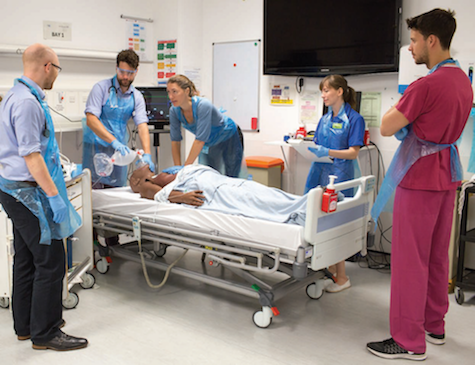
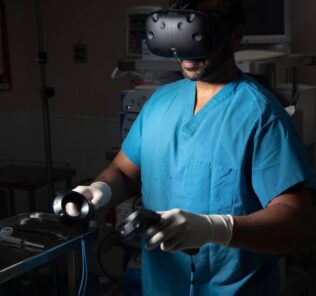
Healthcare Simulation Scenario Development Checklist w/ Downloadable Form
Healthcare simulation scenarios are designed to address specific learning needs. According to the International Nursing Association for Clinical Simulation and Learning (INACSL) the first step in scenario development is the completion of a needs assessment. The INACSL simulation design standard provides a sequential plan for scenario development which can be adapted for use in clinical facilities, medical schools and postgraduate medical education. Today, Dr. Kim Baily PhD, MSN, RN, CNE shares the key areas necessary for developing simulation scenarios and provides a downloadable template form!
Once the learning needs are identified and learning objectives created, scenarios are developed which will assist learners in meeting the learning objectives. All facets of simulation design should be included in a scenario development checklist such as determination of fidelity required, type of simulation, prebriefing and debriefing strategies, manikins and equipment needed, faculty/content expert review and pilot testing.
Needs Assessment: Formal: Chart reviews, critical events analysis (RCAs) e.g. falls, wound infections, late intubations or transfers to the ICU. Failure to meet EBP standards e.g. pediatric codes. Low exam scores. Informal: Reports from line managers regarding potential patient safety issues, CME offerings, residency programs, reports from clinical facility regarding new grads, upper level undergraduates instructor’s review of lower level student competencies, faculty recognition of clinical skills that students find difficult. Identification of coursework where simulation would be beneficial such as communication between team members, prioritizing care, or seldom seen clinical situations such as PP hemorrhage.
Sponsored Content:
Learning Objectives Creation: Learning objectives should match the learning need. Limit the number of objectives that can reasonably be addressed during the simulation time fram. Too many and too broad learning objectives will frustrate the learner and make assessment difficult.
Choice of simulation methodologies: Select a simulation methodology which will address the learning need. Include a theoretical framework as a basis for the simulation. Examples include adult learning theory or interprofessional education theories.
Fidelity: Fidelity is key for learners to immerse themselves in the simulation. Fidelity includes physical (or environmental) fidelity, conceptual fidelity ensures that all elements of the scenario or case relate to each other in a realistic way so that the case makes sense as a whole to the participant(s) and psychological fidelity maximizes the simulation environment by mimicking the contextual elements found in clinical environments.
Prebriefing and Debriefing: Determine pre-briefing exercises and debriefing methods.
Sponsored Content:
Simulation Evaluation: Create survey or evaluation for simulation.
Scenario Equipment and support documents. List needed equipment and props. Create supporting documents or electronic healthcare records such as prescribers order sheet, lab results or diagnostic reports.
Pilot Testing: INACSL recommends that all simulation scenarios are pilot tested! Creating effective healthcare simulation scenarios is a time consuming process. Content experts and/or faculty should review appropriate steps to ensure that content is accurate and addresses the learning objectives. Finally, educators experienced in simulation pedagogy should be part of the review team to advise appropriate scenario design.
Further Reading: INACSL Standards of Best Practice: Simulation Design – Simulation-based experiences are purposefully designed to meet identified objectives and optimize achievement of expected outcomes. Standardized simulation design provides a framework for developing effective simulation-based experiences. The design of simulation-based experiences incorporates best practices from adult learning, education, instructional design, clinical standards of care, evaluation, and simulation pedagogy. Purposeful simulation design promotes essential structure, process, and outcomes that are consistent with programmatic goals and/or institutional mission. The design of effective health care simulations facilitates consistent outcomes and strengthens the overall value of the simulation-based experience in all settings.
Download the Simulation Scenario Development Form Here!
Today’s article was guest authored by Kim Baily PhD, MSN, RN, CNE, previous Simulation Coordinator for Los Angeles Harbor College and Director of Nursing for El Camino College. Over the past 16 years Kim has developed and implemented several college simulation programs and previously chaired the Southern California Simulation Collaborative.
Have a story to share with the global healthcare simulation community? Submit your simulation news and resources here!
Dr. Kim Baily, MSN, PhD, RN, CNE has had a passion for healthcare simulation since she pulled her first sim man out of the closet and into the light in 2002. She has been a full-time educator and director of nursing and was responsible for building and implementing two nursing simulation programs at El Camino College and Pasadena City College in Southern California. Dr. Baily is a member of both INACSL and SSH. She serves as a consultant for emerging clinical simulation programs and has previously chaired Southern California Simulation Collaborative, which supports healthcare professionals working in healthcare simulation in both hospitals and academic institutions throughout Southern California. Dr. Baily has taught a variety of nursing and medical simulation-related courses in a variety of forums, such as on-site simulation in healthcare debriefing workshops and online courses. Since retiring from full time teaching, she has written over 100 healthcare simulation educational articles for HealthySimulation.com while traveling around the country via her RV out of California.
Sponsored Content: