Kaiser Permanente Shares Success of New Sim Labs & TEAMSTEPPS Training at SoCal Sim Collaborative
Yesterday in Los Angeles the Southern California Simulation Collaborative came together at the newly upgraded Kaiser Permanante Los Angeles Medical Center Simulation Center for a half-day of tours, educational sessions and peer support networking. HealthySimulation.com writers were on hand to learn more about the new Simulation Labs, TEAMSTEPPS programs, and training successes at Kaiser.
Dr. Nilesh Patel, Assistant Area Medical Director of the Los Angeles Medical Center (LAMC), opened the event sharing about the goal of the sim center to optimize safety, improve quality of care, and enhance the patient experience by incorporating simulation-based training for their health care professionals and care delivery teams. He shared further that “the goal to have highly reliable teams is now closer to reality for [them], thanks to the new medical simulation space!”.
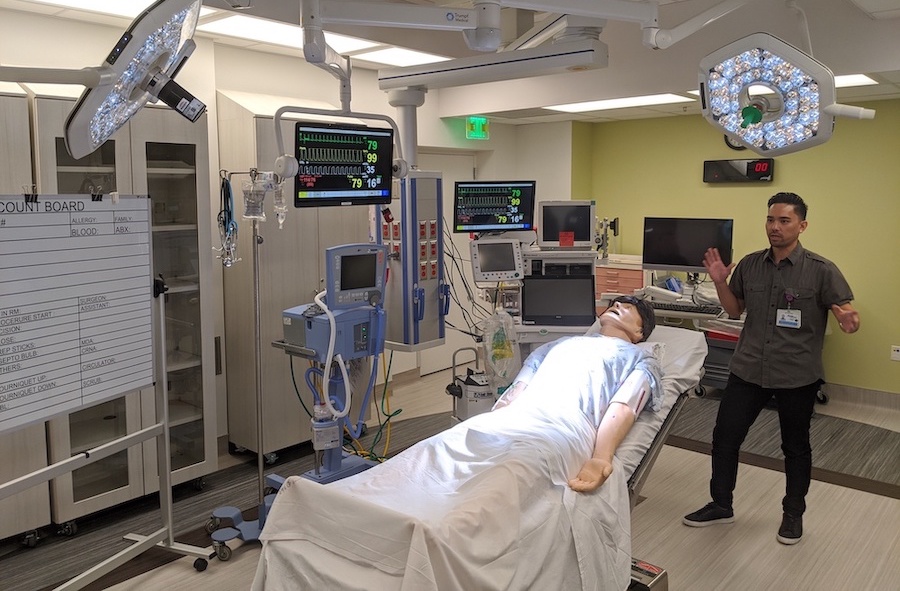
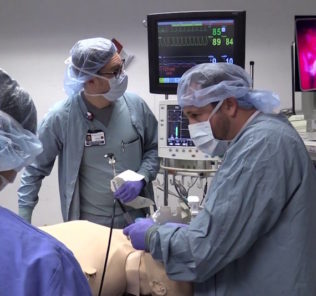
Simulation Technician and Coordinator Nathan Vidal helped to share the story of the expansion of the simulation spaces with Kaiser which opened a new Simulated Surgical OR labs in January of 2019. Sanjeet Gill, Simulation Program Manager, shared on the tour that they utilize CAE Learning Space for their A/V recording and debriefing system which can be streamed live to other Kaiser sites across California, but that they wired the sim labs to be able to utilize any manikin brand throughout the space, now or in the future, to maximize flexibility as technologies evolved.
Sponsored Content:
The Kaiser team shared that their primary learners are the 120+ medical residents at any time with new residents coming in regularly, but also the Nursing programs and Nursing student programs also heavily utilize the spaces. Sanjeet shared that by having clearly defined objectives for each learner group, rather than “haphazard” simulation experiences designed day of, has really helped to drive initiatives.
While each Kaiser Simulation Program is currently locally funded and managed, regional educational groups do utilize the LAMC Simulation Space for specialized training opportunities like RT or Pediatrics groups. The goal is to showcase the regional success stories of simulation centers like the one at LAMC to help grow the California state wide initiatives for expanding simulation.
More About the Kaiser Permanente LAMC Simulation Center
The LAMC Simulation Center now includes two simulation suites specifically designed for procedural skills training and team-based simulations, and the center is equipped with cameras and microphones to facilitate debriefing. The LAMC Simulation Center provides various courses for learners to develop the necessary skills for performing technical procedures.
Sponsored Content:
From the novice to seasoned learner, technical training provides an opportunity to develop procedural knowledge and psychomotor skills. Through repetitive practice on our task trainers and simulators, health care providers can develop muscle memory to conduct procedures, such as Lumbar Punctures, Venipuncture, and more. Technical training assists learners in recognizing areas for improvement that can be implemented their future practice and care delivery.
The LAMC Simulation Center also provides a safe and secure environment for the multidisciplinary team collaboration that is essential for the delivery of safe, highly reliable patient care of the highest quality. Their facility allows learners to practice managing critical events that require teamwork and effective communication, like TEAMSTEPPS which is shared about below. Practicing such skills in a controlled setting allows learners to learn from their mistakes without directly compromising patient care.
Additional Articles About KP’s Use of Simulation:
- Watch Over 50 Anesthesiology Simulation Training Videos From Kaiser Permanente School of Anesthesia
- New Kaiser Permanente School of Medicine and Simulation Center Coming Next Year
TeamSTEPPS: Clinical Performance & Safety Culture
Following the tour, Dr. Mark Lassoff, Assistant Chief of Service for the Department of Urology at LAMC, and Barbara Helliwell RN, Director of Patient Safety and Risk Management, provided a powerful presentation about the use of TEAMSTEPPS.
TeamSTEPPS (Team Strategies and Tools to Enhance Performance and Patient Safety) is an evidence-based framework to optimize team performance across the healthcare delivery system. The core of the TeamSTEPPS framework is comprised of four skills: Leadership, Situation Monitoring, Mutual Support, and Communication.
Barbara said to make TEAMSTEPPS work they needed first to “set the stage” for change by activating the leadership, followed by building stakeholder teams which included Physician Champions, Nurse Leaders, and Patient Safety Trainers. Barbara said a key component for success with this communication-based training was to have representatives of each disciplines be apart of the development of the program for peer-to-peer interactions for socialization of the tools.
Sharing their strategy, Barbara reflected that they trained the entire service line at one time, including all the key groups to ensure maximum engagement. By making the training relevant, memorable and fun while connecting TEAMSTEPPS to existing learning initiatives, Barbara and Mark were able to further connect to further connect the mental models to pre-existing goals. “Connect the content to the need”, Barbara reminded the group, sharing national and organizational data to support the use of TEAMSTEPPS when they were asked “Why?”.
In just three sessions over 3 days, the team was able to train 88% of the staff, remarking that to achieve that goal took a huge amount of time and energy from the programs to coordinate the schedule. Regarding outcomes, the program has been very successful with regards to reducing communication errors, improving outcomes, and winning safety awards!
Following this, Gaumard representative Michael Moyer shared about the features of the Super Tory infant simulator.
Suspending Disbelief: Using Simulation to Enhance Nursing Performance
Aaron Akamine, BSN RN and Denise Sherwood MHA/MSN, RN gave one of the afternoon presentations regarding the use of realistic clinical simulations at KP’s LAMC Sim Center. The covered a spectrum of simulation tools, pre-production and planning, scenario implementation, value of the facilitator debrief, and measuring program effectiveness.
They cited a 2013 meta-analysis of 14 studies which found that simulation-based learning helped improve clinician performance through developing leadership skills, solving complex problems and educating patients, all while reducing costs of care, complication rates and patient discomfort. Following this, they explained how different types of simulation and various ranges of simulator fidelities can best be used to empower educators to train for the specific procedures, skills and understanding.
About the Southern California Simulation Collaborative (SCSC)
Currently chaired by Russell D. Metcalfe-Smith of the Cedars-Sinai Women’s Guild Simulation Center, the SCSC was developed with leadership provided by CINHC, supported with initial funding from the Kaiser Permanente Community Benefit Grants Program in 2009. The SCSC built upon the learnings and success of the BASC funded by the Gordon and Betty Moore Foundation, and provides a regional mechanism to facilitate networking and support collaboration in the advancement of simulation practices in Los Angeles and the five surrounding county areas. The SCSC consists of several hundred service and academic simulation enthusiasts in the greater Los Angeles area and beyond.
The group includes clinicians, academics, sim op specialists and techs from the area. They typically meet quarterly at different sim centers throughout the region (February, May, September and November). They share research and best practices as well as offer support to one another. There are no dues or commitments to belong to the group other than an interest in simulation. They also have offered several local inexpensive debriefing workshops with funding from the Health Workforce Initiative.
Lance Baily, BA, EMT-B, is the Founder & CEO of HealthySimulation.com, which he started while serving as the Director of the Nevada System of Higher Education’s Clinical Simulation Center of Las Vegas back in 2010. Lance is also the Founder and acting Advisor to the Board of SimGHOSTS.org, the world’s only non-profit organization dedicated to supporting professionals operating healthcare simulation technologies. His co-edited Book: “Comprehensive Healthcare Simulation: Operations, Technology, and Innovative Practice” is cited as a key source for professional certification in the industry. Lance’s background also includes serving as a Simulation Technology Specialist for the LA Community College District, EMS fire fighting, Hollywood movie production, rescue diving, and global travel. He and his wife Abigail Baily, PhD live in Las Vegas, Nevada with their two amazing daughters.
Sponsored Content: