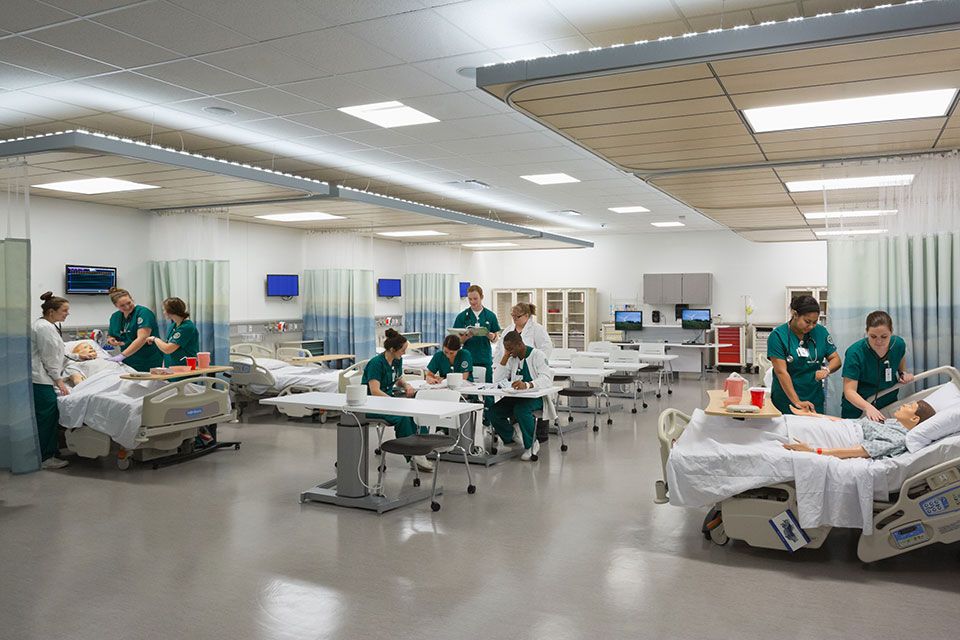
9 Key Considerations When Designing a Sim Lab
Designing a simulation lab is a multi-step process that involves extensive planning. Following a needs assessment, the learning requirements and characteristics of the learners are identified and measurable objectives are written. These objectives will dictate the type of healthcare simulation needed as well as indicate the type of equipment and space requirements to meet the program goals. Below guest author Dr. Kim Baily PhD, MSN, RN, CNE, covers the first 9 of 20 key considerations that might prove useful for planning a nursing or medical simulation laboratory!
1. Stakeholders: Include all stakeholders in planning meetings. Failure to include facilities or IT departments can lead to installation problems later down the line. The type of equipment and operating system will determine whether the simulation lab network will be independent or hooked into the main institution’s network. Network access and security issues need to be decided before building begins.
2. Storage, storage, storage: Imagine all the equipment and electronics needed to operate a simulation lab including but not limited to, a family of manikins with their monitors, computers for electronic health record access, medication carts, IV poles, isolation carts, resuscitation carts, beds, furniture, and general supplies such as linens, dressings, IV bags and medication administration devices etc. etc. Not all equipment will be used for every simulation, therefore, adequate storage is essential. Storing unwanted manikins on chairs around the room frequently leads to damage particularly to the neck of the manikin. Garage shelving creates a safe storage space where manikins may be positioned horizontally. Providing enough storage will ensure that there is adequate clutter free space for simulation.
Sponsored Content:
3. Manikins: High fidelity manikins have many features but can be very expensive. Each program should determine which manikin best fit the program goals. For example, does an associate degree nursing program really need an expensive OB manikin or would this type of program be better served by purchasing a less expensive low or mid fidelity manikin.
4. Water/Sinks/Infection Control. Ideally water should be available in both simulation rooms and preparation spaces however, plumbing installations will add considerably to construction costs. Sinks in the simulation prep room are necessary for prop preparation such as IV fluids, blood bags, body fluids and simply for cleaning. For Infection Control, a decision is needed to determine if simulation participants will use hand gel or hand washing in sinks. Portable sinks are available but remember someone will have to routinely fill the clean water reservoir as well as empty the waste water. Failure to maintain portable sinks leads to stagnant water accumulation.
5. Compressors: Most modern manikins have compressors within the manikin but a separate external compressor might be needed to create simulated gases and/or vacuums. Since compressors tend to be noisy, they should be located in a separate room if possible. Note that the length of connecting hoses may be limited depending on the compressor. Some facilities put compressors on the roof and pipe in gases into the simulation labs.
6. Gases: Room air to simulate oxygen supply or create vacuums may be sufficient for most labs, however, anaesthesiology and respiratory technician programs may require oxygen for their specialized equipment to function properly. Running oxygen into labs involves another set of safety standards. Portable tanks may be used but they will need to be stored, secured and replaced when empty.
Sponsored Content:
7. Headwalls: Actual or simulated head walls help provided fidelity. Some headwalls have compressors/motors within the headwall housing. These headwalls have functioning gas valves which mimic oxygen and air valves found in hospital headwalls. They can also generate a vacuum/suction. Some educational headwalls have internal compressors while others have external compressors both of which can be noisy. Headwalls may be attached to the wall or be portable.
8. Gurneys: Gurneys are very useful for moving manikins around however, the gurneys will need a storage place when not in use. Simulation manikins are often heavy and due consideration should be given to the staff who have to move them. Slider boards are helpful when moving manikins from bed to gurney to storage.
9. Door width: Hospital beds and other large pieces of equipment will not fit through a typical single door so plan on double doors or extra wide doors that will accommodate large pieces of equipment.
Healthcare simulation educators and administrators involved in building a simulation lab should tour local simulation facilities and consider joining regional simulation groups to explore options. Vendors can assist with planning and installation but costs can quickly rise especially if extensive audiovisual and computerized systems are being installed. However, healthcare simulation does not have to be elaborate. A simplified lab with low or mid-fidelity manikins and basic supplies can work well. Several companies make an in situ recording system that fits in a briefcase and for some programs, this may be the way to start. Since the benefits of simulation education are well documented, now might be the right time to create a simulation lab.
Consider that there is a LOT that can go wrong with designing a simulation lab space, and to maximize ROI, simulation programs should consider hiring an outside consultant who specializes in the field. Several A/V companies offer support with A/V systems design, and yet others offer turn-key solutions. Use our “Find Vendor” form linked below to connect with leading consultants now.
Complete Our Form to be Connected with Simulation Lab Consultants Now!
Today’s article was guest authored by Kim Baily PhD, MSN, RN, CNE, previous Simulation Coordinator for Los Angeles Harbor College and Director of Nursing for El Camino College. Over the past 16 years Kim has developed and implemented several college simulation programs and previously chaired the Southern California Simulation Collaborative.
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Dr. Kim Baily, MSN, PhD, RN, CNE has had a passion for healthcare simulation since she pulled her first sim man out of the closet and into the light in 2002. She has been a full-time educator and director of nursing and was responsible for building and implementing two nursing simulation programs at El Camino College and Pasadena City College in Southern California. Dr. Baily is a member of both INACSL and SSH. She serves as a consultant for emerging clinical simulation programs and has previously chaired Southern California Simulation Collaborative, which supports healthcare professionals working in healthcare simulation in both hospitals and academic institutions throughout Southern California. Dr. Baily has taught a variety of nursing and medical simulation-related courses in a variety of forums, such as on-site simulation in healthcare debriefing workshops and online courses. Since retiring from full time teaching, she has written over 100 healthcare simulation educational articles for HealthySimulation.com while traveling around the country via her RV out of California.
Sponsored Content: