Holistic Simulation: Mental and Physical Health in a Pandemic
“If I go to see someone about my eyes, my eyes are what I am, and the rest of me doesn’t matter. It’s the same with mental health. If I go to see someone for a mental health problem, I am a mental health problem,” said a mental health focus group participant discussing clinician approaches to consultation.1 If you work in healthcare, or if you’ve ever been a patient with multiple conditions, you may relate to the statement above. You may have been that clinician or that patient. Here, Oxford Medical Simulation Founder and Chief Medical Officer Jack Pottle, MD asks “Why is this? Why do we as healthcare professionals tend to see one issue at a time?” while considering the opportunity for a more holistic simulation approach to healthcare education and training.
One at a time
Part of it is the time pressures we are under – we need to prioritize and focus on the most urgent issue first. Part of it is about competence – the skills and confidence to work outside our conventional role boundaries. Part of it is about attitudes – there is a tendency to treat physical health ahead of mental health.
Sponsored Content:
And part, unfortunately, is our education. We are taught, in classes, in clinicals and in healthcare simulation, to think of issues as discrete. A mental health simulation involves a mental health issue, and cardiac scenario is about chest pain, and so on.
Yet we know in the real world people aren’t that simple. We know that mental and physical health are inextricably linked and it is detrimental to a person’s overall wellbeing to regard these as two separate entities. As such, shouldn’t we be designing simulation to teach just that? The team at Oxford Medical Simulation (OMS) think so…
Holistic Simulation
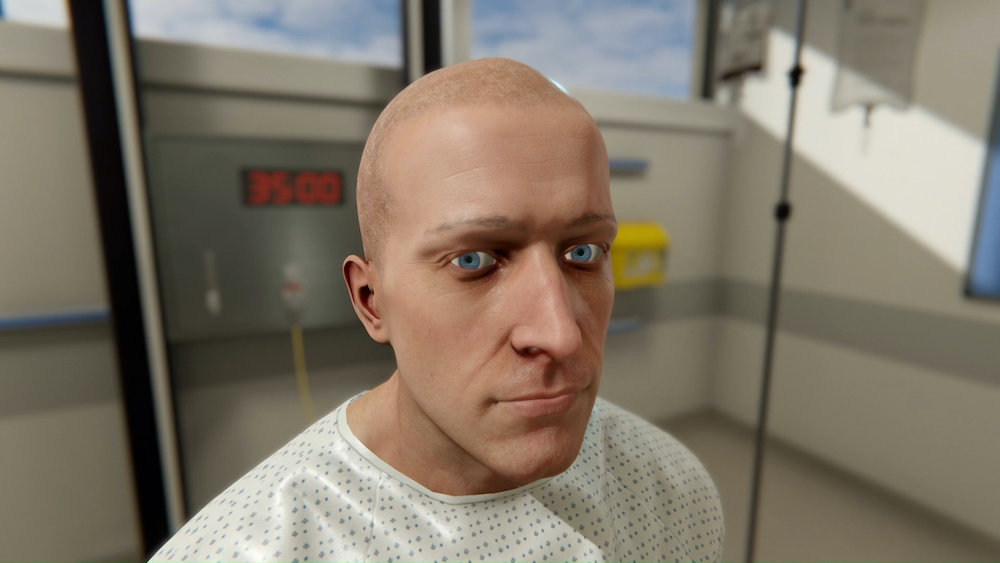
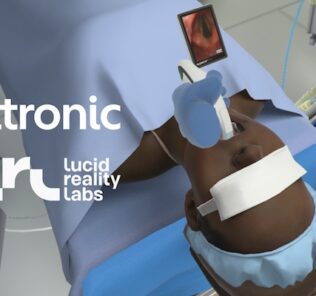
OMS delivers clinical experiences on-demand helping educators provide fully interactive and immersive simulation on screen and in virtual reality. The OMS virtual patients reflect what we see in the real world, taking a holistic approach to managing mental and physical health. Each scenario of the OMS mental health library has been created to help learners hone their skills in mental health assessment, and – as in real life – contain physical health issues as well.
Sponsored Content:
For example, Maria is an 80-year-old patient presenting with shortness of breath. Though she has a history of heart failure, her most prevalent issue is acute anxiety. The learner must balance these two issues to successfully manage Maria. This involves establishing rapport, elucidating a medical and mental health history, assessing acute anxiety, use of scoring systems, investigating coping mechanisms and sources of support, involving the relevant teams for further assessment, and documenting as needed.
As with all the OMS scenarios, all elements of care are possible: communication, examination, investigations, EMR, charting, and team interaction – just like in the real world. This breadth of possibilities, combined with adaptive scenarios that change depending on learner behaviors, ensures scenarios feel real, whilst scaffolded learning ensures they are appropriate for a wide range of learners.
The virtual patients are designed to look and behave like real patients, from low mood and poor eye contact, to confusion and agitation. All have been designed with input from relevant patient populations. After each scenario, detailed feedback, evidence-based blended learning and performance analytics allow the learner to repeat and improve their performance over time, and guided debrief allows them to reflect and document their performance.
Scenarios are objective and standardized and can run with or without faculty input. This allows instructors to focus on debriefing, synchronously or asynchronously, with OMS providing the clinical experience. Running on learners’ own computers, ensuring accessibility, or in virtual reality, for maximal immersion, OMS scenarios are built to deliver simulation at scale.
The mental health library contains a range of scenarios to cover the mental health syllabus. The growing OMS mental health library consists of scenarios that challenge learners across multiple areas: anxiety, self-harm, bulimia nervosa, alcohol dependence, chronic pain, dementia with difficult behavior, gender transition and suicidal ideation.
There is a lot to learn within each scenario. The OMS approach reflects the understanding that healthcare professionals don’t need to be experts in mental health to have a huge impact. Getting the basics right is the most important element in mental healthcare.1 Taking a “whole person” perspective, focusing on communication and consultation skills, ensuring coordination of care, and encouraging self-management and peer support are common across all scenarios.
The Context
Physical health problems significantly increase the risk of poor mental health, and vice versa. Around 30% of all people with a long-term physical health condition also have a mental health problem,2 and mental health problems can seriously exacerbate physical illness, affecting outcomes and the cost of treatment.3 This is compounded as many of those with diagnosable mental health problems receive no formal treatment. As such, a presentation for medical care may be the first presentation with an underlying mental health issue.4
To appreciate just how important and timely these issues are, prior to COVID-19, one in five U.S. adults lived with a mental health issue.5 In 2020 this skyrocketed. Nine months into the pandemic, 42% of people surveyed by the U.S. Census Bureau reported symptoms of anxiety or depression – an increase from 11% the previous year.
This is not surprising. Fear of contracting the virus, working from home, temporary unemployment, home-schooling, and lack of physical contact all contribute. “I don’t think this is going to go back to baseline anytime soon,” says clinical psychologist at Harvard Medical School in Boston, Massachusetts, Luana Marques, who is monitoring the mental-health impacts of the crisis.6
And amongst the mental health casualties are healthcare workers. It was known from the SARS outbreak that clinicians were at high risk of developing anxiety, depression, stress during outbreaks.7 Sadly, this has been reflected across the healthcare spectrum during COVID-19, with nurses seeming to be most impacted by the consequences of the pandemic.8 Without healthcare workers there is no healthcare system, so whilst we continue to strive to improve the care we provide our patients, we mustn’t forget about ourselves, and each other.
All this to say that as the urgency of the pandemic begins to recede, the focus will rightly turn to the mental health epidemic. We should be designing scenarios that reflect this. Blending learning objectives across mental health and physical health through simulation is one way to help us deliver the complex care required for our patients, and scenarios such as those designed by OMS are part of that picture.
Learn More About Oxford Medical Simulation
References:
-
- https://www.kingsfund.org.uk/sites/default/files/field/field_publication_file/Bringing-together-Kings-Fund-March-2016_1.pdf
- https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(12)60240-2/fulltext
- https://www.kingsfund.org.uk/sites/default/files/field/field_publication_file/long-term-conditions-mental-health-cost-comorbidities-naylor-feb12.pdf
- https://www.kingsfund.org.uk/projects/time-think-differently/trends-disease-and-disability-mental-physical-health
- https://www.nimh.nih.gov/health/statistics/mental-illness.shtml#part_154785
- https://www.nature.com/articles/d41586-021-00175-z
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7175897/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7314868/
Today’s article was guest authored by Jack Pottle, MD, Founder and Chief Medical Officer at Oxford Medical Simulation.
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Sponsored Content: