The Emergence of Virtual Clinical Simulation Helps Nursing Students Develop Judgement
Next-gen simulation can seriously help nursing students develop clinical judgement, specifically through the emergence of Virtual Clinical simulation. When high-fidelity, or manikin-based, simulation was first introduced as a complement to clinical instruction in the 1960s, nurse and medical educators finally found a scalable way to give students clinical interactions in a “safe environment” before seeing real patients.
Imagine the first time a nursing student realized their first experience of putting in a Foley catheter could be performed on a manikin instead of a real patient! In the next few decades manikin-based simulation grew in popularity, but some of its limitations also became evident.
The expense to equip and staff a sim lab put a strain on limited budgets and the growing desire of internet-generation students to learn outside the classroom/sim lab augured a need for new types of simulation tools. In the last decade, virtual clinical simulation has grown in popularity by providing a flexible simulation tool with an emphasis on the cognitive tasks involved in building clinical judgement and serving as a lower cost, flexible complement to high-fidelity manikin-based simulation as well as traditional clinical instruction.
Sponsored Content:
A Little History of Trends
If you are reading this, odds are you know some of the history of clinical simulation in healthcare, or at least that for your chosen field. Prior to the emergence of Resuscitation Annie1, the first realistic CPR training aid, clinical training was done solely with clinical instructors and live patients. Resuscitation Annie was the progenitor of computer-based manikin simulators introduced in the 1970s and 1980s such as The Harvey Cardiology manikin and Dr. David Gaba’s CASE (Comprehensive Anesthesia Simulation Environment) anesthesia simulator.2
In the 2000s, as the nursing shortage grew and the number of students in nursing school exploded, it became more difficult for nursing schools to find enough clinical placements; thus simulation became an increasingly important tool for nursing schools.
In the last decade, virtual clinical simulation has seen rapid growth, providing a flexible, lower cost tool for nursing students to practice their clinical judgment. Manikin-based simulation has increasingly become a way for nursing students to do psychomotor-based clinical training while virtual simulation is taking over the cognitive side of clinical education.
Sponsored Content:
Simulated Clinical Client Encounters for Nursing Students
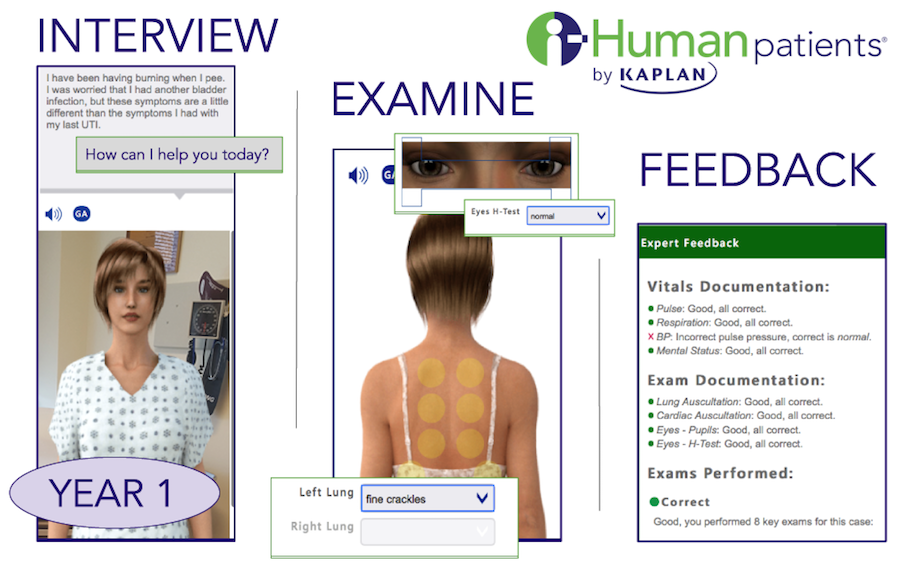
For today’s nursing schools, clinical “cognitive task” education has become an area of interest and need, for both graduate and undergraduate nursing students. “Virtual” client encounter simulations allow nursing students to hone their critical thinking and/or diagnostic reasoning skills prior to working with real clients. The value of this approach has been studied with positive results. How to therapeutically communicate with a client, read and interpret a medical health record, and prioritize issues are critical cognitive skills that can benefit from the latest digital virtual client encounter simulations for all levels of nursing education. Cognitive task simulation education has advanced dramatically since the “taking paper cases online” days a decade ago. Educators in 2018 are the beneficiaries of more recent advancements which now include lifelike client avatars, high resolution medical images, actual physiological sounds/audio, and detailed, realistic responses to the nurse, or other healthcare providers’ questions.
For undergraduate nursing students virtual simulation tools, such as i-Human Patients, can now include a more complete and immersive client encounter. These can include history-taking and recognizing and analyzing cues followed by prioritizing hypotheses, taking action and evaluating actions. For graduate-level nursing students, new virtual clinical simulation can include history taking and physical exam, building and ranking differential diagnoses, responding to feedback on differential diagnoses, ordering tests, and diagnosing.

As technology has improved, the level of client detail that virtual clinical simulation tools like i-Human Patients now exhibit can create an increasingly lifelike experience. i-Human Patients offers consistent feedback to students, allowing them to do simulation work independently, saving time for busy faculty while keeping students engaged.
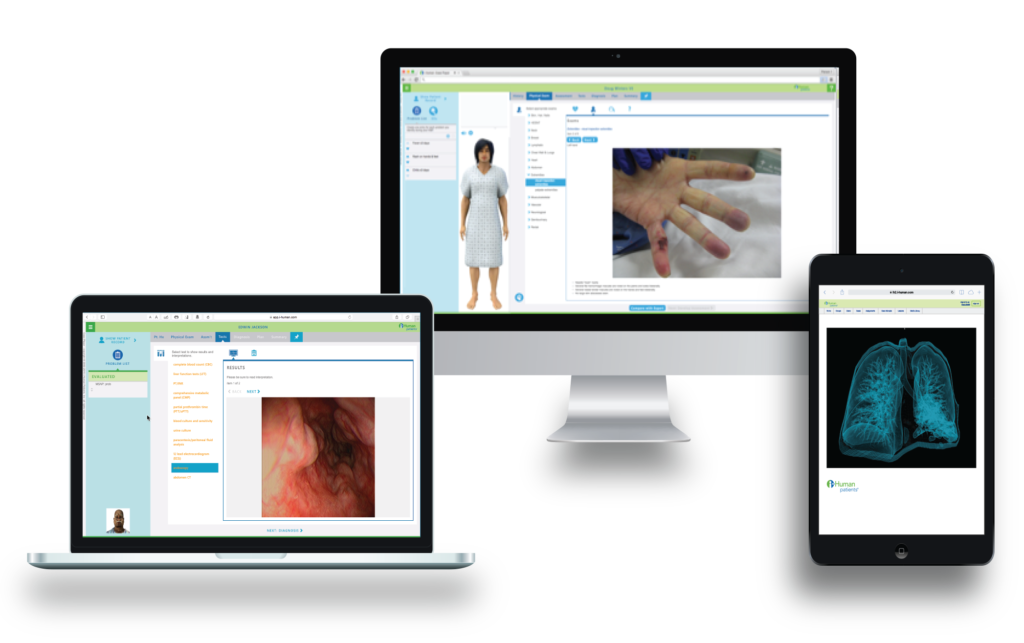
For faculty, i-Human Patients is also an assessment and analytics tool; providing objective, consistent assessment of students’ clinical judgement, and providing individual and cohort-level data to assess performance and competence levels.
Cognitive vs. Psychomotor Clinical Simulation: A Choice?
Manikin-based simulation is still the gold standard for psychomotor-based simulated learning. Many faculty and administrators employing simulation labs have also come to appreciate that psychomotor simulation is also most impactful when students have mastered the cognitive tasks first.
Use of cognitive virtual client simulations will efficiently help your students to learn how to:
- Perform client medical health record/chart review
- Communicate efficiently with client and family members
- Complete client assessment
- Identify client problems
- Prioritize hypotheses
- Select appropriate nursing actions
- Evaluate client outcomes
Nurse educators will continue to use manikin-simulators, standardized clients, and clinical faculty, but perhaps on a more limited basis at least partially because students will be more cognitively prepared for those encounters.
Used in conjunction, the latest in cognitive and psychomotor simulation assists in the development of competency and confidence in the nursing student by exposing them to different client encounters. Thus they will be better prepared when they interact with live clients, which is the desired outcome for you and your students.
Learn more about Virtual Clinical Simulations With a Webinar About i-Human Patients From Kaplan!
- Resuscitation Annie: https://www.cprconsultants.com/the-history-of-resuscitation-annie/
- A brief history of the development of mannequin simulators for clinical education and training, J B Cooper, V R Taqueti, BMJ Quality and Safety, https://qualitysafety.bmj.com/content/13/suppl_1/i11
- Validating the Use of High-Fidelity Simulation as a Clinical Adjunct in Undergraduate Nursing Education, Headstream-Pehl S. and Kunce-Collins, D, Journal of Healthcare Communications ISSN 2472-1654 2017 Vol. 2 No. 3: 24, http://healthcare-communications.imedpub.com/validating-the-use-of-highfidelity-simulation-as-a-clinical-adjunct-in-undergraduate-nursing-education.pdf
Lance Baily, BA, EMT-B, is the Founder / CEO of HealthySimulation.com, which he started in 2010 while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas. Lance also founded SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife live with their two brilliant daughters and one crazy dachshund in Las Vegas, Nevada.
Sponsored Content: