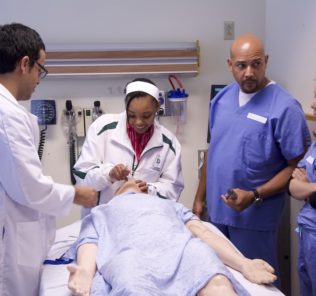
Columbia Nursing Hosts First Annual Innovations in Simulation Summit
In October 14th, healthcare simulation specialists from around the world met at Columbia Nursing’s first annual Innovations in Simulation Summit to exchange and discuss best practices in the field of clinical simulation education, examining its future, its research trends, and how it is and could be used to improve patient safety. Participants gathered from around the world, representing a range of nursing and medical disciplines, including deans, directors of simulation centers, those with deep knowledge of curricula, and prolific researchers. “This interprofessional summit is like a brain trust of simulation,” said Columbia Nursing’s Stephen Ferrara, DNP, assistant professor and associate dean of clinical affairs, in his opening remarks. “Every one of you has helped advance the frontiers of healthcare simulation, which continues to enhance how we train future and current practitioners to provide the best care.” Thanks to Kellie Bryant DNP, WHNP, CHSE, Executive Director of Simulation and Assistant Professor at Columbia University School of Nursing who shared today’s article covering the recent event!
Simulation is the use of human patient simulators (or manikins), actors portraying patients, or augmented/virtual reality modalities to mimic situations students or clinicians may encounter in delivering healthcare. The goals of simulation in healthcare are to give students and healthcare professionals opportunities to practice skills without risking harm to patients and to hone their ability to think critically on their feet. The summit and its participants were, in part, convened to take stock of how and to what degree these goals are being achieved. Participants were grouped into three panels by topic: the future of simulation-based education, latest trends in nursing simulation research, and patient safety outcomes. In each panel, four or five experts, along with a moderator, presented. Each panel also concluded with a Q&A session, where panelists fielded questions from the other participants.
Moderators included: Pamela R. Jeffries, PhD, professor and dean, George Washington University School of Nursing, for the panel on the future of simulation-based education; Michelle L. Aebersold, PhD, clinical associate professor and director of simulation and education innovation, University of Michigan School of Nursing, for the panel on the latest trends in simulation research; and Suzan (Suzie) Kardong- Edgren, PhD, professor and director of the RISE Center, School of Nursing and Health Sciences at Robert Morris University, Drexel University College of Medicine, for the panel on patient safety.
Sponsored Content:
Participants agreed that simulation has gone beyond its original purpose of just teaching basic skills to nursing and medical students. They observed that simulation is now used in healthcare systems as part of staff development, entailing scenarios designed to promote skills maintenance, harm reduction, and better staff integration.
Although simulation aims to prepare students, at any level, for the real world clinical setting, participants also noted differences between the learning environment and the actual workplace. For example, the typical simulation scenario involves one manikin or actor and several students. The opposite ratio occurs in the clinical setting, where a healthcare professional interacts with multiple patients at any time. In addition, panelists remarked that simulations may not be as interprofessional as they could be. Nurses may train exclusively with other nurses and physicians may train exclusively with other physicians, creating silos that extend into clinical practice.
“Often, it’s not until our first job as practitioners that we are put in an environment where we, as either nurses or physicians, need to work together,” said Kellie Bryant, DNP, executive director of simulation and assistant professor. “Yet, by establishing better interprofessional collaborations, we can work to eliminate silos, learning about each other, learning with each other, and learning from each other. Thus, simulation is key to achieving this integration and driving healthcare learning and practice into a space where we are operating from shared knowledge.”
Sponsored Content:
A highlight of the summit was a tour of Columbia Nursing’s Helene Fuld Health Trust Simulation Center. Opened in the autumn of 2017, the center consists of multiple rooms on two floors of the school. Leading the tour, Bryant pointed out a simulated labor and delivery suite, an operating room, and beds equipped as they would be in typical hospital rooms, with vital sign displays and electronic medical records. In one bed was a brand new pediatric manikin, and Bryant used a computer to make the simulated patient display emotions, such as being distraught and agitated, and their manifestations, such as shedding tears.
“Our state-of-the-art simulation center is where we use our knowledge as educators and experienced clinicians to create simulation activities that prepare our students to become the most competent healthcare professionals they can be,” said Bryant. “This summit allowed simulation experts from around the world to engage in thought provoking discussions on the future of simulation through gatherings of the kind we had today.”
As part of the Helene Fuld Health Trust Simulation Center grant, the Innovations in Simulation Summit will continue annually for the next four years. The outcomes of the first summit are being prepared for a journal manuscript submission. The manuscript will detail how simulation in healthcare has advanced over the years, including in research, in simulation-based education, and simulation’s impact on patient safety.
About the Helene Fuld Health Trust Sim Center
The Helene Fuld Health Trust Simulation Center at Columbia University School of Nursing is a two-story 16,000-square-foot state-of-the-art facility that enhances nursing education by simulating clinical practice using sophisticated technologies in a safe learning environment. It is one of the largest simulation centers dedicated to nursing simulation in New York State.
The simulation center is designed to promote patient safety and prepare students for real-world practice in an ever changing, complex healthcare system. It features authentically appointed patient examination rooms, two inpatient hospital rooms, a labor and delivery suite, and an operating room. Every room has been furnished with the equipment one would find in a clinical setting––blood pressure cuffs, thermometers, otoscopes, ophthalmoscopes, oxygen supplies, nitrile gloves, and monitors––for assessing and tracking patients’ health status. All have a sink for hand-washing, and a laptop computer for maintaining electronic medical records (EMRs). And each room has the latest audiovisual technology for recording students in action, providing a source of instructor feedback.
The simulation center features an array of task trainers and manikins––from low fidelity to high fidelity. A technician operates the computer that makes the high-fidelity manikins breathe, gasp for air, speak, blink, and respond to medication. Standardized Patients, trained actors that play the role of patient, are also used to enhance learning.
Visit the Columbia Nursing Helen Fuld Health Trust Simulation Center Website for More!
Lance Baily, BA, EMT-B, is the Founder / CEO of HealthySimulation.com, which he started in 2010 while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas. Lance also founded SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife live with their two brilliant daughters and one crazy dachshund in Las Vegas, Nevada.
Sponsored Content: