Patient Safety
According to the World Health Organization (WHO) Patient Safety “is the absence of preventable harm to a patient during the process of health care and reduction of risk of unnecessary harm associated with health care to an acceptable minimum.” Common healthcare errors include patients receiving the wrong medications, contracting hospital acquired infections, having the wrong body part removed during surgery, receiving an incorrect diagnosis or having a missed diagnosis or treatment.
Despite significant advances in patient care within the United States and around the world, the number of patients harmed while receiving health care is still unacceptably high. The WHO estimates that patient harm is the 14th leading cause of morbidity and mortality around the world. According to a recent John Hopkins study released in 2016, 250,000 patients die in the US each year from medical errors. Other estimates make the number higher. Medical errors are the third leading cause of death in the US following heart disease and cancer.
When comparing healthcare to other potentially lethal industries such as aviation or nuclear power generation, a huge difference in the likelihood of harm becomes evident. Both aviation and nuclear power are considered to be high reliability industries since on most days zero harm occurs. Jumbo jets do not crash everyday and as soon as a crash does occur, the crash is investigated and a cause identified. For many years in medicine, occasional errors were accepted as inevitable and were seldom reported, spoken about or investigated. In 1999 the Institute of Medicine published a report entitled To Err is Human: Building a Safer Health System. This report, which was the first significant attempt to quantify the number of errors, estimated that 98,000 people died annually from preventable causes in the US.
Sponsored Content:
Systems Approach to Preventing Errors
The IOM study spurred much research and change in the following twenty years and although many hospitals and other healthcare facilities have reported better patient outcomes, the number of preventable patient harm events is still high. The Swiss Cheese Model (Jim Reason) depicts errors as a series of layers of Swiss cheese with holes at different places. Usually an error does not progress through all the layers into a harmful event because one or other of the layers of cheese block the error. On rare occasions, the holes of the cheese all line up and the error or series of errors results in patient harm. A systems approach to preventing patient harm accepts that practitioners will on occasion make errors, however implementing a series of checks and warnings will prevent the error from progressing through all the layers and end up causing patient harm.
HealthySimulation.com is dedicated to providing the latest Patient Safety news and resources from around the world. To follow along, sign up for our free medical simulation email newsletter, follow @HealthySim on Twitter and @HealthySim on Facebook, or join our HealthySim LinkedIn Group!
For example, central lines (intravenous access to major blood vessels) are a source of infection. Many hospitals have created check off sheets based on current best practice which all staff must follow. The introduction of check off sheets and additional training has significantly reduced the incidence of central line infections in those hospitals that follow the guidelines.
Sponsored Content:
The use of barcode scanning for medication administration has made significant inroads in reducing medication administration error. Not all hospitals use barcode scanning and not all hospitals that have barcode scanning use the system 100% of the time. In these situations an initial error has no checks or blocks to prevent the error progressing to cause patient harm.
Reporting Errors
Previously healthcare practitioners who made mistakes would try to correct the mistake but would often not speak about or report the error for fear of reprisals. One study revealed that over 50% nurses are afraid of speaking up when near misses occur because of fear of disciplinary action. According to Peter Drucker, “you can’t manage what you can’t measure”. When the error or near miss occurs, it must be reported and investigated. A change in culture is occurring where staff are encouraged to report near misses and errors so that system changes can be made to prevent errors from happening again. Electronic health records can track where errors or near misses occur and can help identify where changes to the system or additional staff training is needed.
Zero Harm (Zero Preventable Deaths)
Many hospitals are adopting zero harm policies where errors are no longer listed as specific actions but rather that the number of times patients were treated safely e.g. 99% of patients with central lines did not develop infections. Hospitals are trying to put a human face on the error so it becomes meaningful to the staff. Departments track their own infection rates or fall rates and all members of the hospital staff are held responsible for patient safety (including non medical staff). Cultures of safety are growing within hospitals so that every patient is treated safely and zero harm results.
Healthcare simulation plays an increasing role in creating zero patient harm. In the past, healthcare practitioners often learned their skills on actual patients. Today, staff can practice repeatedly in various types of simulation exercises before they ever take a step inside a patient’s room or potentially cause patient harm. Teams can learn communication and other soft skills. New equipment and protocols can be investigated before being generally implemented.
Patient Safety Organizations
A sampling of national organizations involved in improving patient safety is listed below.
The Patient Safety Movement Foundation
Mission: Unify the healthcare ecosystem (hospitals, healthcare technology companies, government agencies, policy makers, patient advocates, clinicians, engineers, payers, etc.). Learn more about the PSMF here.
- Identify the challenges that are killing patients and create actionable solutions (Actionable Patient Safety Solutions) to mitigate them.
- Ask hospitals to implement Actionable Patient Safety Solutions (APSS).
- Ask healthcare technology companies to share the data their devices are purchased for in order to create a Patient
- Data Super Highway to help identify at-risk patients
- Promote transparency and aligned incentives
- Promote patient dignity & love
- Educate providers, health professionals in training, patients, and families about patient safety
In January 2019, the Foundation held its 7th Annual World Patient Safety, Science & Technology Summit and announced over 90,146 lives saved because of commitments made by over 4,710 partnered hospitals across 50 countries.
The Joint Commission
Mission: To continuously improve health care for the public, in collaboration with other stakeholders, by evaluating health care organizations and inspiring them to excel in providing safe and effective care of the highest quality and value. The Joint Commission are an independent, not-for-profit organization which accredits and certifies nearly 21,000 health care organizations and programs in the United States. Joint Commission accreditation and certification is recognized nationwide as a symbol of quality that reflects an organization’s commitment to meeting certain performance standards.
The Joint Commission is the nation’s oldest and largest standards-setting and accrediting body in health care.
Institute for Healthcare Improvement
For more than 25 years, the Institute for Healthcare Improvement (IHI) has used improvement science to advance and sustain better outcomes in health and health care across the world. Mission:
To bring awareness of safety and quality to millions, accelerate learning and the systematic improvement of care, develop solutions to previously intractable challenges, and mobilize health systems, communities, regions. Works in collaboration with the growing IHI community to spark bold, inventive ways to improve the health of individuals and populations. Generates optimism, harvest fresh ideas, and support anyone, anywhere who wants to profoundly change health and health care for the better.
Agency for Healthcare Research and Quality (AHRQ) Patient Safety Network (PSNet)
A national web-based resource featuring the latest news and essential resources on patient safety. The site offers weekly updates of patient safety literature, news, tools, and meetings (“Current Issue”), and a vast set of carefully annotated links to important research and other information on patient safety (“The Collection”). The AHRQ PSNet Collection comprises an extensive selection of resources relevant to the patient safety community. These resources come in a variety of formats, including literature, research, tools, and Web sites. Resources are identified using the National Library of Medicine’s Medline database, various news and content aggregators, and the expertise of the AHRQ PSNet editorial and technical teams.
The Leapfrog Hospital Safety Grade
The Leapfrog Hospital Safety Grade is a public service provided by The Leapfrog Group, a nonprofit organization committed to driving quality, safety, and transparency in the U.S. health system.
Mission: Saving lives by reducing errors, injuries, accidents, and infections, The Leapfrog Group focuses on measuring and publicly reporting hospital performance through the annual Leapfrog Hospital Survey. The survey is a trusted, transparent and evidence-based national tool in which nearly 2,000 hospitals voluntarily participate free of charge. The Leapfrog Group advocates for public access to quality and safety data from all U.S. hospitals.
Click Here to Connect to Leading Healthcare Simulation Vendors Who Improve Patient Safety
International Society for Quality in Healthcare Care (ISQua)
The International Society for Quality in Healthcare Care, or ISQua, is a member-based, not-for-profit community and organization dedicated to promoting quality improvement in health care, who have been working to improve the quality and safety of health care worldwide for over 30 years! Their extensive network of health care professionals spans over 70 countries and 6 continents all of whom share the goal of improving patient safety through education, knowledge sharing, external evaluation, supporting health systems worldwide and connecting like-minded people through their health care networks. Today we learn how ISQua and it’s members are continually working towards quality improvement in health care around the world.
Visit our Conference Listings Page to See Events from These Orgs and Others!
Pt Safety Latest News

Support U.S. House Bill HR 7591 to Establish A National Patient Safety Board

Global Healthcare Simulation News Update January 2024

Global State of Patient Safety: Annual Review

Reduce Medical Errors and Enhance Patient Safety Through Medical Simulation

Healthcare Simulation for Process Improvement

HealthStream’s New OB Safety SIMS Toolkit

Laerdal Medical’s One Million Lives Campaign 2023 Update
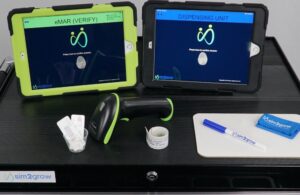
Customers Give High Marks to sim2grow’s Medication Administration System as a Game Changer for Improving Student Learning Outcomes

10 Commandments for the Medical Simulation Novice Debriefer

SimGHOSTS Shares Updates, Upcoming Conference Information

Latest Clinical Simulation News From Around the World | March 2023
Sponsored Content: