Virtual Reality Application Advances ALS-Sim Training
Cardiac arrests present challenges that require medical practitioners and nurses to respond quickly and accurately to save the life of the patient. Advanced Cardiac Life Support refreshment training is required to ensure protocols and skills are kept up to date. Training health practitioners and nurses in Advanced Life Support (ALS) has always presented various challenges and the outbreak of coronavirus has made it very difficult to continue to facilitate training, propelling the development of medical virtual reality applications. Today, an ingenious ALS-Sim virtual reality (VR) application has been developed as a way to overcome logistical restrictions and social distancing requirements.
The significant advantage of using the ALS-Sim VR is that training can take place without the risks involved with conventional ALS training, both for patients and clinicians. This is especially relevant with the increased risk of contracting COVID-19 in conventional training. This is met with the need for the team to work closely together, making the practicing of social distancing nearly impossible. In addition to delivering ALS training anywhere and enabling ALS leaders to practice their skills for their annual reaccreditation; training with the ALS-Sim virtual reality application is also more cost-effective than traditional training methods.
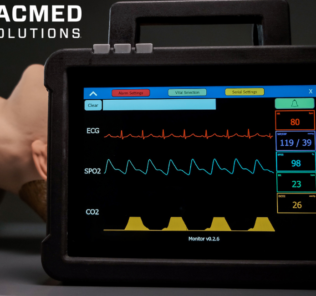
Randomization of the cardiac rhythm and recording of user performance against key KPIs allows the user to practice real-time interpretation of cardiac rhythms in the setting of a cardiac arrest. Common ALS medications are available for administration by the team, and the medication administration is graded against the ARC council guidelines depending on whether the patient is on the shockable or non-shockable side of the algorithm.
Sponsored Content:
An Exploratory Usability Study into the development of VR ALS training, analyzed how effectively specific clinician user needs are met when VR ALS is used for training. The study used Jakob Nielsen’s 10 general principles for heuristic evaluation of the interaction of clinicians with the application. The clinicians had a median age of 40.9 years; with experience delivering ALS training, and limited or no experience using VR applications.
This evaluation was then combined with interviews to find out how the clinicians rated the usability and potential use of ALS-Sim VR in both clinical and educational training. The study concluded that although there were areas that required further development, the ALS-Sim VR was rated highly by the clinicians who trialled it during a single play through for the study.
ALS-Sim VR Application in Practice
Martin Brown from the University of Sydney and Nathan Moore, educational innovation and technology lead for Western Sydney Local Health District, have worked together to develop the ALS-Sim VR application. Supported by the Research and Education Network, the University of Sydney provided the $40,000 funding for the prototype app to be developed and built by the company Frameless Interactive. Now that the ALS-Sim VR application is in the final stages of beta testing, it looks to be a viable way to provide additional training and refresher training in ALS.
Sponsored Content:
Currently, the ALS-Sim VR application is being incorporated into the annual accreditation process ALS leaders need to undertake, in a simulation lab at Westmead Hospital. All decisions made during the use of this immersive application are assessed according to the Australian Resuscitation Council Advanced Life Support courses’ guidelines. During ALS a team of four medical practitioners and/or nurses need to work together, led by the team leader. The ALS-Sim VR application allows the team leader to practice with their team virtually, to ensure they pass their annual accreditation. The Oculus-Quest headset makes it simple to use and works with a handheld control that is easy to use.
A custom-made game engine has been created to ensure the actions taken reflect the reality of a real patient having a cardiac arrest. In addition to enabling safe training to take place, Brown advocates another aspect of the ALS-Sim VR. He explains that this approach “makes it possible for the clinician to be presented with a different case in each practice session.” All decisions that could be realistically made by a clinician treating a patient have been considered and programmed into the game engine.
The application provides an immersive experience with:
- Randomization of the cardiac rhythm.
- Standard ALS medicines.
- Randomized arterial blood gasses.
- Three-dimensional models of either the X Series or R Series ZOLL defibrillator.
- Randomized ECGs.
- Randomized patient clinical handovers.
The clinician’s decisions can then be replayed and reviewed against key KPIs graded against the ARC council guidelines, and randomized arterial blood gasses. They can also be be replayed and reviewed against randomized ECGs.
This makes the ALS-Sim VR extremely reflective of any errors of judgment that could result in a negative patient outcome. Another advantage of using the ALS-Sim VR application is the functionality that allows for all sessions to be recorded. This allows staff to replay the session to analyze what they did correctly and any areas that they need to improve. This should help to increase the clinician’s confidence when under pressure, especially during the treatment of real patients. Consequently, improving patient safety and reducing clinician anxiety and the potential of burnout.
“We’re not just utilizing technology for the sake of technology, we’re looking to fill a real need in our training by giving people the opportunity to practice the skills they’d need in a real emergency,” Moore said.
The Future of ALS-Sim VR Application Training and Refresher Training
Moore is currently undertaking his PhD studies. He plans to assess the effectiveness of the ALS-Sim VR application with clinicians who will use the application, prior to their accreditation assessments. This will provide data into both the usability of the application and potential improvements that need to be made, to generate higher pass rates.
Moore states the application has not been designed to “replace the need for tactile, hands-on training, but it’s definitely a great way to supplement what already exists to help clinicians be better prepared to put their skills into practice.”
Learn more about the ALS-Sim VR application at Frameless Interactive.
Lance Baily, BA, EMT-B, is the Founder & CEO of HealthySimulation.com, which he started while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas back in 2010. Lance is also the Founder and acting Advisor to the Board of SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife Abigail Baily, PhD live in Las Vegas, Nevada with their two amazing daughters.
Sponsored Content: