Pediatric Simulation
Pediatric Simulation is the practice of using medical simulation products and tools to create an experience that represents the healthcare treatment of a child. Used to help teach and train learners and professionals alike, these simulations are intended to provide them with the skills and information needed to make decisions independently in the field. Clinical Simulation in pediatrics has been widely accepted and adapted as a training and assessment tool in medical education.
One advantage of using Pediatric Simulation is that learners are able to practice procedures and make errors without the risk of harming a physical patient. In this simulated environment, the trainees can have their errors corrected in real-time by an instructor, professor or training administrator. The quickness in receiving guided results and corrections helps users of the Pediatric Simulations to internalize what went wrong, how the error was corrected and how to avoid making that same error the next time the simulated situation arises.
Furthermore, there are so many different healthcare scenarios that can arise when treating pediatric patients. Having a pediatric simulator manikin can provide a comprehensive way for a learner to gain insight how to treat a wide variety of ailments, illnesses, conditions and diseases. Although each patient case may come with an individualized set of symptoms and concerns, guided Pediatric Simulation experiences can provide learners with enough information to make educated patient recommendations regarding treatments and medications.
Sponsored Content:
Considering these learning benefits, a number of colleges and universities across the United States and the world have adopted the use of Pediatric Simulation products for use in their simulation labs. Whereas the standard textbook and lecture style of learning presents healthcare concepts as they relate to pediatric patients in a 2-dimensional form, simulation is able to expand how learners work with course materials. For example, Pediatric Simulation creates the opportunity to move and manipulate a high fidelity patient simulator manikin so that all body parts can be clearly identified and observed. Following such simulated experiences, clinical educators will engage learners in a debriefing where the real learning takes place.
Another benefit of Pediatric Simulation products is that learners can practice performing tests, and be able to receive their test results quickly, if not in real-time. Again, the speed in performing simulations is much faster than having to bring in a test patient and wait until the laboratory returns the results. Speed and convenience both majorly assist in the learning process, as the experience will be fresher in their minds and thus the corrections and feedback more applicable, relatable and understandable.
HealthySimulation.com is dedicated to providing the latest Pediatric Simulation resources from around the world. To follow along, sign up for our free medical simulation email newsletter, follow @HealthySim on Twitter and @HealthySim on Facebook, or join our HealthySim LinkedIn Group!
Sponsored Content:
Lastly, Paediatric Simulation tools help prepare learners for the communication often necessary between a healthcare provider and a pediatric patient. Just as pediatric patients differ physical from adult patients, they also come with different emotional needs. Child Patient Simulators often have the ability to speak, hear, cry and make other noises to represent the emotional responses of pediatric patients.
Under these simulated circumstances, learners can determine the best ways to approach administering fluids to a pediatric patient, explaining treatments and interacting with them overall. While practicing treatments and procedures in a simulated environment is essential to prevent errors, simulating communication experiences is important to prevent creating emotional distress of a child.
A global community of pediatricians, pediatric subspecialists, pediatric nurses, educators and other allied health professionals, the International Pediatric Simulation Society (IPSS) strives to bring these knowledge and skills involved in simulation-based education, training and research in pediatric simulation to its global membership and symposium, workshop and meeting audience. Helping to spread awareness, the IPSS collects the titles of the most current publications on Pediatric Simulation from both the PubMed and CINAHL indexing systems to present them for the benefit of the simulation community.
Pediatric Simulator Examples
The company Laerdal, founded in 1940 and headquartered in Stavanger, Norway, produces a number of Simulated Patient products, including a Pediatric Simulation tool. The company’s other products vary based on age, gender and other factors which help learners to understand the specific needs of different types of patients. The Pediatric Simulation manikin offered by Laerdal is the Sim Junior.
SimJunior is an interactive pediatric simulator, designed by Laerdal with the American Academy of Pediatrics to ensure that the product meets the education and training needs of healthcare providers. SimJunior delivers a realistic, full-body simulator for pediatric emergencies, and closely represents the body of a 6-year-old boy. The simulation product allows learners to focus on a broad range of pediatric skills in order to gain exposure and practical experience of life-threatening pediatric problems.
Breathing features included with the SimJunior Manikin are that the product can simulate spontaneous breathing, has an observable chest rise, comes with variable respiratory rates and multiple upper airway sounds synchronized with breathing. Then, the SimJunior airway is anatomically modeled as far as the trachea and has a realistic airway with landmarks. This allows for oral and nasal intubation, LMA for ET insertion, tongue oedema, NG tube, cricoid cartilage and head tilt and jaw trusts without sensors.
Cardiac features included with the SimJunior are the capability for defibrillation and cardioversion, pacing, an extensive ECG library, multiple heart sounds synchronized with ECG, ECG rhythm monitoring (three leads) and a 12 lead ECG display. Furthermore, vascular access, circulation, heart, lung, bowel and patient voice sounds, a session viewer and patient monitor make this product increasingly realistic and useful in learning and educational scenarios.
Click Here to Connect to Leading Pediatric Simulator Vendors!
Then, Gaumard Scientific, a company headquartered in Miami, Fla., offers the Pediatric HAL. This pediatric simulator is capable of producing lifelike emotions through dynamic facial expressions, movement and speech. The product is designed to help providers of all levels to develop the specialized skills needed to effectively communicate, diagnose and treat young patients in nearly all clinical areas.
Other features of the Pediatric Manikin HAL include interactive eyes and dynamic lung compliance with true ventilator support. The tool additionally comes with real patient monitor support, including SpO2, EKG, capnography, NIBP, live pacing and defibrillation. Emergency intervention tools that come with the Pediatric HAL are emergency intervention: surgical airway, needle decompression and chest tube insertion. Lastly, the product is wireless and tether-less leading to an overall ease in use and general convenience. Events like SimGHOSTS, INACSL, IPSS, and SSH are great healthcare simulation conferences to see ped simulators in action!
Paediatric Simulation Latest News
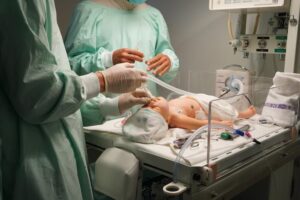
IPSSW Denver Conference Shares Leading Pediatric Simulation Expertise This May 7-9
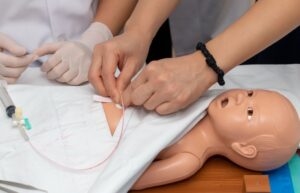
Three Scenarios to Improve Clinical Outcomes with Low Fidelity Pediatric Simulators

IPSSV 2023: Nov. 14th Virtual Online Symposium for Pediatric Simulation
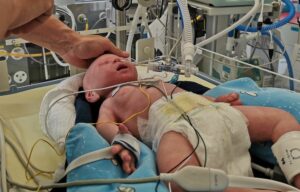
Neonatal Lung Simulator LuSi from neosim Creates Realistic Pediatric Ventilator Training

Pediatric Simulation Conference IPSSW 2023 Opens in Lisbon
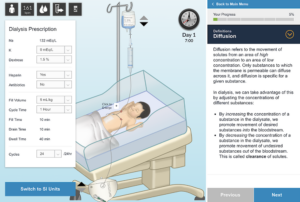
How OPENPediatrics Virtual Simulators Benefit Clinical Simulation Programs

Looking Ahead: 2023 Healthcare Simulation Events

IPSSV2022: Creating Safer Care Through Human Factors in Pediatric Simulation

IPSSV2022: Human Factors in Pediatric Simulation

HBO’s “Rehearsal” is Must-Watch TV for Healthcare Simulation Community

Healthcare Simulation Collaboration Establishes Mixed Reality Neonatal Training
Sponsored Content:

















