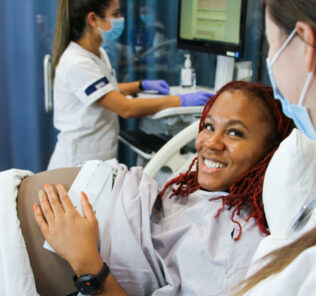
Helpful Thoughts on In Situ Simulation

Today a helpful list of advantages, disadvantages, safety issues and tips, success strategies, and evidence for In Situ Simulation by the blogging team at Life in the Fast Lane. Life in the Fast Lane is comprised of Australasian critical care physicians and nurses exploring the changing world of eLearning, emergency medicine, critical care and toxicology through clinical cases, fictionalized anecdotes and medical satire. Below is an excerpt of the list they created:
“Overview
Sponsored Content:
- In situ simulation is simulation that takes place in the actual working environment and involving those who work there
- As such, it is distinct from ‘center-based simulation’, which takes place in a separate simulation center
- In situ simulation may involve any simulation modality (e.g. mannikin-based, simulated patients, task trainers, hybrid simulations), be high or low fidelity, and may be scheduled or performed impromptu (will appropriate prebriefing)
Advantages
- enable learners to learn about the environment they work and the processes in place (e.g. location of airway trolley)
- learners are more comfortable in their own environment
- the environment is realistic (i.e. identical to reality)
- less detail needed for prebriefing regarding the environment as it is already familiar to learners
- easier and more accessible for busy participants, with minimal travel time
- an expensive dedicated facility is not required
- if families are appropriately informed they often feel more confident when they see staff practicing simulations
- free for participants
- can reveal local system errors and latent threats (e.g. location of difficult airway trolley)
- easy to tailor simulation to case mix and sentinel events that have occurred in the workplace
- can be used to introduce guidelines and protocols
- improve teamwork and inter-professional communication using teams that actually work together
- easy to follow up (e.g. re-run simulation until participants perform well)
- can have repeated scenarios that build upon one another (e.g. follow a ‘patient journey’ over time)
Ensuring Success of In Situ Simulation
- allow sufficient time
- tailor physical fidelity to the needs of the scenario to meet the learning objectives
- organise equipment to allow rapid set up and take down of scenarios
- ensure faculty are trained in simulation and debriefing
- obtain and develop unit-wide support and buy in (may require a change management process)
- ensure adequate prebrief (establishing ground rules and orientation to scenario and equipment)
- employ safety measures as above
- integrate with curriculum
- use unit-specific scenarios
- be flexible (e.g. may need to cancel when the unit is busy)
- evaluate programme
- integrate with quality improvement
- impromptu simulation must still have appropriate prebriefing of those involved (e.g. notification of code team that a simulated code will take place in the near future)”
More about Life in the Fast Lane:
Sponsored Content:
“Our team was born out of passionate (and usually unresolved) debate pertaining to the elements of eLearning; medical education; medical history; political ambiguity; information sharing, sacred secret truthfulness and the open source era and the ethos of web 2.0. We write simply to facilitate the learning process by providing diverse and hopefully entertaining reading material. Naturally we cite and give due reverence to the great hero of modern clinical medicine, Sir William Osler.”
Read the full In Situ Simulation List on the Life In the Fast Lane website!
Lance Baily, BA, EMT-B, is the Founder & CEO of HealthySimulation.com, which he started while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas back in 2010. Lance is also the Founder and acting Advisor to the Board of SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife Abigail Baily, PhD live in Las Vegas, Nevada with their two amazing daughters.
Sponsored Content: