whirlwind from Iowa to Antarctica, Kazakhstan to Arkansas of Wilderness and Critical Care Paramedicine, Information Technologies Support, and Healthcare Simulation Operations and Curriculum Design.
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Mr. Matt Charnetski PhD(c), MS, NRP, CHSOS, CHSE has been in and around healthcare for his entire life. Academically he started with a BA in Biology from Grinnell College, a Masters in Medical and Healthcare Simulation, and is currently a PhD candidate at Maastricht University in the Netherlands. Geographically, he spent most of his life in and around Iowa, punctuated by time spent in East Africa, Antarctica, wandering the earth, Kazakhstan, Arkansas and now landing in New Hampshire. Mr. Charnetski is currently the Director of Simulation Based Education and Research at Dartmouth Hitchcock Medical Center in Lebanon, NH. Prior to this, Mr. Charnetski was the founding Director of Simulation and an Assistant Professor at Nazarbayev University in Nursultan Kazakhstan and the founding Director of Simulation Learning at NYIT – Arkansas in Jonesboro, AR. Professionally, Mr. Charnetski ha had a winding path through Logistics, Search and Rescue, IT, EMS, and various levels of Simulation to arrive at what he describes as “the best and strangest career I’ve ever had.” He is actively involved with SSH on the Internal Relations Committee and with INACSL in the review of some of the current standards of best practice. Mr. Charnetski also serves as Secretary of the Board of Directors of SimGHOSTS.
Sponsored Content: