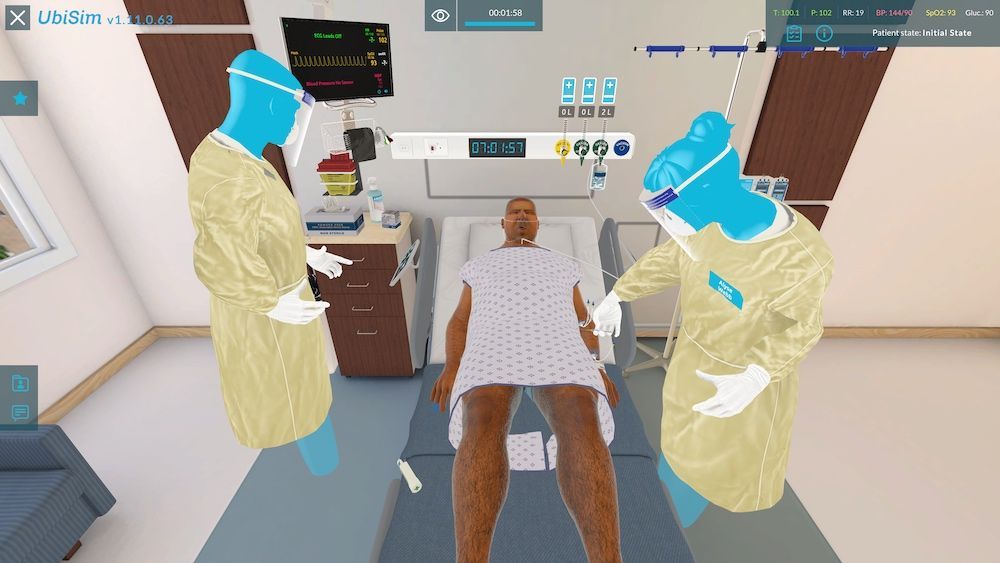
UbiSim Virtual Reality Prepares Nurse Learners for Next Gen NCLEX (NGN) Exam
UbiSim’s immersive Virtual Reality simulation is the new way to prepare prelicensure nursing students to build clinical judgment skills, pass the Next Gen NCLEX (NGN), and safely and effectively practice nursing. UbiSim also enables practicing nurses who are continuing their professional learning to sharpen their skills. The NGN radically changed from the previous nursing licensure exam in 2023. Next Gen NCLEX focuses on clinical judgment. The shortage of preceptors and quality clinical sites means the traditional way of teaching critical thinking and decision-making can no longer fill the gap between classroom theory and practice. Nursing students can go through their whole nursing program and not have opportunities to care for patients with certain critical and common diagnoses. UbiSim enables nurse educators to create and edit these scenarios from scratch themselves with no need to outsource customization to a developer. This HealthySimulation.com article will focus on how UbiSim’s immersive VR simulations prepare nurse learners to gain clinical judgment and excel on the Next Generation NCLEX.
Clinical Judgment Through Clinical Simulation
According to the INACSL Healthcare Simulation Standards of Best Practice, clinical judgment is “the art of making a series of decisions to determine whether to take action based on various types of knowledge. The individual recognizes changes and salient aspects in a clinical situation, interprets their meaning, responds appropriately, and reflects on the effectiveness of the intervention. Clinical judgment is influenced by the individual’s previous experiences, problem-solving, critical thinking, and clinical-reasoning abilities.” Simulation is highly effective for building competency, confidence, critical thinking, and readiness for practice. According to a blog by D’Errico (2022), the National Council of State Boards of Nursing (NCSBN), nurses are involved in 50% of patient errors, with 65% caused by poor clinical judgment. A recent study of 5,000 newly graduated nurses found that only 23% demonstrated adequate clinical judgment skills.
Sponsored Content:
“Simulation does help learners prepare for the NCLEX because it is that standardized patient and environment, the more they can practice through that whole nursing process: assessment, diagnose, intervene, and evaluate, it makes them increase their clinical judgment and be able to pass those questions on the test.” Amy Lee, Minot University, Nursing Department Chair and UbiSim user
National Council of State Boards of Nursing Clinical Judgment Measurement Model
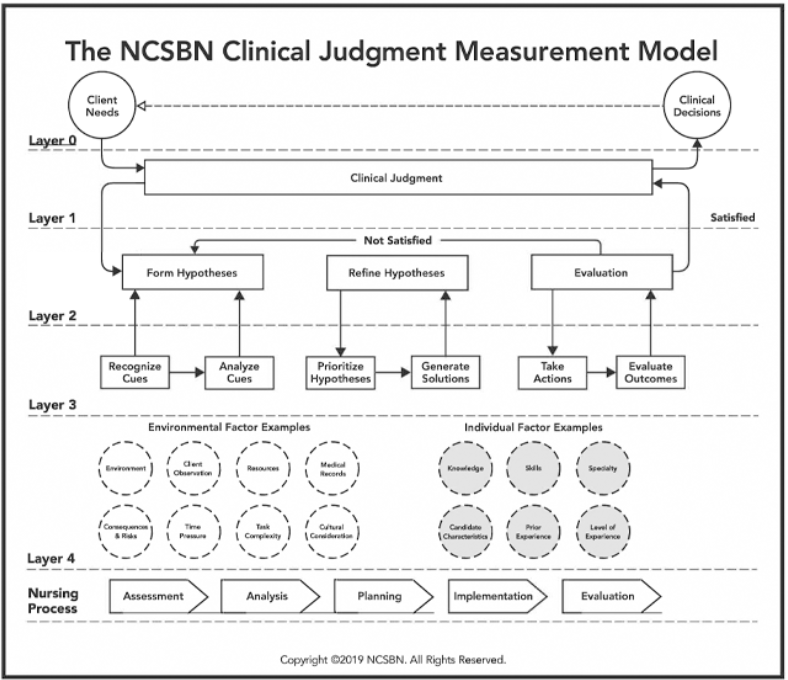
The NCSBN Clinical Judgment Measurement Model (NCJMM) is a framework for the valid measurement of clinical judgment and decision-making within the context of a standardized, high-stakes examination (see image). The NCJMM has contextual layers from 0 to 4.
- Layer 0 defines the context of the clinical situation.
- Layer 1 is the clinical judgment.
- Layer 2 is the conceptual elements required for clinical judgment, which forms and refines hypothesis and the evaluation of actions and outcomes.
- Layer 3 outlines the cognitive aspects of clinical decision-making that are directly measurable and are the basis for Next Generation NCLEX test items and case studies for the NCLEX exam. The six measurable are cognitive skills for appropriate clinical judgment: recognize cues, analyze cues, prioritize hypotheses, generate solutions, take action, and evaluate outcomes.
- Layer 4 provides examples of environment and individual factors as identified in the Nursing Clinical Decision-Making: A Literature Review.
- Retrieved from The NCSBN Clinical Judgment Measurement Model:
Sponsored Content:
UbiSim Prepares Learners for the Next Generation NCLEX
All UbiSim scenarios build upon the NCJMM. During the scenario design process, UbiSim nurse educators align the needs assessment with Layer 3 of the NCJMM to ensure learners can perform all steps of the clinical judgment process, from recognizing cues to evaluating outcomes. Educators can easily use the diverse library of pre-made valid and reliable scenarios or the web-based Editor to customize or create VR scenarios focused on clinical judgment. UbiSim also provides a realistic context for learners to develop clinical judgment skills. Time constraints, risks, and consequences affect the decision-making process; these realistic elements are present throughout the scenarios.
UbiSim scenarios help learners practice and build clinical judgment. The six steps of clinical judgment allow nursing students to recognize and analyze cues, prioritize hypotheses, generate solutions, take actions, and evaluate outcomes. Review the NCJMM diagram.
Recognize Cues
UbiSim scenarios incorporate cues for the nurse to recognize to manage client care. UbiSim includes an interactive EHR, an authentic bedside monitor displaying vital signs in real-time, and a variety of realistic subjective and objective assessment findings.
Analyze Cues
The next step is for learners to analyze the recognized cues and link them to the client’s clinical presentation. Learners identify if the relevant cues signify improving or worsening the client’s condition.
Prioritize Hypotheses
A set of cues can be present in a variety of client problems. When prioritizing hypotheses, UbiSim learners identify the most likely and critical explanations. Real-time prioritization guides the development of the client’s plan of care. A sense of urgency is created as vital signs change, family members ask questions, physical assessment findings evolve, and lab results become available. Prioritization under these dynamic conditions prepares learners for the Next Generation NCLEX and actual nursing practice.
Generate Solutions
In UbiSim, learners are challenged to encounter a virtual patient who has a complex health concern that requires them to generate solutions and identify priority interventions.
Nurse learners generate solutions by identifying actions to achieve a desirable client outcome.
Take Action
UbiSim challenges learners to take actions that address the highest client priorities. Learners decide how each action will be accomplished within the immersive VR scenario. This includes reading the EHR, performing physical assessments, and providing therapeutic communication in the learner’s own words, which mirrors the real-life clinical setting.
Evaluate Outcomes
Learners can evaluate outcomes and determine if their actions were effective. They can reassess the client, ask about subjective findings, or review lab and imaging results. Learners compare observations against expected outcomes to determine if the client is improving or declining. They can also determine if more interventions are needed to address the client’s needs. Events happen in real-time, allowing learners to continuously evaluate the outcome of their nursing actions, just like in a real-life clinical setting.
Debriefings
UbiSim provides a comprehensive, simulation-based experience that extends beyond the scenario itself. Facilitation beyond the scenario meets the INACSL Healthcare Simulation Standard of Best Practice Facilitation. After learners complete a session, they receive an automated feedback report specific to their performance. This report includes evidence-based, constructive feedback that aligns with the NCJMM.
During the debriefing, learners answer guided reflection questions based on the PEARLS framework. Reflecting on their experience, learners imagine how these lessons can be applied beyond the scenario and identify key takeaways to improve their practice moving forward.
View the HealthySimulation.com LEARN CE/CME Platform Webinar Beyond the Simulation Lab: Designing Immersive Virtual Reality Simulations to learn more!
Unfolding Case Studies
UbiSim scenarios feature unfolding case studies as a post-simulation activity. These cases expand upon the scenario, providing vignettes of the client’s situation at a future time. Unfolding case studies foster the development of clinical judgment with various Next Generation NCLEX question types, including matrix multiple response and multiple choice. The Editor empowers educators to customize or create their case studies easily.
UbiSim provides a safe and immersive environment where learners practice each measurable step of the clinical judgment process. In addition, UbiSim’s robust debriefing and case study capabilities reinforce and expand the learning that occurs within the VR scenario itself. These qualities give educators a powerful, fully-customizable platform that prepares learners to excel on the Next Generation NCLEX.
Jill Van Der Like, DNP, MSN, RNC, Director, Nursing Skills & Simulation Laboratory and Clinical Assistant Professor, University of West Florida School of Nursing: “We’re growing at warp speed. Our second-quarter pass rates were 100%. As for UbiSim, I’ve really been enjoying the post-simulation quizzes. Students have a rich discussion, and it’s a powerful way to process the concepts for NCLEX.”
More About UbiSim
UbiSim is a multidisciplinary team of nursing educators, healthcare simulation experts, software engineers, and 3D artists, working to combine nursing simulation and virtual reality for an immersive learning experience. The company aims to make nursing simulation more affordable, more accessible, and more realistic than ever.
Founded in 2016, UbiSim’s solution combines intuitive interactions provided by VR, flexible modules, and immediate feedback after each clinical simulation session. Dedicated to the nursing industry, UbiSim works exclusively on nursing simulation and immersive, interactive virtual reality solutions. This focus has allowed the company to build a platform that best responds to the unique needs of nursing educators and learners.
Learn More About UbiSim and Virtual Reality!
Teresa Gore, PhD, DNP, APRN, FNP-BC, CHSE-A, FSSH, FAAN – Dr. Gore has experience in educating future nurses in the undergraduate and graduate nursing programs. Dr. Gore has a PhD in Adult Education, a DNP as a family nurse practitioner, and a certificate in Simulation Education. Dr. Gore is an innovative, compassionate educator and an expert in the field of healthcare simulation. In 2007l Teresa started her journey in healthcare simulation. She is involved in INACSL and SSH. She is a Past-President of INACSL and is a Certified Healthcare Simulation Educator Advanced (CHSE-A). In 2018, she was inducted as a Fellow in the American Academy of Nursing (FAAN). In 2021, she was inducted as a Fellow in the Society of Simulation in Healthcare Academy (FSSH) and selected as a Visionary Leader University of Alabama at Birmingham School of Nursing Alumni. During her career, Dr. Gore has led in the development and integration of simulation into all undergraduate clinical courses and started an OSCE program for APRN students. Her research interests and scholarly work focus on simulation, online course development and faculty development. She has numerous invited presentations nationally and internationally on simulation topics.
Sponsored Content: